Chapter: Essentials of Anatomy and Physiology: Human Development and Genetics
Placenta and Umbilical Cord
PLACENTA AND UMBILICAL CORD
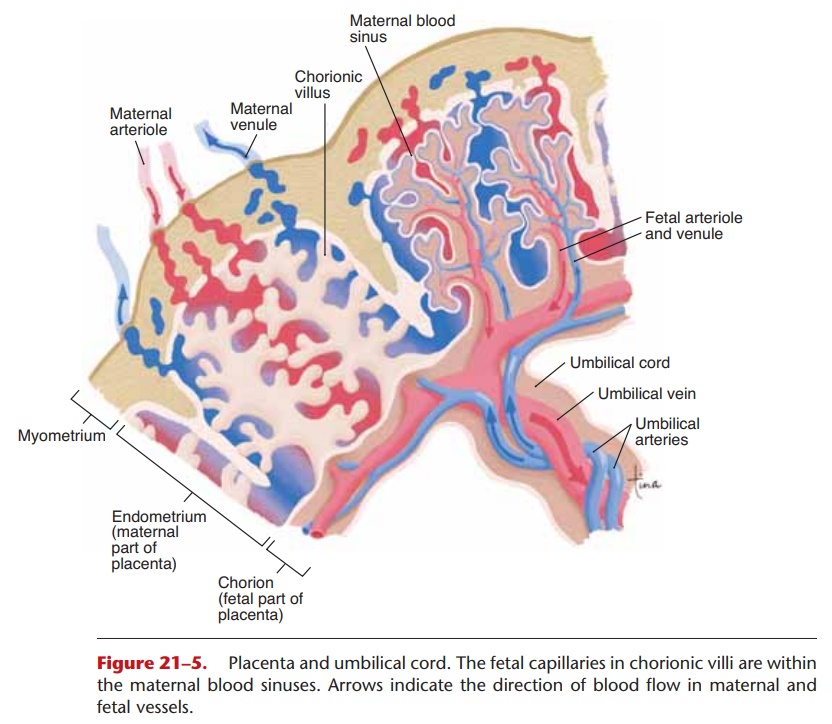
The placenta is made of both fetal and maternal tissue. The chorion of the embryo and the endometrium of the uterus contribute, and the placenta is formed by the third month of gestation (12 weeks). The mature placenta is a flat disc about 7 inches (17 cm) in diameter.
The structure of a small portion of the placenta is shown in Fig. 21–5. Notice that the fetal blood vessels are within maternal blood sinuses, but there is no direct connection between fetal and maternal vessels. Normally, the blood of the fetus does not mix with that of the mother. The placenta has two functions: to be the site of exchanges between maternal and fetal blood and to produce hormones to maintain preg-nancy. We will consider the exchanges first.
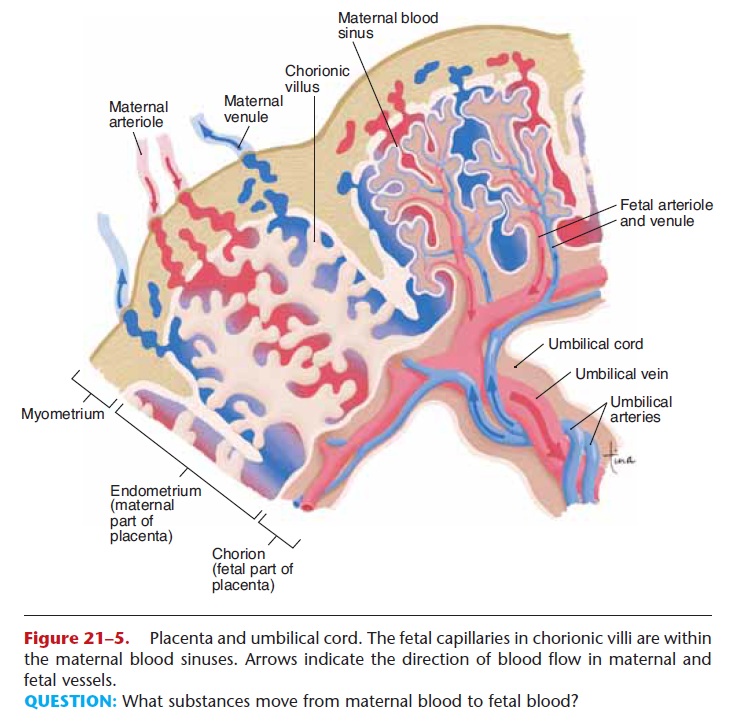
The fetus is dependent upon the mother for oxygen and nutrients and for the removal of waste products. The umbilical cord connects the fetus to the pla-centa. Within the cord are two umbilical arteries that carry blood from the fetus to the placenta and one umbilical vein that returns blood from the placenta to the fetus.
When blood in the umbilical arteries enters the placenta, CO2 and waste products in the fetal capillar-ies diffuse into the maternal blood sinuses. Oxygen diffuses from the maternal blood sinuses into the fetal capillaries; nutrients enter the fetal blood by diffusion and active transport mechanisms. This oxygen- and nutrient-rich blood then flows through the umbilical vein back to the fetus.
When the baby is delivered at the end of gestation, the umbilical cord is cut. The placenta then detaches from the uterine wall and is delivered, with the rest of the umbilical cord, as the afterbirth.
The blood in the remnant of the umbilical cord contains abundant stem cells, and their potential to become different kinds of cells is between that of embryonic stem cells (which may become any human cell) and adult stem cells (which are more limited). Umbilical cord stem cells have already been used to treat newborns with infantile Krabbe’s disease, a neu-rological disorder that is fatal by the age of 2 years. Such treatment depends on genetic testing and having suitable donated cord stem cells available at birth. Banks of cord blood are being established by some medical centers (because such donated blood can be frozen and stored), and the use of cord stem cells may someday decrease the need for bone marrow trans-plants.
Placental Hormones
The first hormone secreted by the placenta is human chorionic gonadotropin (hCG), which is produced by the chorion of the early embryo. The function of hCG is to stimulate the corpus luteum in the maternal ovary so that it will continue to secrete estrogen and progesterone.
The secretion of progesterone is partic-ularly important to prevent contractions of the myometrium, which would otherwise result in miscar-riage of the embryo. Once hCG enters maternal cir-culation, it is excreted in urine, which is the basis for many pregnancy tests. Tests for hCG in maternal blood are even more precise and can determine whether a pregnancy has occurred even before a men-strual period is missed.
The corpus luteum is a small structure, however, and cannot secrete sufficient amounts of estrogen and progesterone to maintain a full-term pregnancy. The placenta itself begins to secrete estrogen and proges-terone within a few weeks, and the levels of these hor-mones increase until birth. As the placenta takes over, the secretion of hCG decreases, and the corpus luteum becomes non-functional. During pregnancy, estrogen and progesterone inhibit the anterior pitu-itary secretion of FSH and LH, so no other ovarian follicles develop. These placental hormones also pre-pare the mammary glands for lactation.
The placenta also secretes relaxin, which helps inhibit contractions of the myometrium. Relaxin also permits stretching of the ligaments of the pubic sym-physis so that this joint will give a little, if necessary, during birth.
Related Topics