Chapter: Biology of Disease: Disorders of Acid Base Balance
Respiratory Acid Base Disorders
RESPIRATORY ACID–BASE DISORDERS
In respiratory acid–base disorders, the primary disturbance is caused by a change in the partial pressure of arterial CO2. Respiratory disorders are related to a defect in the rate of ventilation of lungs or the exchange of gases across the alveolar membrane. The changes in PCO2 alter the concentrations of carbonic acid in the blood, which, in turn, dissociates to HCO3– and H+.
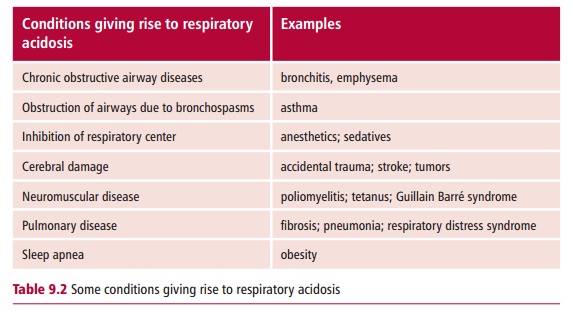
Some causes of respiratory acidosis are shown in Table 9.2. In general, obstruction of the airways by disease, or inhibition of the respiratory center in the brain by disease, trauma or drugs can cause respiratory acidosis.
Respiratory acidosis may be acute or chronic. Acute conditions occur within minutes or hours. It is usually the low PO2 (hypoxemia) that is more dangerous than the high PCO2 (hypercapnia). Further, renal compensation is slow, taking two or three days to become effective, so respiratory acidosis is usually uncompensated. Alveolar hypoventilation is usually the most common reason for acute respiratory acidosis. Hypoventilation increases the arterial PCO2and so the concentration of H+also rises quickly. The high PCO2andassociated low PO2 can cause coma and eventually death if untreated. Causes of acute respiratory acidosis include choking, bronchopneumonia and acute exacerbation of asthma.
Chronic respiratory acidosis is, again, usually due to a decline in alveolar ventilation. However, this is normally a well established condition and subject to maximum renal compensation. Long-standing conditions responsible for chronic respiratory disorders include chronic bronchitis and emphysema.
The high PCO2 is believed to be responsible for the clinical features of respiratory acidosis, such as peripheral vasodilatation and headaches. The acidosis can cause central nervous system depression leading to a coma. The treatment of respiratory acidosis is to improve alveolar ventilation, lowering the PCO2 and increasing the PO2. In chronic respiratory acidosis, it is usually not possible to treat the underlying cause and treatment is aimed at maximizing alveolar ventilation by using physiotherapy or bronchodilators.
Respiratory alkalosis is less common than respiratory acidosis. However, it is often an acute condition due to hyperventilation. Often renal compensation does not occur.
The clinical effects of respiratory alkalosis include confusion, headaches, dizziness and coma. Respiratory alkalosis may be caused by hypoxia, increased respiration or pulmonary disease. Hypoxia is associated with high altitudes, severe anemia and pulmonary disease. Increased respiration may result from the use of respiratory stimulants, such as salicylates, from primary hyperventilation syndrome, artificial hyperventilation, and pulmonary diseases, such as pulmonary edema and embolisms. The treatment of respiratory alkalosis is aimed at removing its underlying cause as this usually resolves the acid–base disturbance.
Related Topics