Chapter: Basic Radiology : Imaging of Joints
Imaging of Joints: Technique Selection
TECHNIQUE SELECTION
Radiography should always be the
initial imaging test to eval-uate the joints and should be obtained after the
patient has had a thorough history and physical examination and there is a
clear indication to obtain the study. Various projections may be used depending
on the clinical indication or the sit-uation, but at least two orthogonal
projections should be obtained. Often radiographs alone will confirm or refute
the clinical diagnosis. In many instances, however, it may be necessary to use
more sophisticated imaging techniques to clarify the radiographic findings or
to further evaluate de-pending on the clinical scenario. The following
paragraphs discuss the selection of the imaging techniques in a few com-mon
clinical scenarios.
Congenital Diseases
Conventional radiographs should
be the initial modality of choice when confronted with a possible congenital
anomaly or pediatric joint abnormality, or in a child presenting with a limp.
Given that the joint structures
are not well mineralized in children, further evaluation of the joint with
ultrasonography or MR imaging is often required to make a definitive
diagno-sis, as these modalities have superior soft-tissue resolution. If MR
imaging facilities are not available, congenital abnormali-ties can be
investigated with a combination of conventional radiography, ultrasonography,
and CT.
Acute Trauma
In acute trauma, the conventional
radiograph remains the mainstay of the initial imaging assessment. If fractures
are identified, additional imaging will depend on the needs of the clinician or
sub-specialist physician as dictated by the clinical situation. Generally,
fractures that extend into the joint surface (intraarticular fractures) are
treated with greater concern because of the importance of reestablishing the
in-tegrity of the joint. Intraarticular fractures are frequently treated by
operative reduction and internal fixation, espe-cially if the fracture
fragments are severely displaced. CT examination of the injured limb and joints
is used preoper-atively for surgical planning and postoperatively to assess the
results of surgical intervention. The advantages of CT are that it enables
precise assessment of joint reconstitution and also identifies any
intraarticular bone fragments or en-trapped tendons that could interfere with
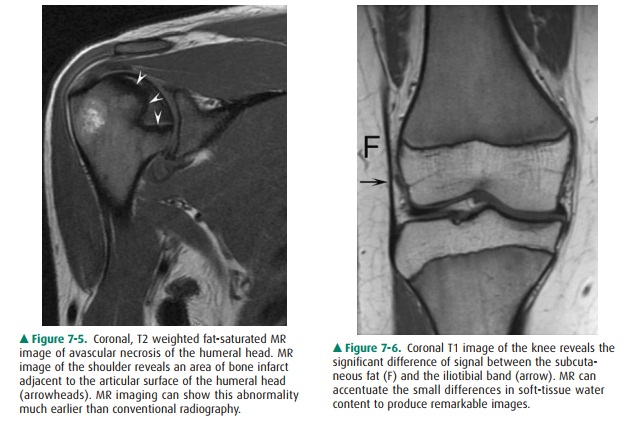
proper reduction and healing (see Figure 7-4).
