Chapter: Essentials of Anatomy and Physiology: Urinary System and Fluid Balance
Regulation of Urine Concentration and Volume
REGULATION OF URINE CONCENTRATION AND VOLUME
Given a solution in a container, such as a pan on a stove, it is pos-sible to change its concentration by adding water to it or by boiling it, thereby removing water. Similarly, the kidneys maintain the concentration of the body fluids by increasing water reabsorption from the filtrate when the body fluid concentration increases and by reducing water reabsorption from the filtrate when the body fluid concentration decreases. The volume and composition of urine therefore change, depending on conditions in the body. If body fluid concentration increases above normal levels, the kidneys produce a small volume of concentrated urine. This eliminates solutes and conserves water, both of which help lower the body fluid concentra-tion back to normal. On the other hand, if the body fluid concentra-tion decreases, the kidneys produce a large volume of dilute urine. As a result, water is lost, solutes are conserved, and the body fluid concentration increases.
Urine production also maintains blood volume and therefore blood pressure. An increase in blood volume can increase blood pressure, and a decrease in blood volume can decrease blood pres-sure. When blood volume increases above normal, the kidneys produce a large volume of urine. The loss of water in the urine lowers blood volume. Conversely, if blood volume decreases below normal, the kidneys produce a small volume of urine to conserve water and maintain blood volume.
Hormonal Mechanisms
Three major hormonal mechanisms are involved in regulating urine concentration and volume: the renin-angiotensin-aldosterone mech-anism, the antidiuretic hormone (ADH) mechanism, and the atrial natriuretic hormone (ANH) mechanism. Each mechanism is activated by different stimuli, but they work together to achieve homeostasis. Both the renin-angiotensin-aldosterone mechanism and the ANH mechanism are more sensitive to changes in blood pressure, whereas the ADH mechanism is more sensitive to chang- es in blood concentration.
Renin-Angiotensin-Aldosterone Mechanism
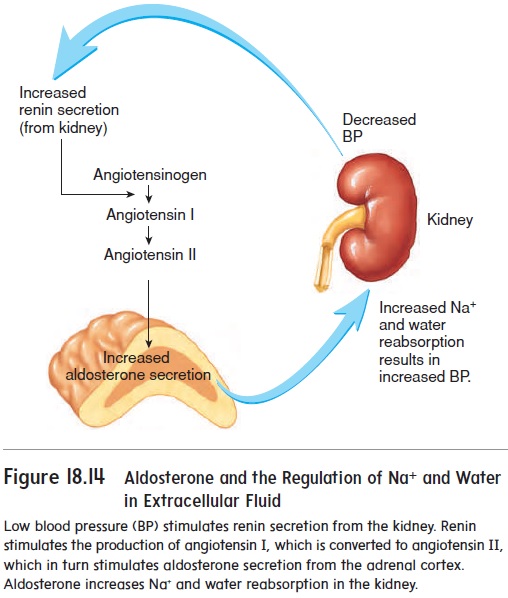
Renin (rē′nin, ren′in) and angiotensin (an′jē-ō-ten′sin) help regu- late aldosterone (al-dos′ ter-ōn) secretion. Renin, an enzyme, is secreted by cells of the juxtaglomerular apparatuses in the kidneys (see figure 18.5b). Renin acts on angiotensinogen (an′ jē-ō-ten-sin ō-jen), a plasma protein produced by the liver, and converts it to angiotensin I. Angiotensin I is rapidly converted to a smaller peptide called angiotensin II by angiotensin-converting enzyme(ACE). Angiotensin II acts on the adrenal cortex, causing it tosecrete aldosterone .
