Chapter: Medical Immunology: Immune Complex Diseases
Immune Complex Diseases
Immune Complex Diseases
INTRODUCTION
The formation of circulating antigen-antibody (Ag.Ab) complexes is one of the natural events that characterize the immunological response against soluble antigens. Normally, immune complexes (IC) formed by soluble proteins and their respective antibodies are promptly phagocytized and eliminated from circulation without any detectable adverse effects on the host. However, there are well-characterized clinical and experimental situa-tions in which it has been proven that IC play a pathogenic role.
In the late 1800s and early 1900s, passive immunization with equine antisera was a common therapy for severe bacterial infections. It was often noted that 1–2 weeks after ad-ministration of the horse antisera, when the symptoms of acute infection had often disap-peared, the patient would start to complain of athralgias, exanthematous rash, and had proteinuria and an abnormal urinary sediment, suggestive of glomerulonephritis. Von Pirquet coined the term serum sickness to designate this condition.
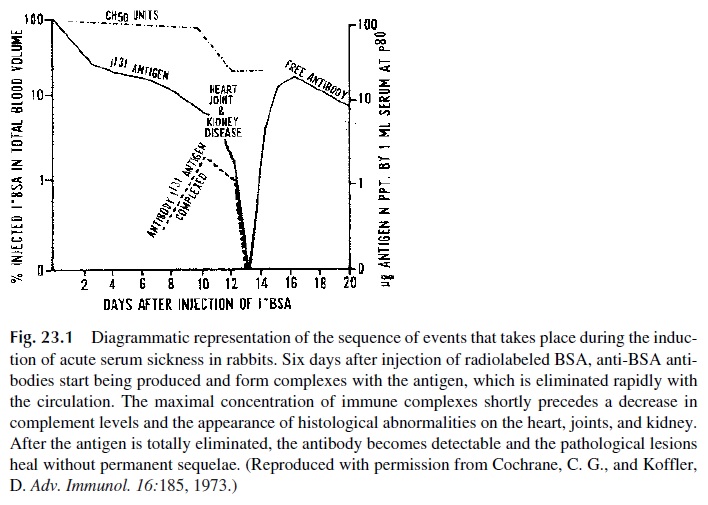
Several decades later, Germuth, Dixon, and coworkers carried out detailed studies in rabbits on which serum sickness was induced by injection of single doses of heterologous proteins. As summarized in Figure 23.1, after the lag time necessary for an-tibody production, soluble immune complexes were detected in serum, serum complement levels decreased, and the rabbits developed glomerulonephritis, myocarditis, and arthritis. The onset of disease coincided with the disappearance of circulating anti-gen, while free circulating antibody appeared in circulation soon after the beginning of symptoms.
Both the experimental one-shot serum sickness and human serum sickness are usu-ally transient and will leave no permanent sequelae. However, if the organism is chroni-cally exposed to antigen (as in chronic serum sickness), irreversible lesions will develop.
Related Topics