Chapter: Essentials of Anatomy and Physiology: Lymphatic System and Immunity
Anatomy of the Lymphatic System
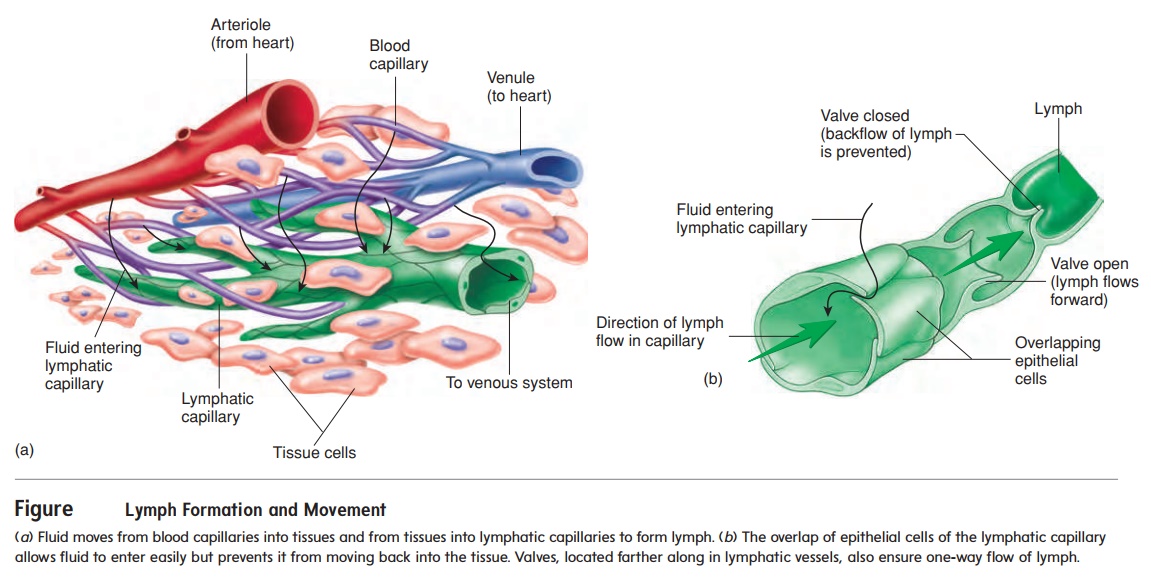
ANATOMY OF THE LYMPHATIC SYSTEM
Lymphatic capillaries and Vessels
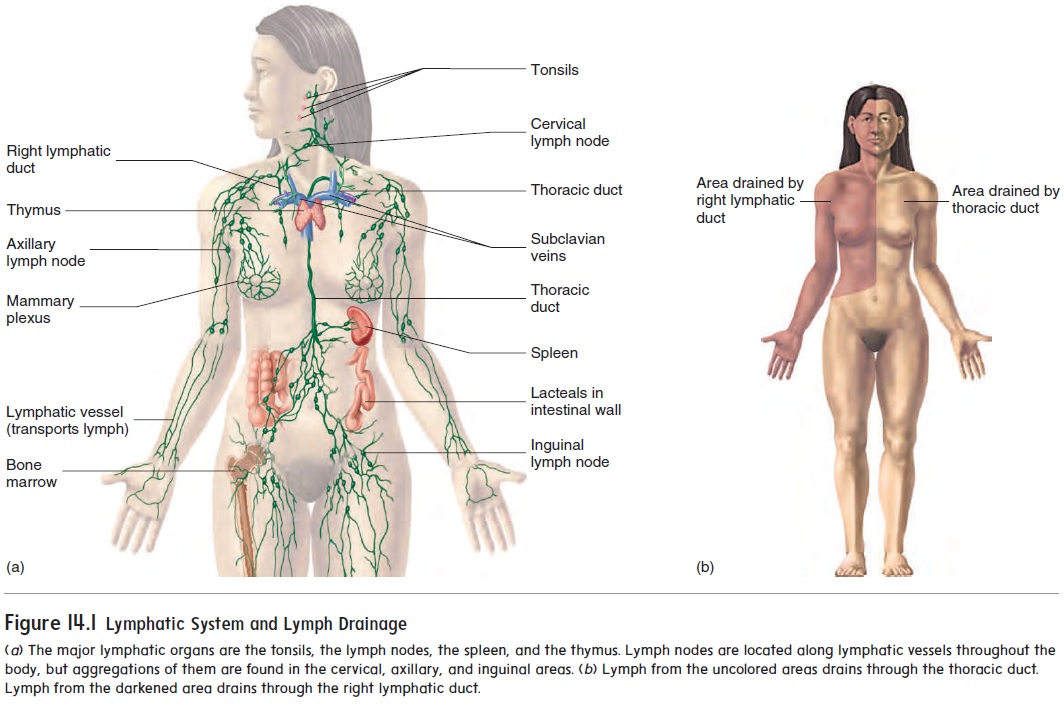
The lymphatic system includes lymph, lymphocytes, lymphatic vessels, lymph nodes, the tonsils, the spleen, and the thymus (fig-ure 14.1a). The lymphatic system, unlike the circulatory system, does not circulate fluid to and from tissues. Instead, the lymphatic system carries fluid in one direction, from tissues to the circulatorysystem. Fluid moves from blood capillaries into tissue spaces (see figure 13.24). Most of the fluid returns to the blood, but some of the fluid moves from the tissue spaces into lymphatic capillaries to become lymph (figure 14.2a). The lymphatic capillaries are tiny, closed-ended vessels consisting of simple squamous epithelium. The lymphatic capillaries are more permeable than blood capillaries because they lack a basement membrane, and fluid moves easily into them. Overlapping squamous cells of the lymphatic capillary walls act as valves that prevent the backflow of fluid (figure 14.2b). After fluid enters lymphatic capillaries, it flows through them.
