Chapter: Medical Surgical Nursing: Terrorism, Mass Casualty, and Disaster Nursing
Initiating the Emergency Operations Plan
INITIATING THE EMERGENCY OPERATIONS PLAN
Notification of a
disaster situation to a facility varies with each sit-uation. Generally, the
notification to the facility comes from out-side sources unless the initial
incident occurred at the facility. The disaster activation plan should clearly
state how the EOP is to be initiated. If communication is functioning, field
incident com-mand will give notice of the approximate number of arriving
pa-tients, although the number of self-referring patients will not be known.
Identifying Patients and Documenting Patient Information
Patient tracking is a
critical component of casualty management. Disaster tags, which are numbered
and include triage priority, name, address, age, location and description of
injuries, and treat-ments or medications given, are used to communicate patient
in-formation. The tag should be securely placed on the patient and remain with
the patient at all times. The tag number and the pa-tient’s name are recorded
in a disaster log. The log is used by the command center to track patients,
assign beds, and provide families with information.
Triage of Disaster Victims
Triage is the sorting of
casualties to determine priority of health care needs and the proper site for
treatment. In nondisaster situ-ations, health care workers assign a high
priority and allocate the most resources to those who are the most critically
ill. For exam-ple, a young man who has a chest injury and is in full cardiac
ar-rest would receive advanced cardiopulmonary resuscitation, including
medications, chest tubes, intravenous fluids, blood, possibly even emergency
surgery in an effort to restore life. In a disaster, however, when health care
providers are faced with a large number of casualties, the fundamental
principle guiding re-source allocation is to do the greatest good for the
greatest num-ber of people. Decisions are based on the likelihood of survival
and consumption of available resources. Therefore, this same pa-tient, and
others with conditions associated with a high mortality rate, would be assigned
a low triage priority in a disaster situation, even if the person is conscious.
Although this may sound uncaring, from an ethical standpoint the expenditure of
limited resources on individuals with a low chance of survival, and denial of
those resources to others with serious but treatable conditions, cannot be
justified.
The triage officer
rapidly assesses those injured at the disaster scene. Victims are immediately
tagged and transported or given life-saving interventions. One person performs
the initial triage while other emergency services personnel perform life-saving
mea-sures (eg, intubation) and transport patients. Although emergency medical
services personnel carry out initial field triage, secondary and continuous
triage at all subsequent levels of care is essential.
Staff should control all entrances to the acute care
facility so that incoming patients are directed to the triage area first. The
triage area may be outside the entry or just at the door of the ED. This allows
all patients, including those arriving by medical trans-port and those who walk
in, to be triaged. Some patients already seen in the field will be reclassified
in the triage area, based on their current presentation.
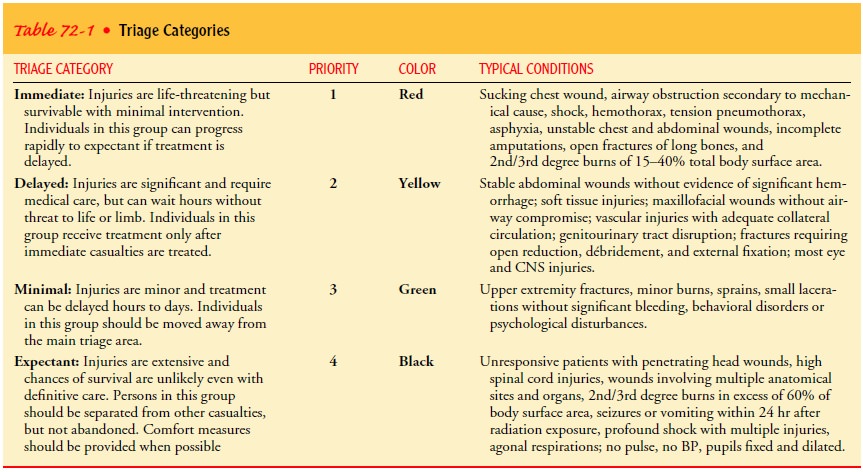
TRIAGE CATEGORIES
Triage categories
separate patients according to severity of injury and use a color-coded tagging
system so that the triage category is immediately obvious. There are several
triage systems in use across the country, and every nurse should be aware of
the system used by his or her facility and community. The North Atlantic Treaty
Organization (NATO) triage system is one that is widely used and is presented
here. It consists of four colors—red, yellow, green, and black. Each color
signifies a different level of priority. Table 72-1 describes each category and
gives examples of how dif-ferent injuries would be classified.
Managing Internal Problems
Each facility must
determine its supply lists based on its own needs assessment. The Red Cross has
developed a basic survival/ shelter resource kit. The EOP committee should
determine the top 10 critical medications used during normal day-to-day
operations and then anticipate which other medications may be required in a
disaster or an MCI. For example, the hospital might plan to have available a
stockpile of cyanide kits or antibiotics used in treating biological agents.
Information should be avail-able about local resources for stocking or
restocking any of the basic and special supplies, how those supplies are
requested, and the time required to receive those supplies.
Communicating With the Media and Family
Communication is a key component of disaster management.
Communication within the vast team of disaster responders is paramount;
however, effective, informative communication with the media and worried family
members is also crucial.
MANAGING MEDIA REQUESTS FOR INFORMATION
Although the media have
an obligation to report the news and can play a significant positive role in
communication, the number of reporters, newscasters, and their support teams
can be over-whelming, possibly compromising operations and patient
confi-dentiality. A clearly defined process for managing the media, which
includes a designated spokesperson, a site for the dissemination of information
(away from patient care areas), and a regular sched-ule for providing updates
should be part of the disaster plan.