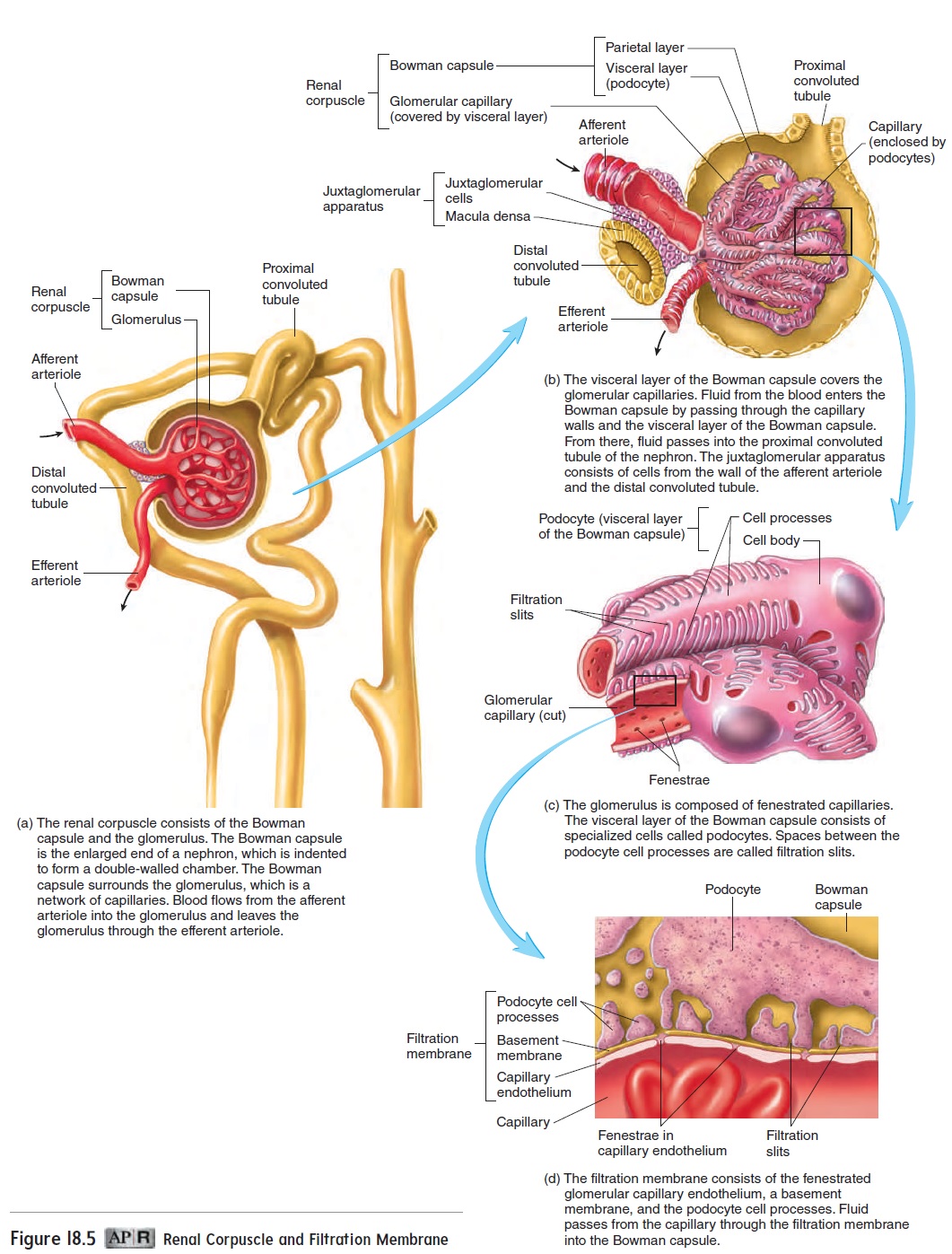
Aldosterone increases the rate of active transport of Na+ in the distal convoluted tubules and collecting ducts. In the absence of aldosterone, large amounts of Na+ remain in the nephron and become part of the urine. A high Na+ concentration in the filtrate causes water to remain in the nephrons and increases urine volume. Therefore, when the rate of active transport of Na+ is slow, urine volume increases, and the urine contains a high concentration of Na+. Because Cl− is attracted by the positive charge on Na+, Cl− is cotransported with Na+.