Lymphatic capillaries are present in most tissues of the body. Exceptions are the central nervous system, bone marrow, and tis-sues lacking blood vessels, such as the epidermis and cartilage. A superficial group of lymphatic capillaries drains the dermis and subcutaneous tissue, and a deep group drains muscle, the viscera, and other deep structures.
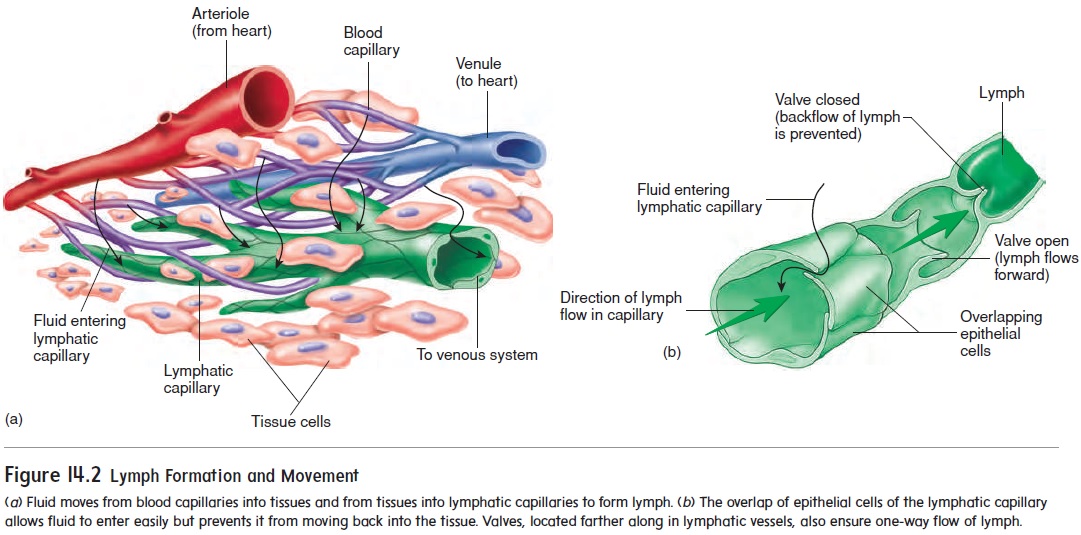
The lymphatic capillaries join to form larger lymphaticvessels, which resemble small veins (figure 14.2b). Small lym-phatic vessels have a beaded appearance because they have one-way valves that are similar to the valves of veins . When a lymphatic vessel is compressed, the valves prevent backward movement of lymph. Consequently, compression of the lymphatic vessels causes lymph to move forward through them. Three fac-tors cause compression of the lymphatic vessels: (1) contraction of surrounding skeletal muscle during activity, (2) periodic contraction of smooth muscle in the lymphatic vessel wall, and (3) pressure changes in the thorax during breathing.
