Chapter: Paediatrics: Genetics
Paediatrics: Genetic disorders of growth
Genetic disorders of growth
Assessment of growth plays an
important role in deciding whether a child may have an underlying genetic
disorder. Measurements <0.4th centile or >99.6th centile nearly always
merit further assessment, unless there is a clear explanation. Measurements
between the 0.4th and 2nd centiles or 98th and 99.6th need to be interpreted in
context and may be clinically significant. If in doubt, discuss with a senior
colleague.
Intrauterine growth retardation (IUGR)
Silver–Russell syndrome
•
Incidence
is unclear (1/3000–100 000 births). Equal sex ratio.
•
710%
of children have maternal UPD7.
•
Genetically
heterogeneous condition characterized by intrauterine and postnatal growth
retardation with short stature and FTT. Typically, babies have
disproportionately large head (OFC usually 3rd–25th centile), triangular
facies, down-turned mouth, some asymmetry of limbs.
•
About
30–50% of cases will show hypomethylation of the paternal chromosome at the IC1
(imprinting centre) on 11p15.5.
Cornelia de Lange syndrome
•
Rare;
incidence 71/50,000 live births.
•
Intrauterine
and postnatal growth impairment, limb anomalies, microcephaly, hirsutism, and
distinctive facial features (neat arched eyebrows, short upturned nose, thin
lips with down-turned corners of the mouth).
•
Approximately
60% of affected children have mutations in the gene NIPBL on chromosome 5p13.
Short stature
Turner syndrome
•
Affects
71/2500 females.
•
Most
girls have a single X chromosome (45, X), usually due to non-disjunction.
•
As
well as short stature, the typical phenotype includes: broad neck; ptosis; wide
carrying angle at elbows (cubitas valgus); widely spaced hypoplastic nipples;
low posterior hairline, excessive pigmented naevi. Puffiness of the hands and
feet is a common neonatal finding.
•
Associated
abnormalities include: congenital heart disease (15–50%), especially
coarctation of the aorta and VSD; structural renal anomalies (730%), e.g.
horseshoe kidney or unilateral renal agenesis; hypoplastic ‘streak’ ovaries (p amenorrhoea and infertility).
•
The
phenotype can be very subtle and is easily missed, and so a chromosome analysis
is usually offered to all girls with unexplained short stature.
Tall stature
Marfan syndrome
Obesity
Bardet–Biedl syndrome (BBS)
•
Rare
condition; incidence in the UK population <1/100 000.
•
Genetically
heterogeneous with at least 8 genes identified to date. In the majority of
families inheritance is autosomal recessive.
•
Features include: pigmentary retinopathy; postaxial
polydactyly; obesity; cognitive
impairment; renal defects.
Prader–Willi syndrome (PWS)
•
Affects
71/10 000 individuals.
•
Caused
by disruption to the paternally derived imprinted domain on 15q11–13.
•
Babies
are floppy with feeding difficulties and may fail to thrive in infancy. There
is rapid weight gain between the ages of 1 and 6yrs.
•
Older
children have truncal obesity, mild/moderate learning difficulties, and short
stature. Typically children have an insatiable appetite with food-foraging and
other behavioural problems.
•
Diagnosis
is by molecular genetic analysis (SNRPN
methylation assay).
Overgrowth
Beckwith–Wiedemann syndrome
·Incidence 71/14,000.
•
Genetic
basis is complex; it is caused by disruption of the imprinted region on
chromosome 11p15.
•
Usually
presents in the perinatal period with macrosomia. Birth weight is usually
>97th centile and length is usually > +2SD. Polyhydramnios or preterm
delivery commonly occur.
•
There
may be associated congenital anomalies: exomphalos/umbilical hernia; dysmorphic
features (e.g. ear lobe creases, port wine stain, macroglossia (large tongue));
visceromegaly; hemihypertrophy.
•
Neonates
are at risk for severe hypoglycaemia and should be monitored closely.
•
Macrosomia
continues through early childhood and then becomes less dramatic with
increasing age.
•
Some
children with BWS are at increased risk for Wilms’ tumour.
