Chapter: The Massage Connection ANATOMY AND PHYSIOLOGY : Digestive System
Wall of the Digestive Tract
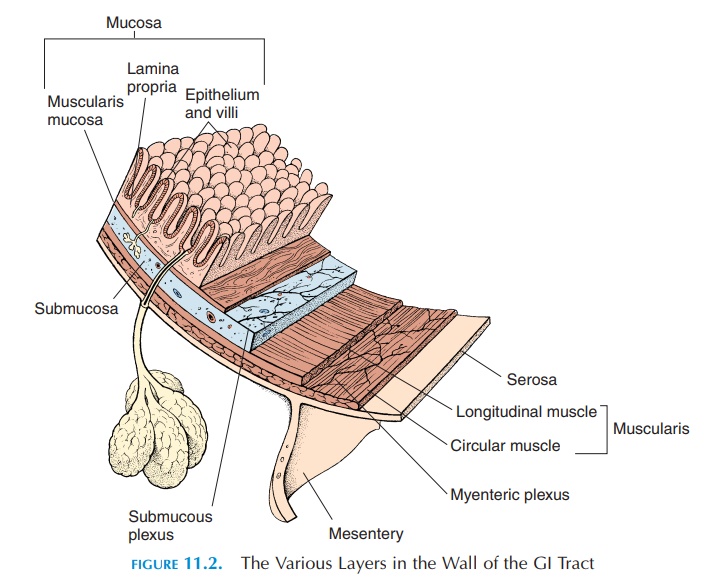
Wall of the Digestive Tract
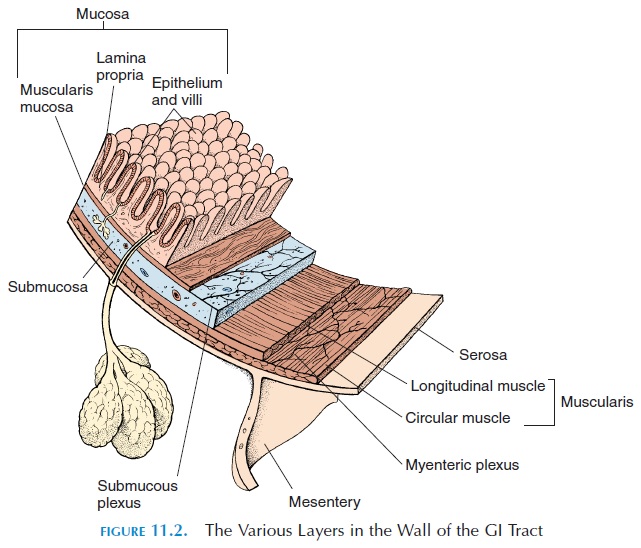
The wall of the digestive tract (see Figure 11.2) has four layers—deep to superficial (i.e., from the lumen to the outer surface of the gut)—the mucosa, sub-mucosa, muscularis, and serosa.
MUCOSA
The layer surrounding the lumen is the mucosa. The mucosa consists of single layer of epithelium, a sup-portive connective tissue layer (lamina propria), and a thin, muscle layer (muscularis mucosae). The type of lining epithelium varies from region to region ac-cording to function. In areas where this is a likelihood of excessive friction and injury, the epithelium is nonkeratinized, stratified squamous (flat, pavement-like). This type of epithelium is found in the mouth, pharynx, esophagus, and the anus. In areas where ab-sorption or secretion must occur, the epithelium is a simple, columnar type. Most of the gut has this type of epithelium. Scattered between the columnar ep-ithelial cells are exocrine cells (goblet cells) that se-crete mucus into the lumen and endocrine cells (en-teroendocrine cells) that secrete hormones into theblood. To increase efficiency, the epithelium is thrown into folds called villi in regions where absorption takes place. The folds also allow for expansion when a large meal is ingested. The individual epithelial cells also have folds on the surface facing the lumen known as microvilli. The presence of microvilli increases the surface area by 20% and helps improve absorption of nutrients. The epithelium proliferates rapidly and is replaced every 5 to 7 days.