The lymphatic vessels converge and eventually empty into the blood at two locations in the body. Lymphatic vessels from the right upper limb and the right half of the head, neck, and chest form the right lymphatic duct, which empties into the right sub-clavian vein. Lymphatic vessels from the rest of the body enter the thoracic duct, which empties into the left subclavian vein (seefigure 14.1b).
Lymphatic organs
The lymphatic organs include the tonsils, the lymph nodes, the spleen, and the thymus. Lymphatic tissue, which consists of many lymphocytes and other cells, such as macrophages, is found within lymphatic organs. The lymphocytes originate from red bone marrow and are carried by the blood to lymphatic organs. These lymphocytes divide and increase in number when the body is exposed to pathogens. The increased number of lym-phocytes is part of the immune response that causes the destruc-tion of pathogens. In addition to cells, lymphatic tissue has very fine reticular fibers . These fibers form an interlaced network that holds the lymphocytes and other cells in place. When lymph or blood filters through lymphatic organs, the fiber network also traps microorganisms and other items in the fluid.
Tonsils
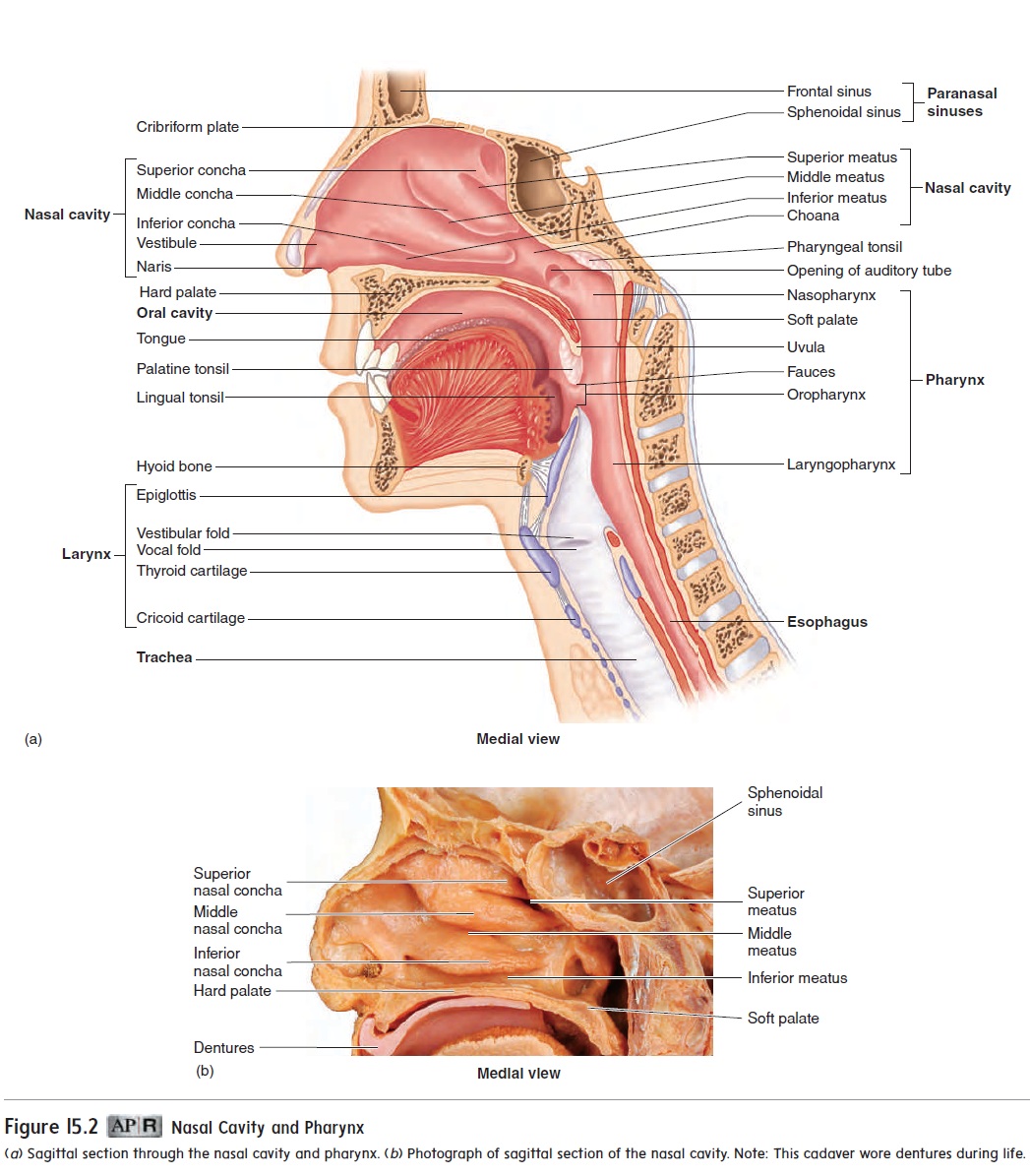
There are three groups of tonsils (figure 14.3; see figure 15.2). The palatine (pal′ ă-tı̄n; palate) tonsils are located on each side of the posterior opening of the oral cavity; these are the ones usually referred to as “the tonsils.” The pharyngeal (fă-rin′ jē-ăl) tonsil is located near the internal opening of the nasal cavity. When thepharyngeal tonsil is enlarged, it is commonly called the adenoid (ad′ ĕ-noid), or adenoids. An enlarged pharyngeal tonsil can inter- fere with normal breathing. The lingual (ling′ gwăl; tongue) tonsil is on the posterior surface of the tongue.