Such a plan helps to prevent the release of contradictory or in-accurate information. Initial statements should focus on current efforts and what is being done to better understand the scope and impact of the situation. Information about casualties should not be released. Security staff should not allow media personnel access to patient care areas.
CARING FOR FAMILIES
Friends and family
members converging on the scene must be cared for by the facility. They may be
feeling intense anxiety, shock, or grief and should be provided with
information and up-dates about their loved ones as soon as possible and
regularly thereafter. They should not be in the triage or treatment areas, but
in a designated area staffed by available social service workers, counselors,
therapists, or clergy. Access to this area should be con-trolled to prevent
families from being disturbed. See Chart 72-2 for a discussion of cultural
variables to consider when coping with disaster-related injuries and death.

The Role of Nursing in Disaster Response Plans
The role of the nurse during a disaster varies. The nurse
may be asked to perform outside his or her area of expertise and may take on
responsibilities normally held by physicians or advanced prac-tice nurses. For
example, a critical care nurse may intubate a pa-tient or even insert chest
tubes. Wound débridement or suturing may be performed by staff registered
nurses. A nurse may serve as the triage officer.
Although the exact role of a nurse in disaster management
depends on the specific needs of the facility at the time, it should be clear
which nurse or physician is in charge of a given patient care area and which
procedures each individual nurse may or may not perform. Assistance can be
obtained through the incident command center, and nonmedical personnel can
provide services where possible. For example, family members can provide
nonskilled interventions for their loved ones. Nurses should remember that
nursing care in a disaster focuses on essential care from a perspective of what
is best for all patients.
New settings and atypical roles for nurses arise during a
disaster: the nurse may provide shelter care in a temporary housing area, or
bereavement support and assistance with identification of de-ceased loved ones.
Individuals may require crisis intervention, or the nurse may participate in
counseling other staff members and in critical incident stress management
(CISM). At-risk popula-tions may also require special considerations during a
disaster (Chart 72-3).

CONSIDERING ETHICAL CONFLICTS
Disasters represent a disparity between the resources of the health care agency and the needs of the victims. This generates ethical dilemmas for the nurses and other providers of care. Issues in-clude conflicts related to
·
Rationing care
·
Futile therapy
·
Consent
·
Duty
·
Confidentiality
·
Resuscitation
·
Assisted suicide
Nurses may find it
difficult to not provide medical care to the dying, or to withhold information
to avoid spreading fear and panic. Clinical scenarios that are unimaginable in
normal cir-cumstances, confront the nurse in extreme instances. Other eth-ical
dilemmas may arise out of health care providers’ instinct for self-protection
and protection of their families. For example, what should a pregnant nurse do
when incoming disaster victims have been exposed to radiation, yet too few nurses
are available?
Nurses can plan for the
ethical dilemmas they will face during disasters by establishing a framework
for evaluating ethical ques-tions before they arise and by identifying and
exploring possible responses to difficult clinical situations. They can
consider how the fundamental ethical principles of utilitarianism, beneficence,
and justice will influence their decisions and care in disaster response.
MANAGING BEHAVIORAL ISSUES
Although most people pull together and function during a
dis-aster, both individuals and communities suffer immediate and sometimes
long-term psychological trauma. Common responses to disaster include
·
Depression
·
Anxiety
·
Somatization (fatigue, general
malaise, headaches, gastro-intestinal disturbances, skin rashes)
·
Posttraumatic stress disorder
·
Substance abuse
·
Interpersonal conflicts
·
Impaired performance
Factors that influence
an individual’s response to disaster in-clude the degree and nature of the
exposure to the disaster, loss of friends and loved ones, existing coping
strategies, available re-sources and support, and the personal meaning attached
to the event. Other factors, such as loss of home and valued possessions,
extended exposure to danger, and exposure to toxic contamina-tion, also
influence response and increase the risk of adjustment problems. Those exposed
to the dead and injured, eyewitnesses and those endangered by the event, the
elderly, children, emergency first-responders, and medical personnel caring for
victims are considered to be at higher risk for emotional sequelae.
Nurses can assist
disaster victims by providing active listening and emotional support, giving
information, and referring pa-tients to a therapist or social worker. Health
care workers must refer individuals to mental health care services, because
experi-ence has shown that few disaster victims seek these services and early
intervention minimizes psychological consequences. Nurses can also discourage
victims from subjecting themselves to re-peated exposure to the event through
media replays and news ar-ticles, and encourage them to return to normal
activities and social roles when appropriate.
Critical Incident Stress Management (CISM)
CISM is an approach to preventing and treating the
emotional trauma that can affect emergency responders as a consequence of their
jobs and that can also occur to anyone involved in a disaster or MCI. Critical
incident stress management is handled by CISM teams that are available to the
OEM. There are 350 such teams in the United States. All branches of emergency
services have CISM teams, as do the military and many industries (eg, airline
industry).
Components of a management plan include education before
an incident about critical incident stress and coping strategies; field support
(ensuring that staff get adequate rest, food and fluids, and rotating work
loads) during an incident; and defus-ings, debriefings, demobilization, and
follow-up care after the incident.
Defusing is a process by
which the individual receives education about recognition of stress reactions
and management strategies for handling stress. Debriefing is a more complicated
interven-tion; it involves a 2- to 3- hour process during which participants
are asked about their emotional reactions to the incident, what symptoms they
may be experiencing (eg, flashbacks, difficulty sleeping, intrusive thoughts),
and other psychological ramifica-tions. In follow-up, members of the CISM team
contact the par-ticipants of a debriefing and schedule a follow-up meeting if
necessary. People with ongoing stress reactions are referred to mental health
specialists.
Related Topics