Chapter: Obstetrics and Gynecology: Isoimmunization
Isoimmunization: Assessment
ASSESSMENT
Although antibody titers reflect
the strength and the amount of the maternal antibody response, their utility in
pregnancy management is limited. Titers
provide no information aboutfetal status. In an initial sensitized
pregnancy, serial antibodytiter values can assist in determining when the
maternal anti-body response is strong enough to represent a risk of fetal
anemia. A critical titer is that
titer associated with a signif-icant risk for severe fetal hemolytic disease
and hydrops fetalis. In most centers, this is between 1:8 and 1:32. If the
initial antibody titer is 1:8 or less, the Rh D-negative patient can be
monitored with titer assessment every 4 weeks. In a first-sensitized pregnancy,
titers are generally performed every 4 weeks. With a history of an affected
fetus or infant, titers are not helpful in predicting fetal hemolytic disease
and further evaluation is warranted.
Evaluation for possible fetal
anemia is usually under-taken in the second trimester, although management may
be individualized depending on history and available exper-tise. Traditionally,
amniotic fluid assessment of the level of bilirubin has been used as a measure
of fetal status and an indirect means of estimating the potential for severe
fetal anemia. In the second half of a normal pregnancy, the level of bilirubin
in the amniotic fluid decreases progressively, whereas in an affected,
isoimmunized patient, the amount of bilirubin detected can deviate
significantly. The increase in the amniotic fluid bilirubin in affected pregnancies
is a result of fetal urinary excretion of the increased amount of circulating
bilirubin. Until recently, serial amnio-centeses were performed to determine
the level of biliru-bin in the amniotic fluid, which in turn reflected the
severity of fetal anemia.
The
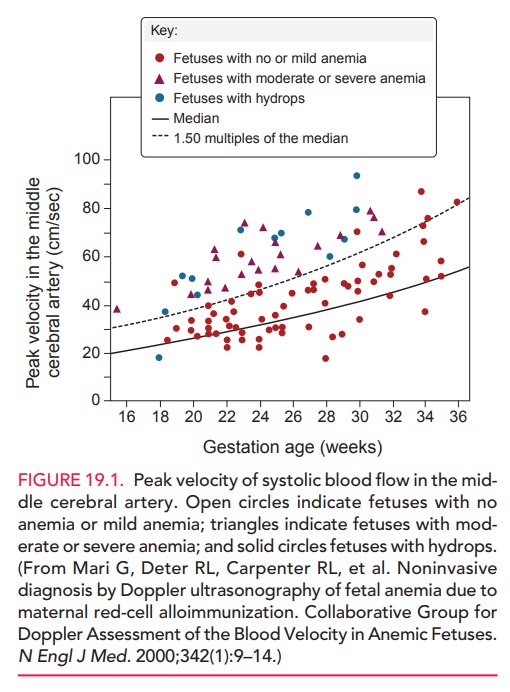
current trend in management is the measurement of peak velocity of middle cerebral artery (MCA) flow using Doppler ultrasound. The
velocity of flow through the MCA is related to the viscosity of the blood. In
the setting of fetal anemia, the blood is less viscous due to fewer cells and,
therefore, the velocity of flow increases. Gestational age-specific peak
velocity normal curves have been derived and correlated with the fetal
hematocrit. The degree of peak velocity elevation above the median for that
gestational age can be used to estimate the fetal hematocrit and thus the risk
of fetal anemia. Using the peak systolic velocity of the MCA, almost all
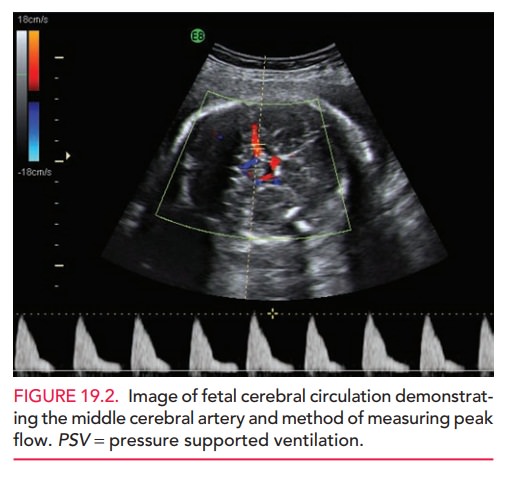
fetuses with moderate to severe anemia can be identified (Figs. 19.1 and 19.2).
Ultrasound
assessment of the fetus is also helpful in detecting severe signs of hemolysis
that have resulted in profound fetal anemia. Occasionally,
the first presenting signs of fetalhemolysis may be hydropic changes in the
fetus including subcutaneous edema, pericardial and/or pleural effusions, and
ascites. When these findings are identified and hydrops fetalis is diagnosed,
the fetal hematocrit is typically <15%.
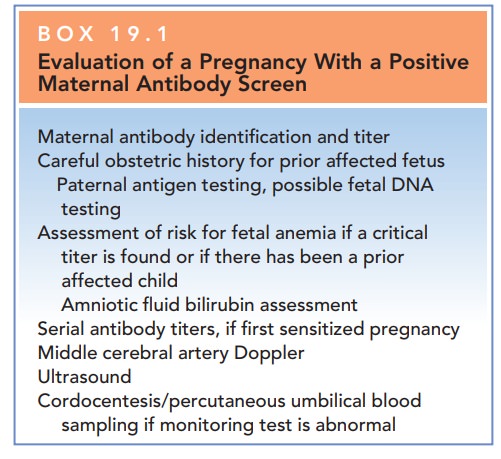
Regardless of the methods used to monitor pregnan-cies at risk for fetal anemia, all techniques are designed to determine the fetal hematocrit using indirect measures. If the monitoring test indicates a risk for fetal anemia, or if hydrops is diagnosed, cordocentesis or percutaneous umbilicalblood sampling (PUBS) is performed to directly measure thefetal hematocrit. Under ultrasound guidance, a needle isadvanced into the umbilical vein, a sample of fetal blood removed, and the hematocrit is measured. In general, the average fetal hematocrit is 36% to 44% and, with severe anemia, it is less than 30% (Box 19.1).
In addition to
proce-dures to monitor the fetus for anemia, general tests for fetal well-being
are indicated in all isoimmunized women with titers above the critical threshold,
because the ability of an affected fetus, even if only mildly anemic, to
withstand the stresses of pregnancy and labor may be compromised.
Related Topics