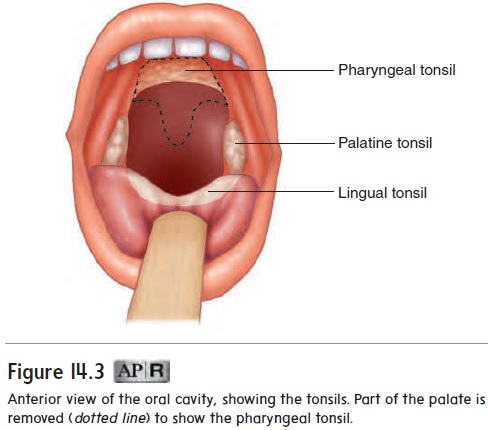
The tonsils form a protective ring of lymphatic tissue around the openings between the nasal and oral cavities and the pharynx. They protect against pathogens and other potentially harmful material entering from the nose and mouth. Sometimes the palatine or pharyngeal tonsils become chronically infected and must be removed. The lingual tonsil becomes infected less often than the decrease in size and may eventually disappear.
Lymph Nodes
Lymph nodes are rounded structures, varying from the size of asmall seed to that of a shelled almond. Lymph nodes are distrib-uted along the various lymphatic vessels (see figure 14.1a), and most lymph passes through at least one lymph node before enter-ing the blood. Although lymph nodes are found throughout the body, there are three superficial aggregations of lymph nodes on each side of the body: inguinal nodes in the groin, axillary nodes in the axilla (armpit), and cervical nodes in the neck.
A dense connective tissue capsule surrounds each lymph node (figure 14.4). Extensions of the capsule, called trabeculae, subdivide a lymph node into compartments containing lymphatic tissue and lymphatic sinuses. The lymphatic tissue consists of lymphocytes and other cells that can form dense aggregations of tissue calledlymphatic nodules. Lymphatic sinuses are spaces between the lym-phatic tissue that contain macrophages on a network of fibers. Lymph enters the lymph node through afferent vessels, passes through the lymphatic tissue and sinuses, and exits through efferent vessels.
