Chapter: Pathology: Central Nervous System Pathology
CNS Trauma And Herniations
CNS TRAUMA AND HERNIATIONS
Cranial Cavity and Brain
Concussion is mild traumatic brain injury with a transient
loss of brain function. The trauma is commonly due to
a change in the momentum of the head (impact against a rigid surface).
Concussion causes loss of consciousness and reflexes, tem-porary respiratory
arrest, and amnesia for the event. The pathogenesis is uncertain. Parenchymal
injuries may or may not be evident at autopsy
Contusions are bruises of the brain tissue. Common sites
of injury include crests of orbital gyri in frontal and
temporal poles, in addition to coup
(site of injury) and contrecoup (site
diametrically opposite) injuries. Coup and contrecoup develop when the head is mobile at the time of
impact.
•
Acute
contusion is characterized by hemorrhage of brain tissue in a wedge-shaped
area.
•
Subacute
contusion shows necrosis and liquefaction of brain.
•
Remote
contusion causes a depressed area of cortex with yellow discoloration (“plaque
jaune”).

Epidural hematoma
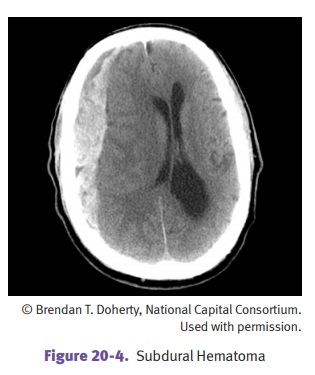
Subdural hematoma is caused by the rupture of
bridging veins (from the cerebral convexities to the sagittal
sinus); it is usually traumatic in older individuals. Pre-disposing conditions
include brain atrophy (due simply to aging) and abnormal hemostatis. Symptoms
include headache, drowsiness, focal neurological deficits, and sometimes
dementia. It recurs frequently.
Diffuse
axonal injury refers to damage to axons at nodes of Ranvier with impairment of axoplasmic flow. It causes
coma after trauma without evidence of direct paren-chymal injuries. There is a
poor prognosis, related to duration of coma. The injury to the white matter is
due to acceleration/deceleration forces with shearing of axons.
The histopathology shows
axonal swellings appreciable in the white matter. It is dif-fuse, but with a
predilection for the corpus callosum, periventricular white matter, and
hippocampus, as well as cerebral and cerebellar peduncles.
Spinal cord injuries are usually traumatic, due to
vertebral displacement. Symptom-atology depends on the interruption of
ascending and descending tracts.
•
Lesions to thoracic segments or below cause paraplegia.
•
Lesions to cervical segments cause tetraplegia.
•
Lesions above C4 cause respiratory arrest due to paralysis of the
diaphragm.
Chronic traumatic encephalopathy is a neurodegenerative
disorder that occurs years or decades after a sports
career with repetitive brain trauma. Neuropathological changes include
neurofibrillary tangles, cerebellar atrophy and gliosis, hypopigmen-tation of
the substantia nigra, and cavum septum pellucidum.
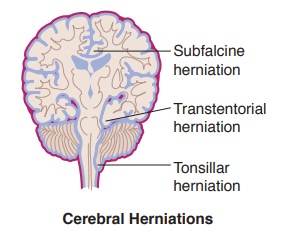
Cerebral Herniations
Subfalcine (cingulate gyrus) herniation occurs when the cingulate
gyrus is displaced underneath the falx to the
opposite side. Compression of the anterior cerebral artery can occur.
Transtentorial (uncal) herniation occurs when the uncus of the
temporal lobe is dis-placed over the free edge of the tentorium. Clinical
features include compression of the third nerve, ipsilateral pupillary
dilatation, and infarction of the tissue supplied by the posterior cerebral
artery. Advanced stages of transtentorial herniation can cause Duret
hemorrhages within the central pons and midbrain.
Cerebellar tonsillar herniation occurs when there is
displacement of cerebellar ton-sils through the foramen magnum. Compression of
the medulla may lead to car-diorespiratory arrest.
Related Topics