Chapter: Microbiology and Immunology: Bacteriology: Chlamydia and Chlamydophilaum
Chlamydophila
Chlamydophila
C. pneumoniae was first isolated from the conjunctiva of a childin Taiwan in 1965 and subsequently from throat of a patient with pharyngitis in 1983. These organisms were initially believed to be C. psittaci strains TWAR (from Taiwan acute respiratory),because they produced inclusion bodies in cell cultures similar to those produced by C. psittaci. Taiwan isolate was designated as TW-183, and the pharyngeal isolate was designated as AR-9. These two strains were initially believed to be related to psittaci strains, but later on were found to be different. These two organ-isms were then classified as Chlamydia pneumoniae but now have been reclassified and finally placed in a new genus Chlamydophila.
Chlamydophila pneumonia
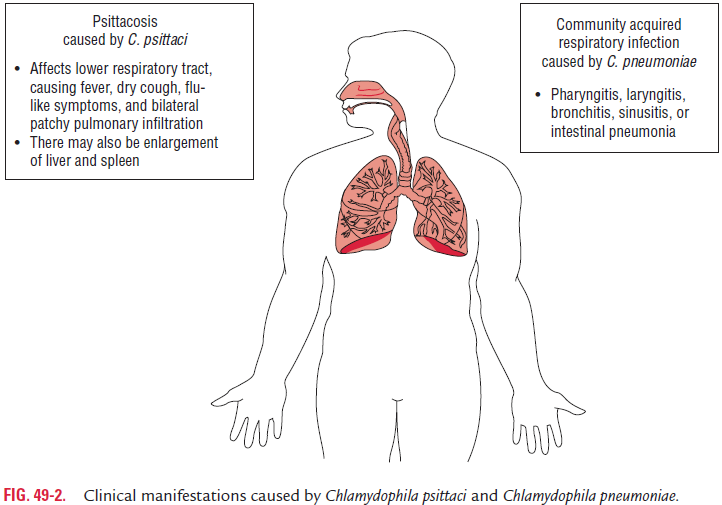
C. pneumoniae is the third common cause of pneumonia follow-ing Streptococcus pneumoniae and Haemophilus influenzae. It is an important cause of respiratory disease in older children and adults worldwide. C. pneumoniae causes mostly asymptomatic infections. Pharyngitis, sinusitis, bronchitis, and pneumonia are the common manifestations of symptomatic cases in severe respiratory tract infection.
C. pneumoniae is also a strict human pathogen and does nothave any animal reservoir. Infection is transmitted by respira-tory secretions from person to person without any avian or animal host. Approximately, 2–3 lakh cases of C. pneumoniae occur every year, and most of these cases occur in adults.
Diagnosis of infection is made by demonstration of C.pneumoniae antigen in specimens by enzyme immunoassay orDFA test. Diagnosis by culture is not done as C. pneumoniae grows poorly in cell cultures. Serodiagnosis is carried out by using CFT, ELISA, or MIF. Antibodies have been demonstrated in sera of more than 50% of people. PCR is also used to detect bacterial genome in the specimen.
Tetracycline, doxycycline, erythromycin, and azithromy-cin are given for 10–14 days for treatment of C. pneumoniae infection. Control of C. pneumoniae infection is difficult.
Chlamydophila psittaci
C. psittaci is the causative agent of psittacosis, a disease ofparrots and psittacine birds which can be transmitted to humans. The disease was first observed in parrots, hence named psittacosis (Greek word psittakos means parrot). A similar disease of nonpsittacine birds was called ornithosis (Greek word ornithos means bird). Now both the conditions are called psittacosis.
Infection in birds may occur as asymptomatic or symp-tomatic. Symptomatic infection may manifest as respiratory infection, diarrhea, and emaciation. In the infected birds, the bacteria are present in the blood, tissue, and feathers and are also excreted in the feces, nasal discharges, aerosols, etc.
C. psittaci can be transmitted from birds to humans as wellas sheep, cows, and goat. Humans acquire the infection mostly from psittacine birds, such as parrots, parakeets, cockatiels, and macaws. They get infected by inhalation of dried bird drop-pings, urine, or respiratory secretions of these infected birds.
Human infections are mostly occupational, and veteri-narians, poultry workers, pet-shop workers, pigeon farmers, etc. are at increased risk for this infection. Person-to-person transmission is rare. Ingestion of poultry birds also does not cause any infection. Laboratory infection is well documented.
C. psittaci in humans causes a clinical syndrome, which var-ies from a mild influenza-like illness to a fatal pneumonia. Incubation period varies from 5 to 14 days. Headache, high fever, chills, malaise, and myalgia are the symptoms at the initial stage of the illness. Nonproductive cough, rales, and con-solidation are the respiratory manifestations. The untreated cases may be severe and progress to encephalitis, endocarditis, pericarditis, and even death (Fig. 49-2).
Laboratory diagnosis of the condition is based mainly on the serological tests. Demonstration of a fourfold rise in antibody titer in the paired acute and convalescent sera by the CFT is suggestive of C. psittaci infection. MIF test is a specific test used to confirm the diagnosis.
Levinthal-Cole-Lille (LCL) inclusion bodies:These are demon-strated in mouse brain, yolk sac, cell cultures, and in infected cells including alveolar macrophages from patients suffering from C. psittaci infection. These inclusion bodies are not stained by iodine, and are more diffuse and irregular. They are not inhibited by sulfadiazine or cycloserine. C. psittaci can be grown in cell cultures, such as L cells after 5–10 days of incubation, but is not used routinely.
Tetracycline, doxycycline, erythromycin, and azithromy-cin are useful for treatment of C. psittaci infection. Infection is prevented by controlling it in birds.
Related Topics