Chapter: Human Nervous System and Sensory Organs : Autonomic Nervous System
Sympathetic Trunk
Sympathetic Trunk
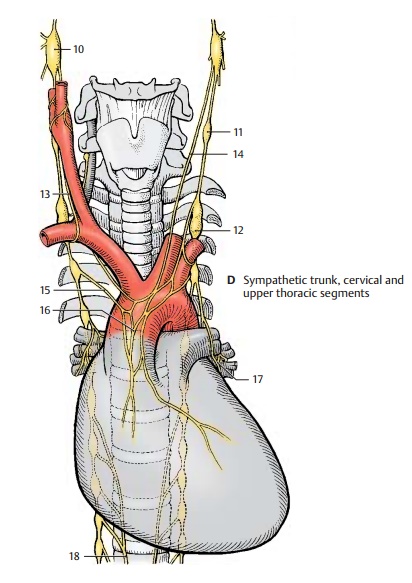
Cervical and Upper Thoracic Segments (D)
The cervical ganglia are reduced to three; the uppermost, the superior cervical ganglion (D10), lies below the base of the skull near the nodose ganglion (inferior ganglion of the vagus nerve). It receives fibers from the upper thoracic segment via the intergan-glionic branches. Its postganglionic fibers form plexuses around the internal carotid artery and external carotid artery. Branches extend from the internal carotid plexus to the meninges, to the eyes, and to the glands of the head region. The superior tarsal muscle of the upper eyelid and the ophthal-mic muscles at the posterior wall of the orbit are innervated by sympathetic fibers. Injury to the superior cervical ganglion therefore leads to drooping of the upper eyelid (ptosis) and to a backward displace-ment of the eyeball (enophthalmos).
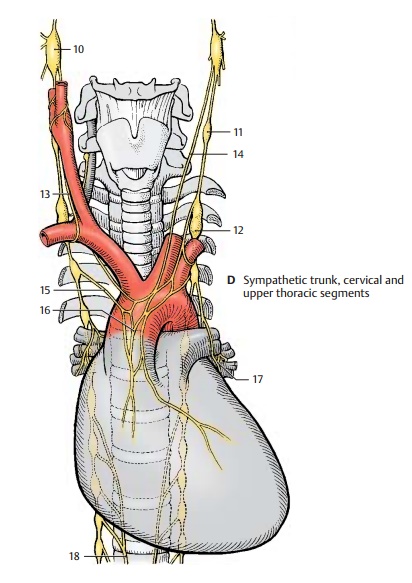
The middle cervical ganglion (D11) may be absent, and the inferior cervical ganglion has in most cases fused with the first thoracic ganglion to form the stellate ganglion (D12). Its postganglionic fibers form plexuses around the subclavian artery and around the vertebral artery. Fiber bundles connect-ing the stellate ganglion with the middle cervical ganglion extend across the sub-clavian artery and form the subclavian ansa (D13). Nerves from the cervical ganglia (D14) and nerves from the upper thoracic ganglia (D15) extend to the heart and to the hila of the lungs, where they participate to-gether with the parasympathetic fibers of the vagus nerve in the formation of the car-diac plexus (D16) and the pulmonary plexus(D17). The branches of the fifth to ninth sympathetic trunk ganglia join to form the greater splanchnic nerve (D18) which ex-tends to the celiac ganglia.
Lower Thoracic and Abdominal Segments (A)
Branches originating from the thoracic and upper lumbar sympathetic trunk ganglia extend to the prevertebral ganglia of the abdominal aortic plexus. There are severalgroups of ganglia. At the exit of the celiac trunk lie the celiac ganglia (A1) where the greater splanchnic nerve (A2) (T5 – T9) andthe lesser splanchnic nerve (A3) (T9 – T11) terminate. Their postganglionic fibers ex-tend with the branches of the aorta to stom-ach, duodenum, liver, pancreas, spleen, and adrenal gland (gastric plexuses, hepatic plexus, splenic plexus, pancreatic plexus, suprarenal plexus). Preganglionic fibers run to the adrenal medulla .
