Chapter: Clinical Dermatology: Skin reactions to light
Photoallergy
Photoallergy
Drugs,
topical or systemic, and chemicals on the skin, can interact with UVR and cause
immunological reactions.
Cause
UVR
converts an immunologically inactive form of a drug into an antigenic molecule.
An immunological reaction, analogous to allergic contact dermatitis, is induced
if the antigen remains in the skin or is formed there on subsequent exposure to
the drug and UVR. Many of the same drugs that cause photo-toxic reactions can
also cause photoallergic ones.
Presentation
Photoallergy
is often similar to phototoxicity. The areas exposed to UVR become inflamed,
but the reaction is more likely to be eczematous. The eruption will be on
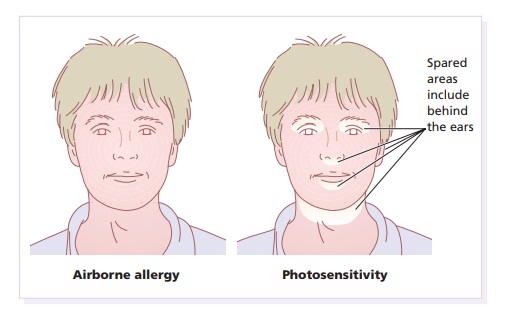
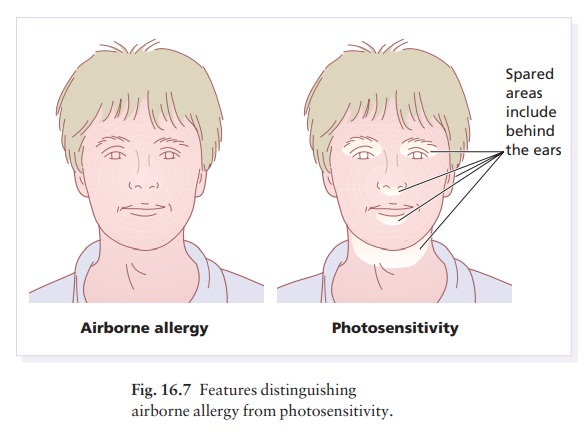
exposed areas such as the hands, the V of the neck, the nose, the chin and the
forehead. There is also a tendency to spare the upper lip under the nose, the
eyelids and the submental region (Fig. 16.7). Often the eruption does not occur
on the first expos-ure to ultraviolet, but only after a second or further
exposures. A lag phase of one or more weeks is needed to induce an immune
response.
Course
The original lesions are red patches, plaques, vesicles or bullae, which usually become eczematous. They tend to resolve when either the drug or the exposure to UVR is stopped, but this may take several weeks.
Complications
Some
drugs, such as the sulphonamides, can cause a persistent light reaction .
Investigations
Photopatch
testing by an expert can confirm the diagnosis. The chemical is applied for 24
h and the skin is then irradiated with UVA. An acute photo-allergic contact
dermatitis is then elicited. A control patch, not irradiated, rules out
ordinary allergic con-tact dermatitis.
Treatment
The
drug should be stopped and the patient pro-tected from further ultraviolet
exposure (avoidance,clothing and sunscreens). Potent topical corticos-teroids
or a short course of a systemic corticoster-oid will hasten resolution and
provide symptomatic relief.
Related Topics