Subacute and Remote Trauma
Conventional radiographs are used
initially to determine the integrity of the joint. If the joint is normal and
there is a per-sistent clinical suspicion of injury, MR imaging should be
employed because of its superior soft-tissue contrast and res-olution. It is,
therefore, particularly suited for investigation of the intraarticular and
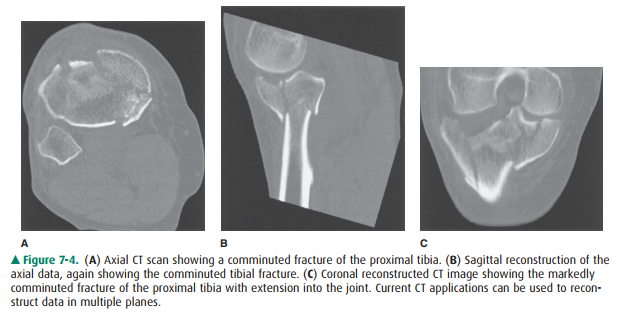
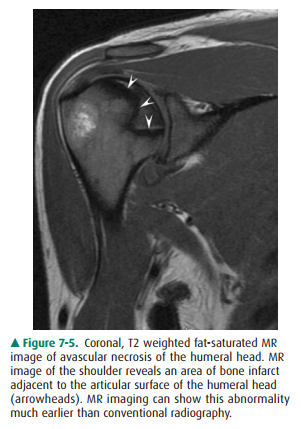
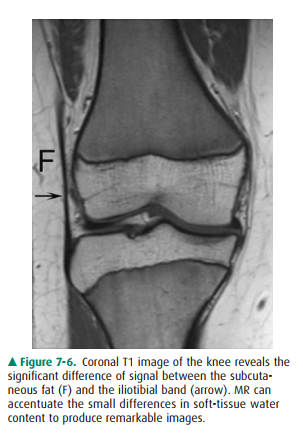
periarticular soft-tissue structures and cartilage (see Figures 7-5, 7-6).
Nontraumatic Cases
Likewise, if the initial
conventional radiographs are normal, MR imaging is the next modality of choice
in the patient with a painful joint. MR imaging may detect evidence of a small
joint effusion, inflamed synovium, and subtle erosions that could suggest the
diagnosis of an inflammatory arthropathy or a septic joint. Percutaneous joint
aspiration of synovial fluid, often fluoroscopically guided, may result in
confirma-tion of infection or yield abnormal crystal deposits within the joint,
such as with gout.
Radiologic Findings
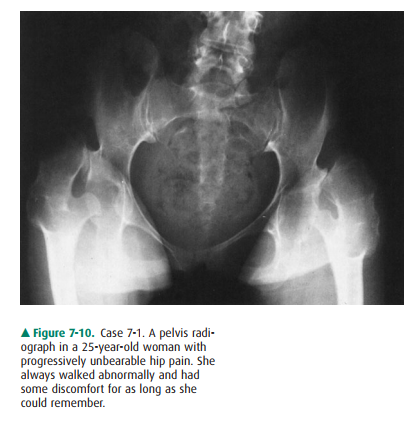
7-1. Both hips in the patient in this case (Figure 7-10) are
abnormal. The femoral heads and necks are mal-formed and dislocated from the
acetabula fossae su-periorly. The acetabulae are also malformed and oriented
more vertically than normal. The patient had bilateral congenital dislocation
of the hips that had been ignored by her parents (A is the correct an-swer to
Question 7-1). This diagnosis should have been made at birth or shortly
thereafter so that cor-rective therapy could have been instituted.
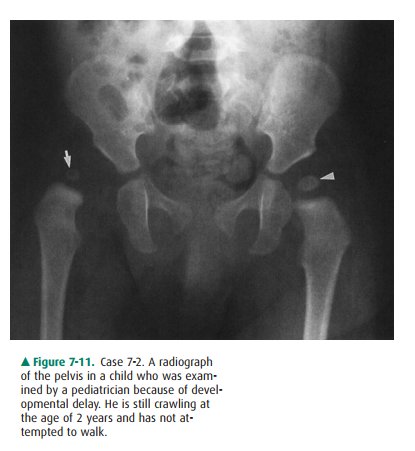
7-2. In this case (Figure 7-11), the capital femoral epi-physis on
the right (arrow) is laterally displaced and smaller than the left epiphysis
(arrowhead). The acetabular fossa on the right side is also mal-formed and more
vertical than the one on the left. The normal development of the acetabulum is
de-pendent on a normally located femoral head, and this is the explanation for
this abnormality. These findings are the classical radiographic features of
developmental dysplasia of the hip (DDH). When this finding is encountered, MR
imaging is the next most appropriate imaging test (B is the correct an-swer to
Question 7-2).