When blood pressure suddenly decreases (figure 18.14; see fig-ure 18.17) or when the concentration of Na+ in the filtrate becomes too low, the kidney releases renin. The resultant increase in aldo-sterone causes an increase in Na+ and Cl− reabsorption from the nephrons. Water follows the Na+ and Cl−. Thus, the volume of water lost in the form of urine declines. This method of conserving water helps prevent a further decline in blood pressure (figure 18.14; see figure 18.17).
Antidiuretic Hormone Mechanism
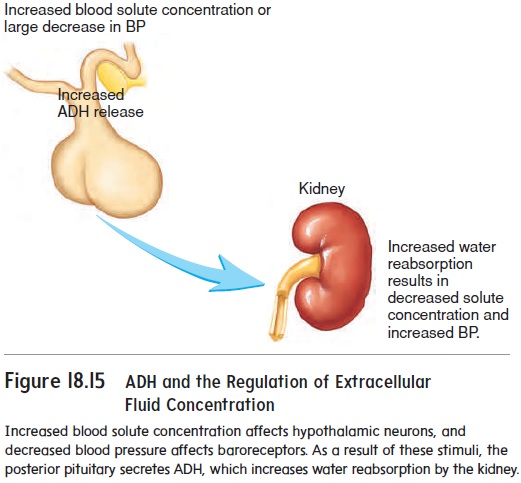
Antidiuretic (an′tē-d̄ı-̄u-ret′ik) hormone (ADH), secreted by theposterior pituitary gland, passes through the circulatory system to the kidneys. ADH regulates the amount of water reabsorbed by the distal convoluted tubules and collecting ducts. When ADH levels increase, the permeability of the distal convoluted tubules and collecting ducts to water increases, and more water is reabsorbed from the filtrate. Consequently, an increase in ADH results in the production of a small volume of concentrated urine. On the other hand, when ADH levels decrease, the distal convoluted tubules and collecting ducts become less permeable to water. As a result, less water is reabsorbed, and a large volume of dilute urine is pro-duced (figure 18.15; see figure 18.17).