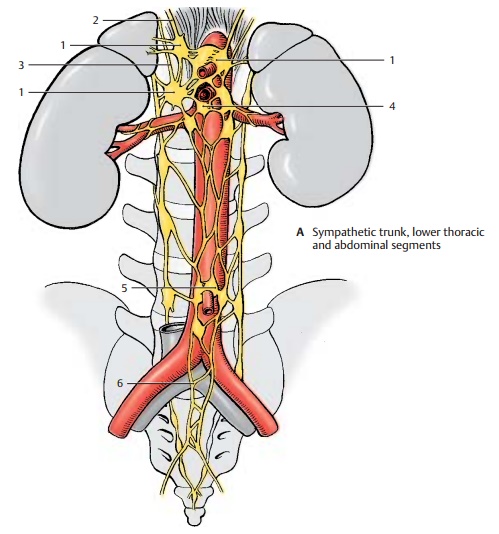
The postganglionic fibers from the superiormesenteric ganglion (A4), together with thebranches of the celiac ganglion, supply the small intestine, the ascending colon, and the transverse colon. The fibers from the inferiormesenteric ganglion (A5) supply the de-scending colon, the sigmoid colon, and the rectum. The preganglionic fibers (lumbar splanchnic nerves) of both ganglia originate from levels T11 – L2. Some branches extend to the renal plexus, which also contains fibers from the celiac ganglia and the supe-rior hypogastric plexus.
Parasympathetic fibers also participate in the formation of the visceral plexuses. Stimulation of parasympathetic fibers in the digestive tract leads to increased peristalsis and secretion as well as relaxation of the sphincter muscles, while stimulation of sympathetic fibers causes reduced peristal-sic and secretion as well as contraction of the sphincter muscles.
The pelvic organs are supplied by the supe-rior hypogastric plexus (A6) and the inferior hypogastric plexus. Both plexuses receivepreganglionic sympathetic fibers from the lower thoracic and upper lumbar spinal cord, and parasympathetic fibers from the sacral spinal cord.
The urinary bladder is predominantly inner-vated by the parasympathetic fibers of the visceral plexus that supply the muscles for bladder contraction (detrusor muscle). The sympathetic fibers terminate at the smooth muscles of the orifice of the urethra and both ureteral orifices. Regulation of bladder tone and urination takes place via spinal re-flexes which, in turn, are controlled by the hypothalamus and by cortical areas.
The genitals are supplied by the prostaticplexus in the male and by the uterovaginal plexus in the female. Stimulation of para-sympathetic fibers dilates the vessels of the cavernous bodies and thus triggers erection in the male (nervi erigentes). Stimulation of sympathetic fibers leads to vasoconstriction and to ejaculation. The uterine muscles are innervated by sympathetic and parasympa-thetic fibers. Their functional significance is not clear because even a denervated uterus is fully functional during pregnancy and parturition.
Innervation of the Skin (B)
The sympathetic fibers returning from the sympathetic trunk ganglia into the spinal nerves run in the peripheral nerves to the skin, where they innervate vessels, sweat glands, and erector pili muscles (vasomotor, sudomotor, pilomotor functions) in the corresponding derma-tomes. Segmental loss of these func-tions is of diagnostic significance in injuries to the spinal cord.
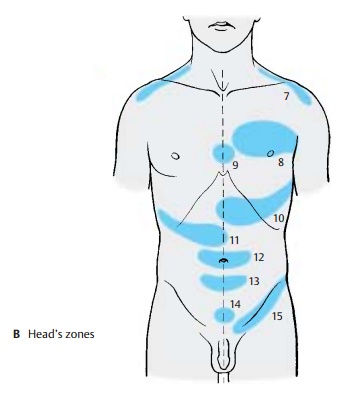
Clinical Note: In specific skin regions, Head’s zones (zones of hyperalgesia) (B), disease of anorgan may give rise to pain or hypersensitivity, with each organ being represented in a specific zone: diaphragm (B7) (C4), heart (B8) (T3/4), esophagus (B9) (T4/5), stomach (B10) (T8), liver and gallbladder (B11) (T8 – 11), small intestine (B12) (T10), large intestine (B13) (T11), urinary bladder (B14) (T11 – L1), kidneys and testes (B15) (T10 – L1). The Head’s zones are of practical im-portance in the diagnosis.
Related Topics