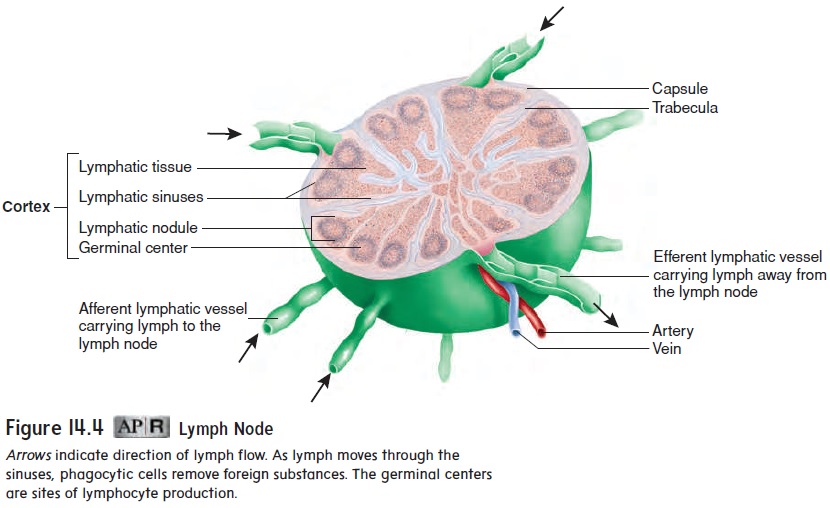
As lymph moves through the lymph nodes, two functions are performed. One function is to activate the immune system. Pathogens in the lymph can stimulate lymphocytes in the lymphatic tissue to divide. The lymphatic nodules containing the rapidly divid-ing lymphocytes are called germinal centers. The newly produced lymphocytes are released into the lymph and eventually reach the blood, where they circulate and enter other lymphatic tissues. The lymphocytes are part of the adaptive immune response (see “Adaptive Immunity” later that destroys pathogens. The second function of the lymph nodes is to remove pathogens from the lymph through the action of macrophages.
Spleen
The spleen (splēn) is roughly the size of a clenched fist and is located in the left, superior corner of the abdominal cavity (fig-ure 14.5). The spleen has an outer capsule of dense connective tissue and a small amount of smooth muscle. Trabeculae from the capsule divide the spleen into small, interconnected compartments containing two specialized types of lymphatic tissue. White pulp is lymphatic tissue surrounding the arteries within the spleen. Redpulp is associated with the veins. It consists of a fibrous network,filled with macrophages and red blood cells, and enlarged capillar-ies that connect to the veins.
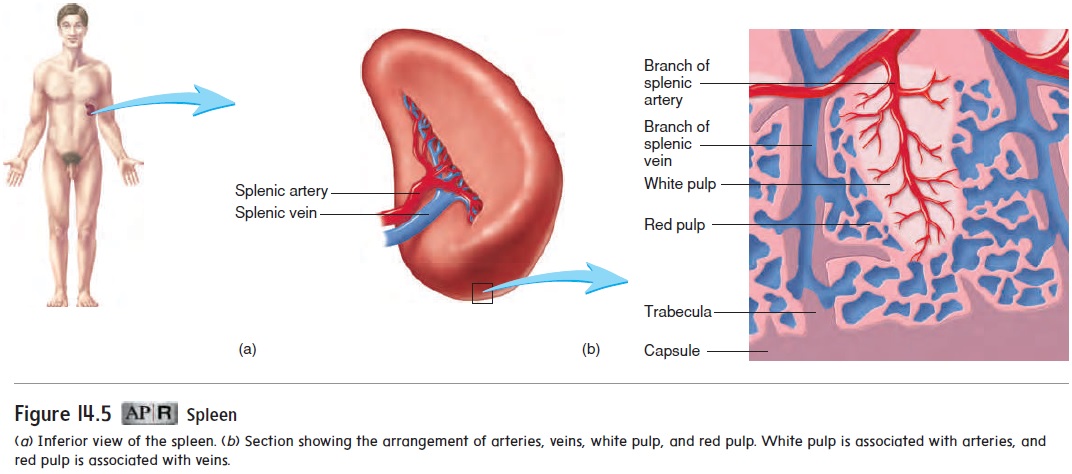
The spleen filters blood instead of lymph. Cells within the spleen detect and respond to foreign substances in the blood and destroy worn-out red blood cells. Lymphocytes in the white pulp can be stimulated in the same manner as in lymph nodes. Before blood leaves the spleen through veins, it passes through the red pulp. Macrophages in the red pulp remove foreign substances and worn-out red blood cells through phagocytosis.