The lamina propria consists of connective tissue. In some areas, this connective tissue contains glands, which open into the lumen and secrete the enzymes and fluids required for digestion. The lamina propria also has nerve endings, blood vessels, and lymphoid tissue. The lymphoid tissue, consisting of lympho-cytes and macrophages, protects the GI tract from entry of microorganisms. Some smooth muscle—the muscularis mucosae—is also seen in the lamina pro-pria. Muscle contraction causes the mucosa to be thrown into folds that increase surface area for se-cretion and absorption and ensure that the contents of the GI tract come in better contact with the ab-sorptive surface.
Glands not located in the digestive tract also se-crete enzymes and fluids. These secretions are ex-pelled into the lumen by ducts that carry the secre-tion from the glands.
SUBMUCOSA
Outside the lamina propria and its muscles, lies the submucosa. This, too, is a connective tissue layer containing large nerves and blood vessels. The nerves form a network known as the submucous plexus, comprised of both parasympathetic and sympathetic fibers. The parasympathetic fibers stimulate muscle tone and activity and increase glandular secretions. The sympathetic fibers relax the muscles and reduce secretions. However, the circular muscles controlling the openings—the sphincter muscles—are stimulated by the sympathetics.
MUSCULARIS
Just external to the submucosa is another layer of muscles, the muscularis externa. The muscularis externa consists of inner circular and outer longitudinal smooth muscle.
Sandwiched between the circu-lar and longitudinal muscle layers is another network of autonomic (sympathetic and parasympathetic) fibers, themyenteric plexus.
The mouth, pharynx, and superior and middle part of the esophagus have skeletal muscle that helps to vol-untarily control swallowing. The anus also has skeletal muscle that helps voluntarily control defecation.
SEROSA
Outside the muscularis externa is a connective tissue layer, the serosa. In those parts of the gut in the ab-domen, the serosa is the smooth membrane known as the peritoneum. In the oral cavity, pharynx, esophagus, rectum, and anus, the serosa is the connective tissue that attaches the part to the surrounding region.
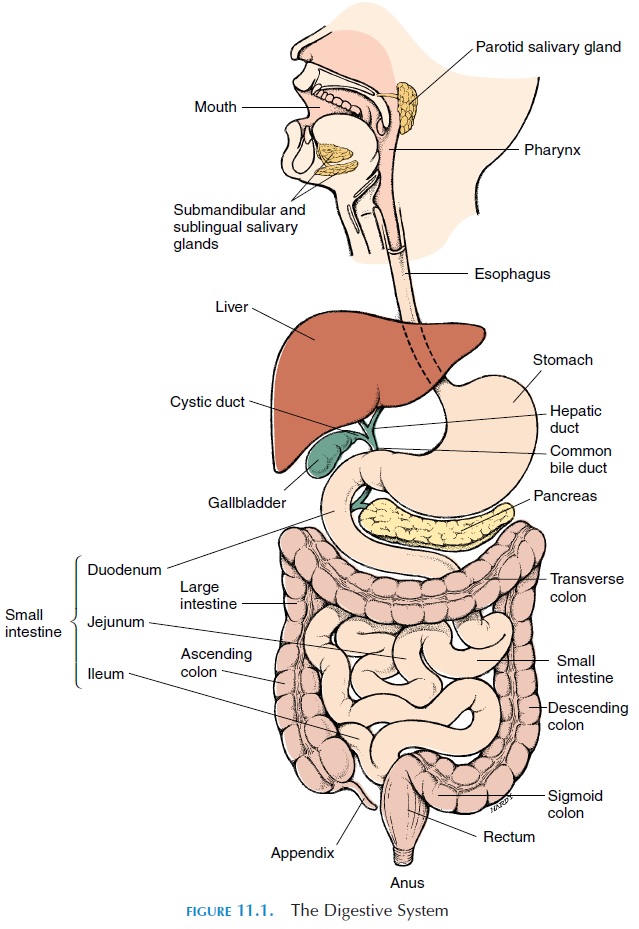
Related Topics