Chapter: Clinical Dermatology: Psoriasis
Psoriasis: Treatment
Treatment
The
need for this depends both on the patient’s own perception of his or her
disability, and on the doctor’s objective assessment of how severe the skin
disease is. The two do not always tally.
General measures
Explanations
and reassurances must be geared to the patient’s or the parent’s intelligence.
Information leaflets help to reinforce verbal advice. The doctor as well as the
patient should keep the disease in per-spective, and treatment must never be
allowed to be more troublesome than the disease itself. The dis-ease is not
contagious. At present there is no cure for psoriasis; all treatments are
suppressive and aimed at either inducing a remission or making the condition
more tolerable. However, spontaneous remissions will occur in 50% of patients.
Treatment for patients with chronic stable plaque psoriasis is relatively
simple and may be safely administered by the family practitioner. However,
systemic treatment for severe psoriasis should be monitored by a dermatologist.
No treatment, at present, alters the overall course of the disease.
Physical
and mental rest help to back up the specific management of acute episodes.
Concomitant anxiety and depression should be treated on their own merits (see
Table 5.1 for appropriate treatments).
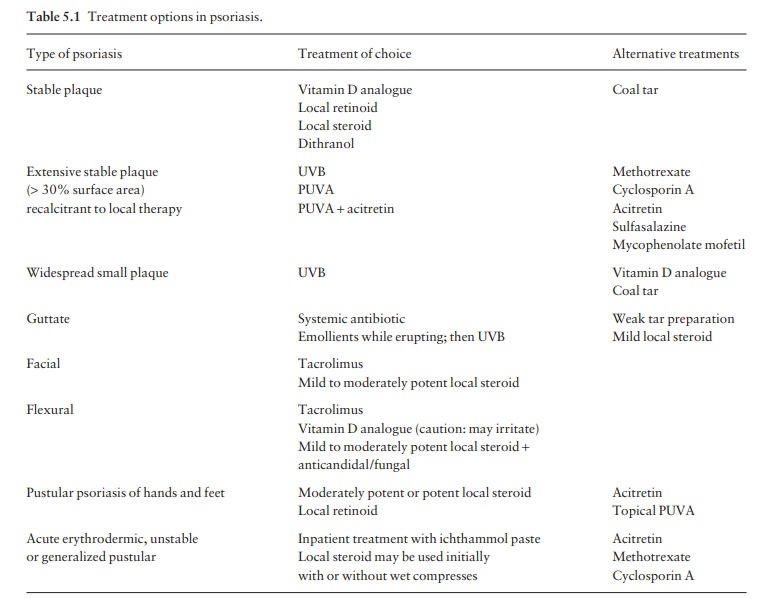
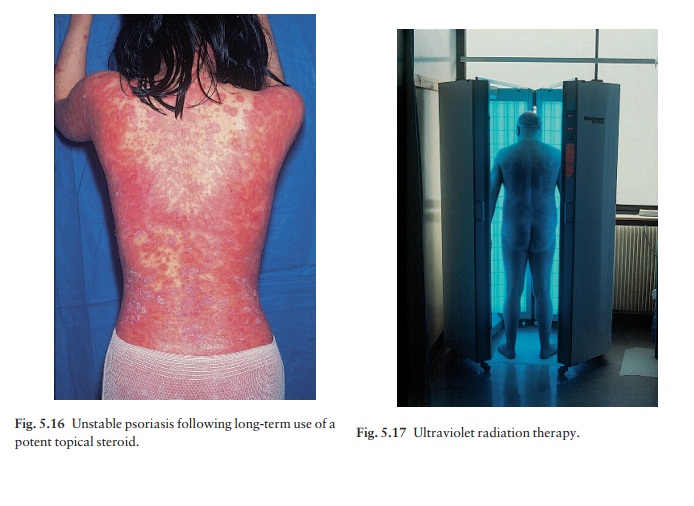
Main types of treatment
These
can be divided into four main categories: local, ultraviolet radiation,
systemic and combined. Broad recommendations are listed in Table 5.1, but most
physicians will have their own favourites. In many ways it is better to become
familiar with a few remedies than dabble with many. The management of patients
with psoriasis is an art as well as a science and few other skin conditions
benefit so much from patience and experienceaof both patients and doctors.
Related Topics