The spleen also functions as a blood reservoir, holding a small volume of blood. In emergency situations, such as hemorrhage, smooth muscle in splenic blood vessels and in the splenic capsule can contract, allowing a small amount of blood to move out of the spleen into the general circulation.
Thymus
The thymus (thi′ m̆u s) is a bilobed gland roughly triangular in shape (figure 14.6a). It is located in the superior mediastinum, the partition dividing the thoracic cavity into left and right parts. Each lobe of the thymus is surrounded by a thin connective tissue capsule. Trabeculae from the capsule divide each lobe into lobules (figure 14.6b). Near the capsule and trabeculae, the lymphocytes are numerous and form dark-staining areas called the cortex. A lighter-staining, central portion of the lobules, called the medulla, has fewer lymphocytes.
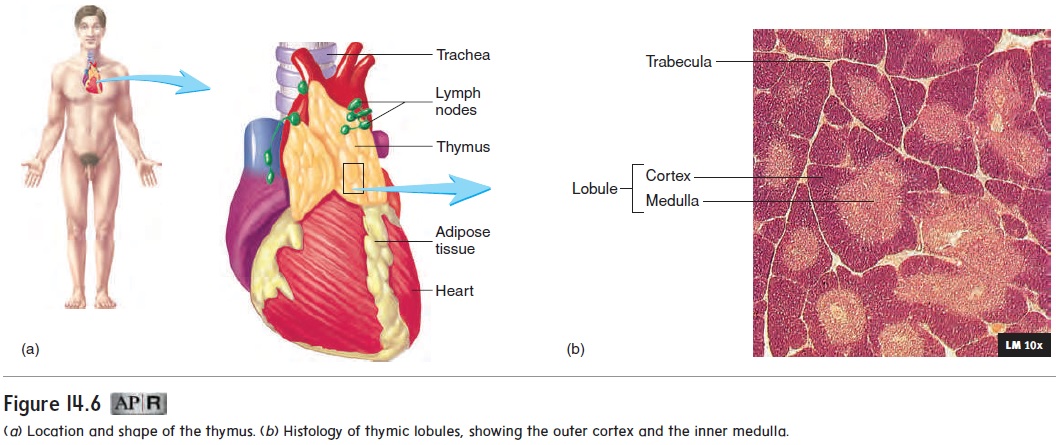
The thymus is the site for the maturation of a class of lym-phocytes called T cells (described in “Adaptive Immunity” later). Large numbers of T cells are produced in the thymus, but most degenerate. The T cells that survive the matura-tion process are capable of reacting to foreign substances. The mature T cells migrate to the medulla, enter the blood, and travel to other lymphatic tissues, where they help protect against patho-gens. Production of T cells declines later in life due to decreased function of the thymus (see “Effects of Aging on the Lymphatic System and Immunity” later).
Overview of The Lymphatic System
Figure 14.7 summarizes the processes performed by the lymphatic system. Lymphatic capillaries and vessels remove fluid from tissues and absorb lipids from the small intestine. Lymph nodes filter lymph, and the spleen filters blood.
Figure 14.7 also illustrates two types of lymphocytes, called B cells and T cells. B cells originate and mature in red bone mar-row. Pre-T cells are produced in red bone marrow and migrate to the thymus, where they mature to become T cells. B cells from red bone marrow and T cells from the thymus circulate to, and populate, other lymphatic tissues.
