Chapter: Human Neuroanatomy(Fundamental and Clinical): Tracts of Spinal Cord and Brainstem
Pathways connecting the spinal cord to the cerebral cortex
PATHWAYS CONNECTING THE SPINAL CORD TO THE CEREBRAL CORTEX
The Posterior Column − Medial Lemniscus Pathway
Fasciculus gracilis and fasciculus cuneatus:
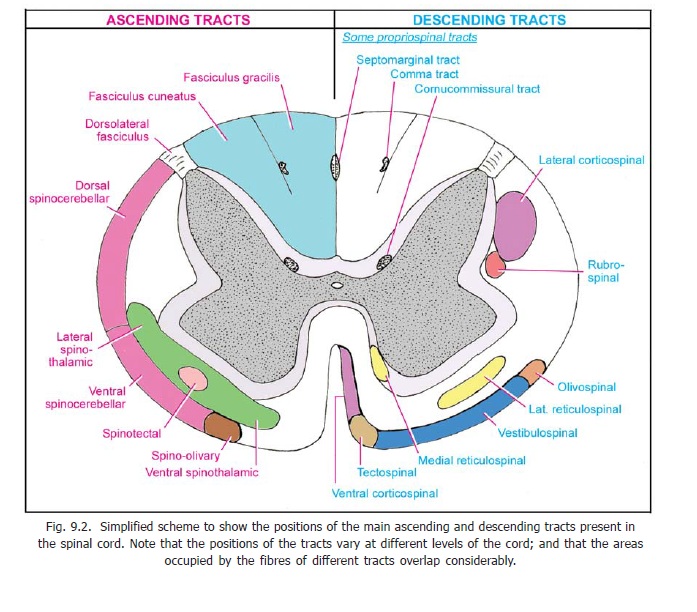
These tracts occupy the posterior funiculus of the spinal cord and are, therefore, often referred to as the posterior column tracts(Fig. 9.2). They are unique in that they are formed predominantly by central processes of neurons located in dorsal nerve root ganglia i.e., by first order sensory neurons (Fig. 9.6). The fibres derived from the lowest ganglia are situated most medially; while those from the highest ganglia are most lateral. The fasciculus gracilis, which lies medially is, therefore, composed of fibres from the coccygeal, sacral, lumbar and lower thoracic ganglia; while the fasciculus cuneatus which lies laterally consists of fibres from upper thoracic and cervical ganglia. The fibres of these fasciculi extend upwards as far as the lower part of the medulla. Here the fibres of the gracile and cuneate fasciculi terminate by synapsing with neurons in the nucleus gracilis and nucleus cuneatus respectively.
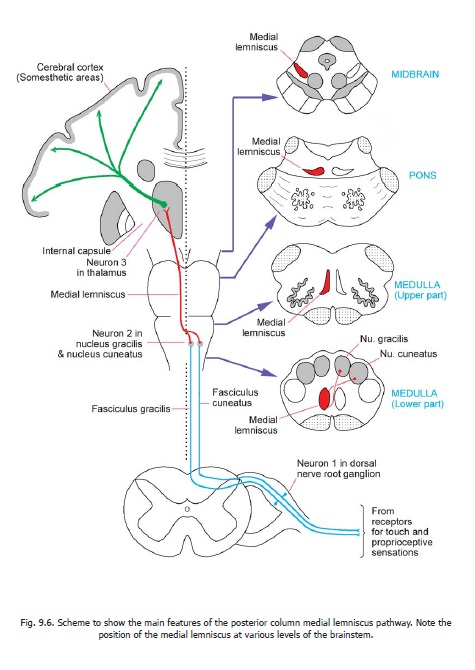
Medial Lemniscus
The neurons of the gracile and cuneate nuclei are second order sensory neurons. Their axons run forwards and medially (asinternal arcuate fibres) to cross the middle line. The crossing fibres of the two sides constitute the sensory decussation (or lemniscal decussation). Having crossed the middle line, the fibres turn upwards to form a prominent bundle called the medial lemniscus (Fig. 9.6). The medial lemniscus runs upwards through the medulla, pons and midbrain to end in the thalamus (ventral posterolateral nucleus).
Third order sensory neurons located in the thalamus give off axons that pass through the internal capsule and the corona radiata to reach the somatosensory areas of the cerebral cortex.
The pathway described above carries:
(a) Some components of the sense of touch. These include deep touch and pressure, the ability to localise exactly the part touched (tactile localisation), the ability to recognise as separate two points on the skin that are touched simultaneously (tactile discrimination), and the ability to recognise the shape of an object held in the hand (stereognosis).
(b) Proprioceptive impulses that convey the sense of position and of movement of different parts of the body.
(c) The sense of vibration.
Some further facts of interest about the fasciculus gracilus and fasciculus cuneatus are as follows.
1. Nerve fibres carrying proprioceptive impulses through the fasciculus gracilis predominantly end inthe dorsal nuclei (in the posterior grey column of thoracic segments of the spinal cord) and, therefore, do not reach cervical levels. Hence, most of the fibres passing through the fasciculus in upper cervical segments are from cutaneous receptors.
2. In contrast to the fasciculus gracilis, the fasciculus cuneatus carries numerous proprioceptivefibres (as well as those for cutaneous sensations) throughout its extent.
