Chapter: Basic & Clinical Pharmacology : Management of the Poisoned Patient
Toxic Syndromes: Cholinesterase Inhibitors
CHOLINESTERASE INHIBITORS
Organophosphate and carbamate cholinesterase inhibitors are widely used to kill insects and other pests. Most cases of serious organophosphate or carbamate poisoning result from intentional ingestion by a suicidal person, but poisoning has also occurred at work (pesticide application or packaging) or, rarely, as a result of food contamination or terrorist attack (eg, release of the chemical warfare nerve agent sarin in the Tokyo subway system in 1995).
Stimulation of muscarinic receptors causes abdominal cramps, diarrhea, excessive salivation, sweating, urinary frequency, and increased bronchial secretions. Stimulation of nicotinic receptors causes generalized ganglionic activation, which can lead to hypertension and either tachycardia or brady-cardia. Muscle twitching and fasciculations may progress to weak-ness and respiratory muscle paralysis. CNS effects include agitation, confusion, and seizures. The mnemonic DUMBELS (diarrhea, urination, miosis and muscle weakness, bronchospasm, excitation, lacrimation, and seizures, sweating, and salivation) helps recall the common findings. Blood testing may be used to document depressed activity of red blood cell (acetylcholinest-erase) and plasma (butyrylcholinesterase) enzymes, which provide an indirect estimate of synaptic cholinesterase activity.
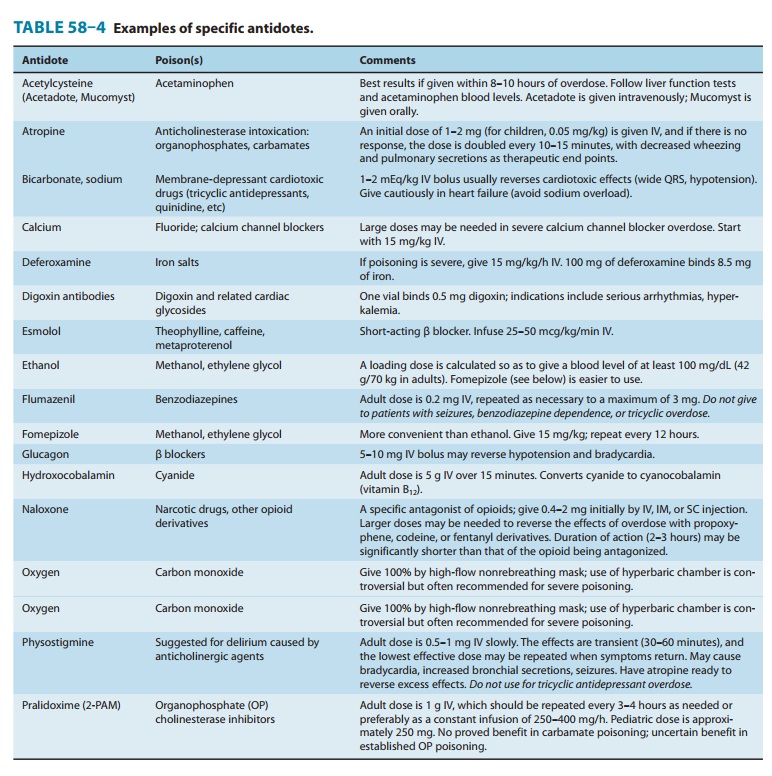
General supportive care should be provided as outlined above. Precautions should be taken to ensure that rescuers and health care providers are not poisoned themselves by exposure to contami-nated clothing or skin. This is especially critical for the most potent substances such as parathion or nerve gas agents. Antidotal treatment consists of atropine and pralidoxime (see Table 58–4). Atropine is an effective competitive inhibitor at muscarinic sites but has no effect at nicotinic sites. Pralidoxime given early enough may be capable of restoring the cholinesterase activity and is active at both muscarinic and nicotinic sites.
Related Topics