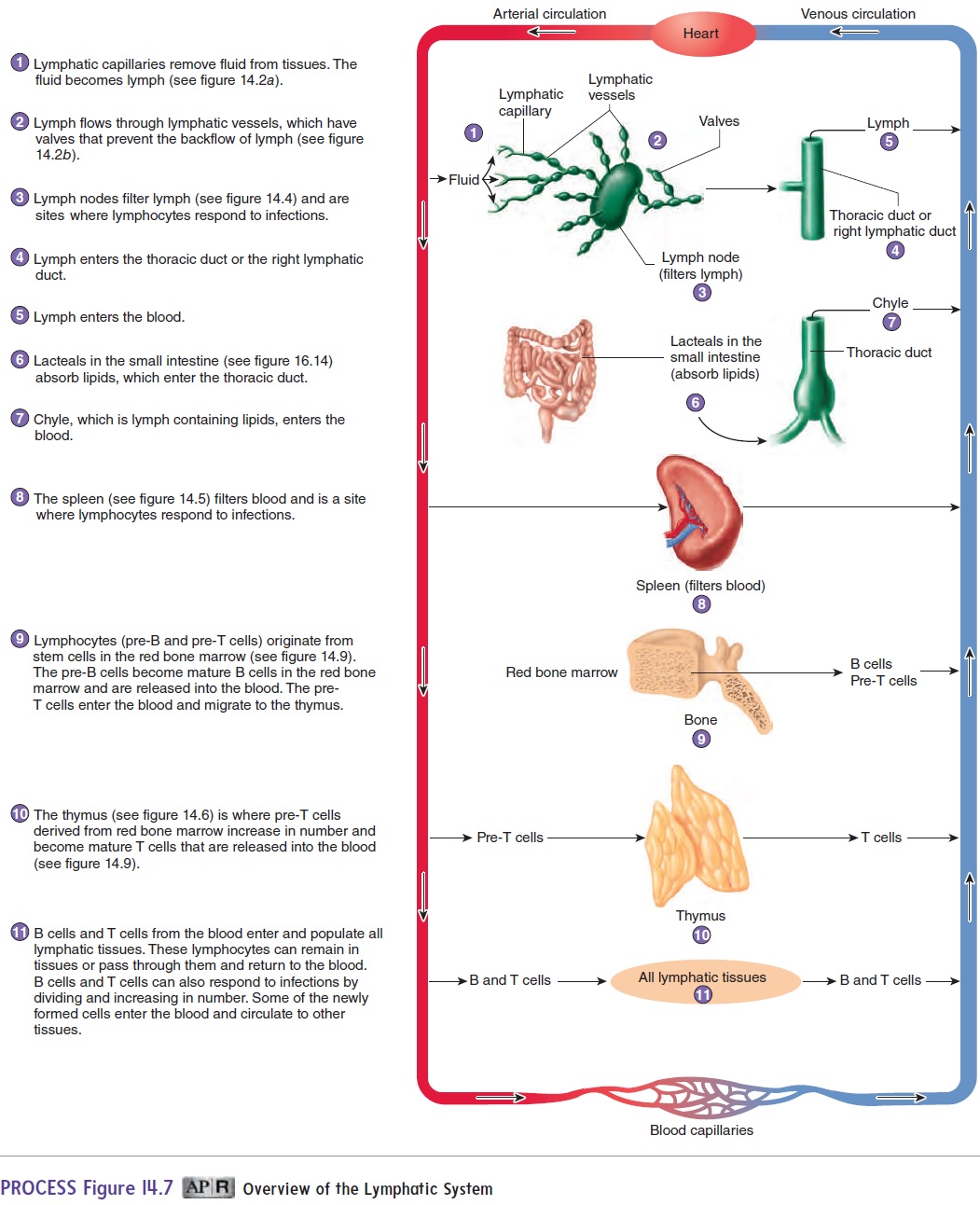
B cells and T cells are responsible for much of immunity. In response to infections, B cells and T cells increase in number and cir-culate to lymphatic and other tissues. How B cells and T cells protect the body is discussed laterr (see “Adaptive Immunity”).
Related Topics