3. Both the fasciculi are made up predominantly of myelinated fibres.
4. In experimental animals it has been shown that the fibres of these fasciculi are grouped in termsof the dermatomes they carry impulses from. At higher levels the fibres change position and come to be arranged somatotropically (i.e., in accordance with parts of the body). This somatotropic organisation is maintained in the gracile and cuneate nuclei. The fibres from the lower limb are most medial (in nucleus gracilis) followed by those from the trunk and upper limbs (in nucleus cuneatus).
5. The nucleus gracilis and cuneatus receive descending fibres from the cerebral cortex, the cerebellum,and from the reticular formation. These afferents may facilitate or inhibit transmission through these nuclei.
Spinothalamic Pathways
Anterior and Lateral spinothalamic tracts
a. The first order neurons of this pathway are located in spinal ganglia. The central processes of these neurons enter the spinal cord and terminate in relation to spinal grey matter. They may ascend in the dorsolateral tract (situated near the tip of the dorsal grey column, Fig. 9.2) for one or more segments before ending in grey matter.
b. The second order neurons of this pathway, are located mainly in laminae IV, V, VI and VII. The axons of these neurons constitute the anterior and lateral spinothalamic tracts. They cross to the opposite side of the spinal cord in the white commissure (but some fibres may remain on the same side). The crossing of the fibres is oblique. The fibres for the lateral spinothalamic tract cross within the same segment of the cord, while those of the anterior spinothalamic tract may ascend for one or more segments before they cross to the opposite side. The tracts also carry some uncrossed fibres (about 10 per cent).
The fibres for the anterior spinothalamic tract enter the anterior funiculus (Figs. 9.2, 9.7) where they lie medial to emerging fibres of ventral nerve roots. The fibres for the lateral spinothalamic tract enter the lateral funiculus. The two tracts form one continuous band that runs up the spinal cord. On reaching the medulla the two tracts separate. The anterior spinothalamic tract joins the medial lemniscus and travels through it to the thalamus. The lateral spinothalamic tract runs through the brainstem as a separate bundle called the spinal lemniscus which (like the anterior tract) ends in the thalamus. All spinothalamic fibres end in the ventral posterolateral nucleus.
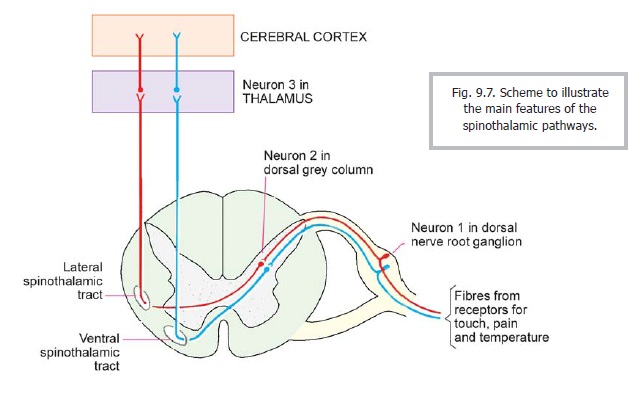
Traditionally it has been said that the anterior spinothalamic tract carries sensations of crude touch and pressure, while the lateral tract has been said to carry sensations of pain and temperature. It is now realised that although different fibres within the spinothalamic tracts carry different types of sensations, the anterior and lateral spinothalamic tracts constitute a single functional unit.
Advanced:
According to some authorities the anterior spinothalamic tract does not join the medial lemniscus, but travels along with the lateral spinothalamic tract in the spinal lemniscus.
Studies in experimental animals (monkeys) have brought out some interesting facts regarding the location of neurons giving rise to the spinothalamic tracts.
1. The neurons are not uniformly distributed through the length of the cord. As many as 30% of allneurons are present in the first three cervical segments; and another 20% in the lower cervical segments. Lumbar segments account for another 20%, the remaining 30% being from thoracic and sacrococcygeal segments.
2. About ten per cent of neurons are ipsilateral, and of these 50% are in the upper three cervicalsegments.
3. The neurons are widely distributed in spinal grey matter, but the laminae involved vary at differentlevels of the spinal cord. In the upper three cervical segments most neurons lie in laminae VI and VII. Some neurons lie in laminae I, IV, and V. Ipsilateral neurons lie mainly in lamina VIII.
In the lower cervical segments, and also in the lumbar region, the neurons lie in laminae 1, V, VII and VIII. In thoracic segments they are confined to laminae V and VII.
Dorsolateral spinothalamic tract
In addition to the anterior and lateral spinothalamic tracts a separate dorsolateral spinothalamic tract has been described. The fibres of this tract arise from neurons in lamina I, cross to the opposite side, and ascend in the dorsolateral fasciculus to reach the ventral posterolateral nucleus of the thalamus. The tract carries impulses arising in skin (mainly pain and temperature). Relief of pain observed after dorsolateral cordotomy may be a result of the cutting of these fibres.
Spino-cervico-thalamic pathway
This is yet another pathway through which cutaneous sensations (touch, pressure, pain and temperature) reach the thalamus. Axons arising from neurons located in laminae III to V of spinal grey matter collect to form a spinocervical tract that ascends through the dorsolateral fasciculus. They end in the lateral cervical nucleus (which is a small collection of neurons lying amongst the fibres of the lateral funiculus in spinal segments C1 and C2). New fibres arising here project to the ventral posterolateral nucleus of the thalamus.
Related Topics