Chapter: Medical Physiology: Cardiac Arrhythmias and Their Electrocardiographic Interpretation
Atrial Fibrillation
Atrial Fibrillation
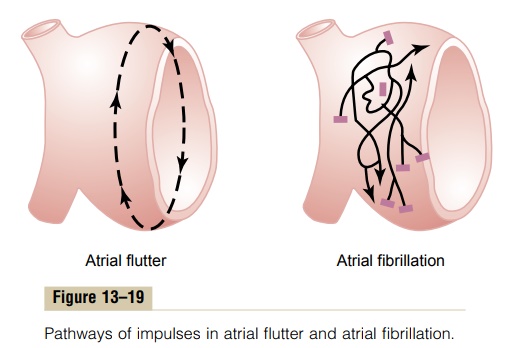
Remember that except for the conducting pathway through the A-V bundle, the atrial muscle mass is separated from the ventricular muscle mass by fibrous tissue. Therefore, ventricular fibrillation often occurs without atrial fibrillation. Likewise, fibrillation often occurs in the atria without ventricular fibrillation (shown to the right in Figure 13–19).
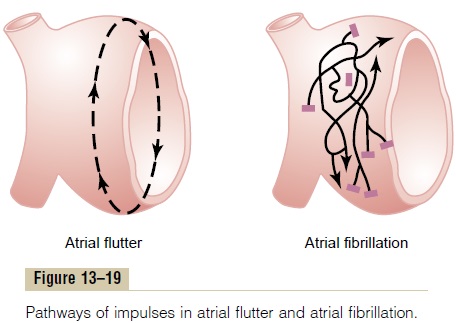
The mechanism of atrial fibrillation is identical to that of ventricular fibrillation, except that the process occurs only in the atrial muscle mass instead of the ventricular mass. A frequent cause of atrial fibrillation is atrial enlargement resulting from heart valve lesions that prevent the atria from emptying adequately into the ventricles, or from ventricular failure with excess damming of blood in the atria. The dilated atrial walls provide ideal conditions of a long conductive pathway as well as slow conduction, both of which predispose to atrial fibrillation.
Pumping Characteristics of the Atria During Atrial Fibrillation.
For the same reasons that the ventricles will not pump blood during ventricular fibrillation, neither do the atria pump blood in atrial fibrillation. Therefore, the atria become useless as primer pumps for the ventricles. Even so, blood flows passively through the atria into the ventricles, and the efficiency of ventricular pumping is decreased only 20 to 30 per cent. Therefore, in contrast to the lethality of ventricular fibrillation, a person can live for months or even years with atrial fibrillation, although at reduced efficiency of overall heart pumping.
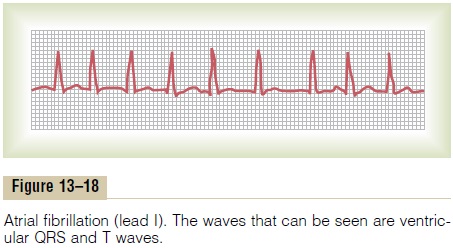
Electrocar diogram in Atrial Fibrillation. Figure 13–18 showsthe electrocardiogram during atrial fibrillation. Numer-ous small depolarization waves spread in all directions through the atria during atrial fibrillation. Because the waves are weak and many of them are of opposite polarity at any given time, they usually almost com-pletely electrically neutralize one another. Therefore, in the electrocardiogram, one can see either no P waves from the atria or only a fine, high-frequency, very low voltage wavy record. Conversely, the QRS-T complexes are normal unless there is some pathology of the ven-tricles, but their timing is irregular, as explained next.
Irregularity of Ventricular Rhythm During Atrial Fibrillation.
When the atria are fibrillating, impulses arrive from the atrial muscle at the A-V node rapidly but also irregu-larly. Because the A-V node will not pass a second impulse for about 0.35 second after a previous one, at least 0.35 second must elapse between one ventricular contraction and the next.
Then an additional but variable interval of 0 to 0.6 second occurs before one of the irregular atrial fibrillatory impulses happens to arrive at the A-V node. Thus, the interval between suc-cessive ventricular contractions varies from a minimum of about 0.35 second to a maximum of about 0.95 second, causing a very irregular heartbeat. In fact, this irregularity, demonstrated by the variable spacing of the heartbeats in the electrocardiogram of Figure 13–18, is one of the clinical findings used to diagnose the condi-tion. Also, because of the rapid rate of the fibrillatory impulses in the atria, the ventricle is driven at a fast heart rate, usually between 125 and 150 beats per minute.
Electroshock Treatment of Atrial Fibrillation. In the samemanner that ventricular fibrillation can be converted back to a normal rhythm by electroshock, so too can atrial fibrillation be converted by electroshock. The pro-cedure is essentially the same as for ventricular fibrilla-tion conversion—passage of a single strong electric shock through the heart, which throws the entire heart into refractoriness for a few seconds; a normal rhythm often follows if the heart is capable of this.
Related Topics