The release of ADH from the posterior pituitary is regulated by the hypothalamus. Certain cells of the hypothalamus are sensi-tive to changes in solute concentration. When the solute concen-tration in the blood increases, action potentials are sent along the axons of the ADH-secreting neurons of the hypothalamus to the posterior pituitary, and ADH is released from the ends of the axons (figure 18.15;). A reduced solute concentration in the blood causes inhibition of ADH release.
Baroreceptors that monitor blood pressure also influence ADH secretion. A large decrease in blood pressure causes an increase in ADH secretion (figure 18.15; see figure 18.17), and a large increase in blood pressure decreases ADH secretion.
Atrial Natriuretic Hormone
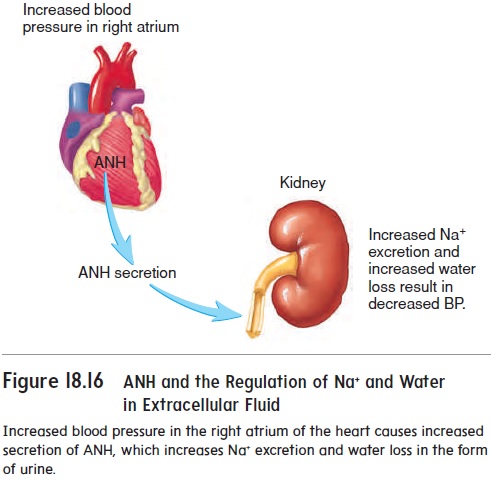
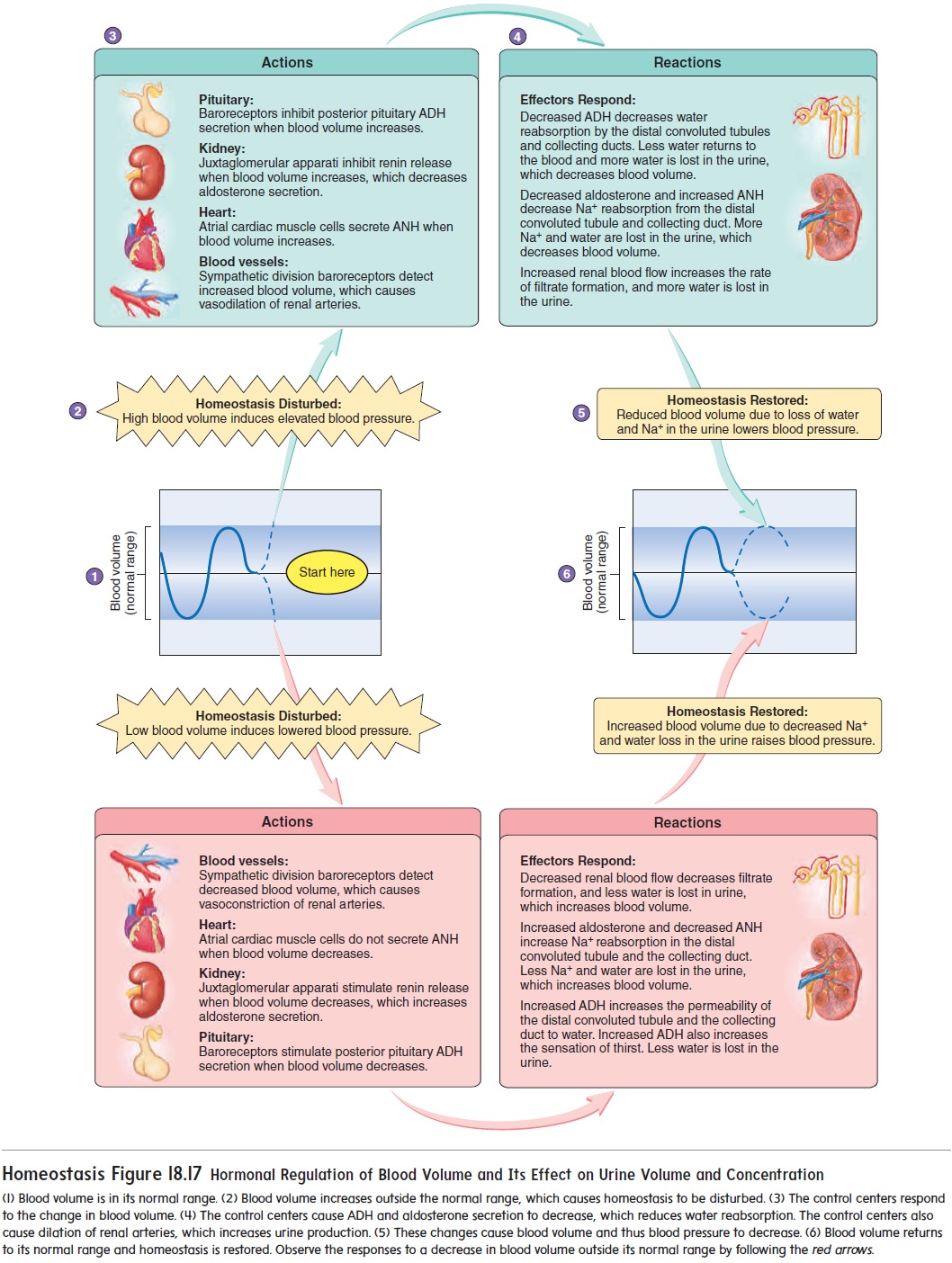
Atrial natriuretic (n̄a′trē-̄u-ret′ik) hormone (ANH) is secreted from cardiac muscle cells in the right atrium of the heart when blood pressure in the right atrium increases above normal (fig-ures 18.16 and 18.17). ANH acts on the kidney to decrease Na+ reabsorption. Therefore, Na+ and water remain in the nephron to become urine. The increased loss of Na+ and water as urine reduces the blood volume and the blood pressure.
Related Topics