Chapter: Medicine and surgery: Gastrointestinal system
The acute abdomen introduction - GI presentations
GI presentations
The acute abdomen introduction
Patients with an acute abdomen are those with the following clinical presentation:
· Pain that may be local or more generalised.
· Tenderness to palpation with associated guarding (the reflex tensing of their abdominal wall musculature to prevent further pain on palpation).
· Rebound tenderness (pain worse on sudden release
of palpation, which is often more severe than on palpation).
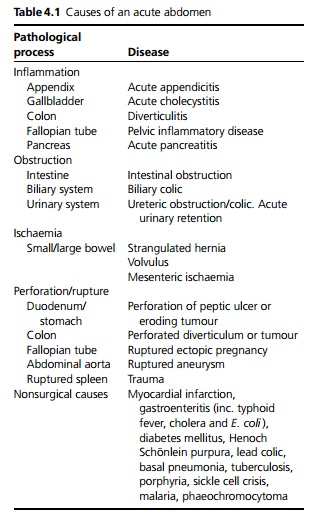
The patient is often generally unwell and may be shocked due to dehydration and loss of fluid into extravascular spaces such as the lumen of the bowel and the abdominal cavity. See Table 4.1 for causes.
Investigations
Full blood count (often normal, but leucocytosis may be present).
Urea and electrolytes, and liver function tests should be performed.
Serum amylase measurement is useful in diagnosing pancreatitis.
Urinalysis for sugar, ketones, protein, blood, bilirubin and urobilinogen.
Imaging: Erect chest X-ray, abdominal X-ray, ultra-sound or CT scan may be helpful.
Management
Patients may require resuscitation, and general management includes the following:
· Nil by mouth, nasogastric tube and i.v. fluids if vomiting, obstructed or perforated (drip and suck).
· If shocked, a fluid balance chart should be started and where appropriate urinary catheterisation to monitor output.
· Broad-spectrum antibiotics are often used.
· Subsequent management is directed at the underlying cause.
Related Topics