Chapter: Modern Pharmacology with Clinical Applications: Diuretic Drugs
Thiazide Diuretics
Thiazide Diuretics
Thiazide diuretics consist of
two distinct groups: those containing a benzothiadiazine ring, such as
hydro-chlorothiazide and chlorothiazide, referred to as thiazide diuretics, and
those that lack this heterocyclic structure but contain an unsubstituted
sulfonamide group. The lat-ter are called thiazidelike diuretics; they include
metola-zone, xipamide, and indapamide. The major thiazide and thiazidelike
drugs available in the United States are bendroflumethiazide, benzthiazide,
chlorothiazide, hy-drochlorothiazide, hydroflumethiazide, methyclothiazide,
polythiazide, and trichlormethiazide; and chlorthalidone, indapamide,
metolazone, and quinethazone, respectively.
Despite the structural
distinctions, the drugs share the functional attribute of increasing sodium and
chlo-ride excretion by inhibiting NA+ –Cl- cotransport in
dis-tal convoluted tubules.
Although chlorothiazide and
its subsequently devel-oped congeners (Table 21.2) retain the sulfamyl group SO2NH2,
which is necessary for carbonic anhydrase in-hibition, their primary effect
does not rely on carbonic anhydrase inhibition.
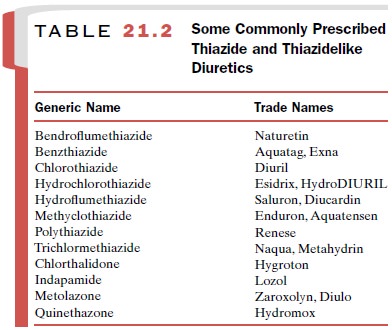
The thiazidelike compounds,
including chlorthali-done (Hygroton),
quinethazone (Hydromox), and
metolazone (Zaroxolyn) have similar
mechanisms of action, but they differ substantially from one another in their
duration of action, the degree of carbonic anhy-drase inhibition, and the dose
required for maximum natriuretic activity.
Mechanism of Action
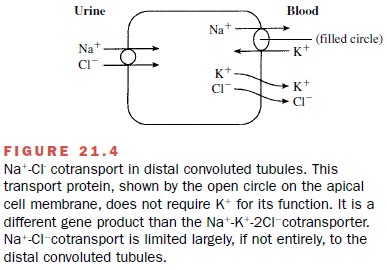
Thiazide diuretics act in the distal convoluted tubule, where they
block NA+ –Cl- cotransport (Fig. 21.4). The NA+ –Cl- cotransport
takes place on the luminal surface of distal convoluted tubules. Thus, to exert
their diuretic action, the thiazides must reach the luminal fluid. Since the
thiazide diuretics are largely bound to plasma pro-teins and therefore are not
readily filtered across the glomeruli, access to the luminal fluid is
accomplished by the proximal tubule organic acid secretory system. The drugs
then travel along the nephron, presumably being concentrated as fluid is
abstracted, until they reach their site of inhibitory action in the distal
convoluted tubule.
Especially at higher doses,
administration of some of the thiazides results in some degree of carbonic
anhy-drase inhibition. However, at usual
doses, only chloroth-iazide shows any appreciable carbonic anhydrase
in-hibitory activity.
Renal Response
When administered at maximal
doses, chlorothiazide markedly increases excretion of NA+ , K+ ,
Cl- , and HCO3- . Maximal diuresis may
approach values as high as 10% of the filtered load, although fractional NA+
ex-cretions of 5% are more common. At usual clinical doses, however, the
thiazide diuretics generally increase excretion of NA+ and Cl-
, with an accompanying loss of K+ . Thus, unlike that of the
carbonic anhydrase in-hibitors, the diuresis produced by thiazide and
thiazide-like diuretics is of NaCl and not NaHCO3-. The
urinary K+ wasting induced by the thiazides is primarily a
con-sequence of the increased NA+ delivered to the distal tubule as
discussed earlier.
Two renal responses are
unique to the thiazide and thiazidelike diuretics. With these compounds, NA+
excre-tion is increased, while Ca++ excretion is decreased,
pri-marily and directly because of increased distal Ca++ re-absorption,
secondarily and indirectly because of a compensatory elevation of proximal
solute absorption, making this class of diuretics useful in treating
hypercal-ciuria. This effect, which may not be evident upon initial
administration of the drug, is particularly beneficial in individuals who are
prone to calcium stone formation.
A second unusual action of
this class of diuretics is their utility in treating nephrogenic diabetes
insipidus. Patients who have an adequate supply of ADH but whose kidneys fail
to respond to ADH excrete large volumes of very dilute urine, not unlike those
who have an ADH deficiency. The thiazides reduce glomerular fil-tration
modestly and decrease positive free water for-mation (CH2O), that is, production of
dilute urine. These actions combine to cause patients with nephrogenic di-abetes
insipidus to excrete a somewhat reduced urine volume with increased osmolality.
Absorption and Elimination
Orally administered thiazides
are rapidly absorbed from the gastrointestinal tract and begin to produce
diuresis in about 1 hour. Approximately 50% of an oral dose is excreted in the
urine within 6 hours. These compounds are organic acids and are actively
secreted into the prox-imal tubular fluid by the organic acid secretory
mecha-nism.There also appears to be an extrarenal pathway for their elimination
involving the hepatic–biliary acid se-cretory system that is particularly
important for thiazide elimination when renal function is impaired.
The thiazides have a variable
effect on elimination of uric acid, which also is secreted by the renal acid
se-cretory mechanism. Administration of thiazide diuret-ics, especially at low
doses, may elevate serum uric acid levels and cause goutlike symptoms.
Following large doses, thiazides may compete with uric acid for active
reabsorption and thereby may promote uric acid elimi-nation rather than impair
it .
Clinical Uses
Thiazides, especially
hydrochlorothiazide (Dyazide, Esidrix, HydroDIURIL, Oretic), are
useful adjunctive therapy in controlling the edema associated with con-gestive
heart failure, cirrhosis, premenstrual tension, and hormone therapy. They are
widely used in the treat-ment of hypertension whether or not it is accompanied
by edema .They can be used in patients with renal disease; however, their
diuretic activity is proportional to the residual tubular functional capacity
of the kidney. The thiazides do not prevent toxemia in pregnancy, nor are they
useful in the treatment of it.
Adverse Effects
Thiazides should be used
cautiously in the presence of severe renal and hepatic disease, since azotemia
and coma may result. The most important
toxic effect associ-ated with this class of diuretics is hypokalemia, which may result in muscular and central
nervous system symptoms, as well as cardiac sensitization (see Hypokalemia).
Periodic examination of serum elec-trolytes for possible imbalances is strongly
recom-mended. Appropriate dietary and therapeutic measures for controlling
hypokalemia are described later. The thiazides also possess some diabetogenic
potential, and although pancreatitis during thiazide therapy has been reported
in a few cases, the major mechanism contributing to the potential for glucose
in-tolerance is not known.
Related Topics