•
In
750% diagnosis can be confirmed by molecular genetic testing. Uniparental
disomy 11p15 analysis requires blood testing of child and both parents.
Sotos syndrome
•
Incidence
71/15 000 children.
•
Due to
mutation or deletion in the NSD1 gene
on chromosome 5q35. Most are isolated de
novo mutations but familial cases do occur.
Characterized by prenatal overgrowth (birth weight 74200g in males; 74000g in females), which persists in childhood, especially through the pre-school years. Final adult height is often in the upper normal range. OFC is also increased and bone age is advanced. Affected children typi-cally have a tall skull with a prominent broad forehead and pointed chin. Developmental delay is almost always present, but varies from mild to severe. Some children have seizures.
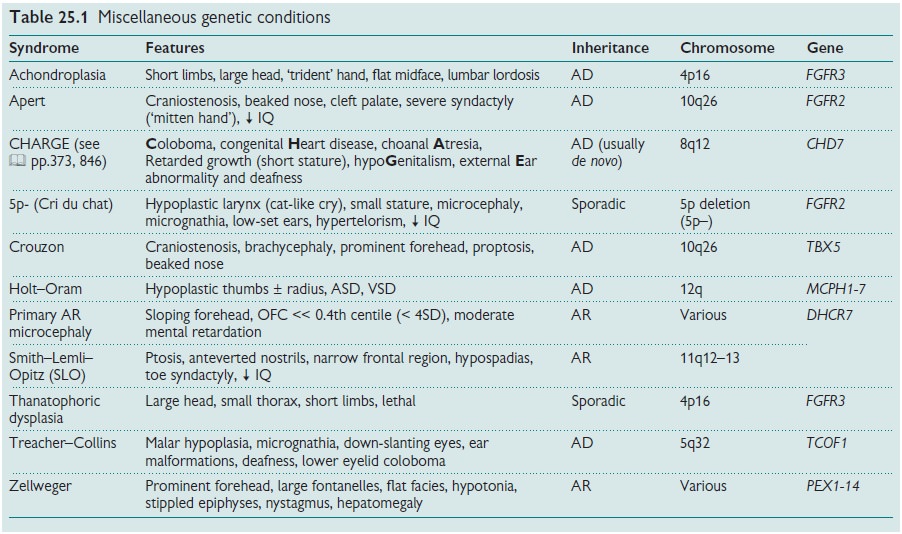
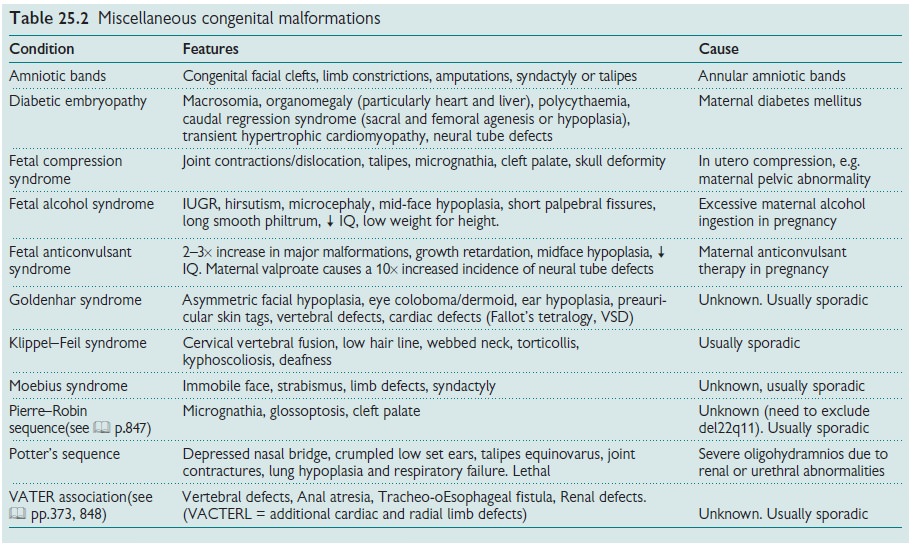
Related Topics