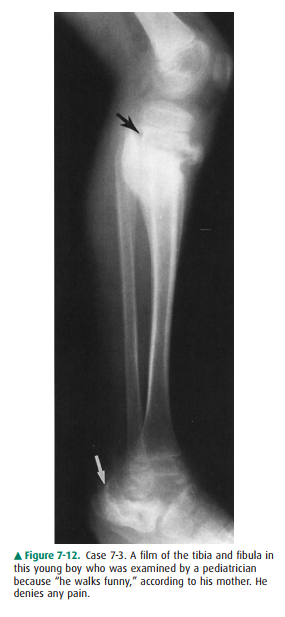
7-3. In this case
(Figure 7-12), the calcaneus is de-formed (white arrow). The talus is poorly
visual-ized because of its complete dislocation from its normal position below
the tibia, and there are sub-luxations at the tibiotalar, talocalcaneal, and
talonav-icular joints. There is overall frank disorganization of this ankle
joint, and clinically there was diffuse soft-tissue swelling around the ankle
(not appreci-ated on this lateral film). There is also a metaphy-seal fracture
of the proximal tibia with exuberant periosteal/callus formation (black arrow).
All of these findings in this patient are caused by chronic repetitive trauma
in a patient with congenital insensitivity to pain (D is the correct answer to
Question 7-3).
Discussion
Congenital joint disorders are
uncommonly encountered, but they should be diagnosed as early as possible after
birth because delayed diagnosis complicates management. Some of the more common
congenital joint disorders include:
A.
Congenital dislocation of the hips
B.
Arthrogryposis multiplex congenita
C.
Congenital insensitivity to pain (asymbolia)
Congenital hip dislocation is
actually a bone dysplasia manifesting as a joint disorder. The femoral head is
dysplastic and does not provide adequate stimulation for proper development of
the acetabulum. Usually, the femoral head is displaced laterally out of an
unusually shal-low (ie, more vertically oriented) acetabulum (Figure 7-11). Once
the diagnosis of DDH is confirmed, treatment should begin at birth or in the
perinatal period to minimize complications.
Historically, hip arthrograms
were used to define the lo-cation of the femoral head in the neonate because
the struc-ture is cartilaginous at birth and therefore radiolucent.
Ultrasonography is an excellent test to assist in the diagno-sis of DDH in
utero and in the neonatal period because it re-quires no ionizing radiation.
However, the interpretation of ultrasound is observer dependent, and the
diagnosis and char-acterization of DDH can be difficult at times. MR imaging
can show the soft-tissue and osseous structures, as well as the articular
cartilage, and is currently the modality of choice in the evaluation of DDH. If
patients are not treated or are incompletely treated, they will eventually
develop secondary, premature osteoarthritis. MR imaging offers limited
diagnostic value over conventional radiographs in late-stage disease.
Proximal focal femoral deficiency
(PFFD) is a disease of uncertain etiology that is characterized by congenital
absence of a segment or all of the proximal third of the femur. The in-cidence
is higher in children of diabetic mothers, and there is also an association
with congenital hip dysplasia. MR imag-ing is also the imaging modality of
choice in evaluating chil-dren with these disorders.
Arthrogryposis multiplex
congenita is a noninheritable congenital disease of uncertain etiology
characterized by multiple joint contractures. It is believed to be due to
neuro-muscular events occurring in utero. The joints of the lower limb are
almost invariably affected. There may be other asso-ciated extraskeletal
congenital anomalies.
A neuropathic joint is caused by
chronic repetitive trauma in the setting of impaired or absent sensation. The
characteristic features of neuropathic joint include soft-tissue swelling,
fragmentation of the bony structures, and general disorganization of the joint.
Joint effusion is often present. The more common causes of neuropathic joints
in the lower extremities include diabetes mellitus and tabes dorsalis
(neurosyphilis). Asymbolia or congenital insensitiv-ity to pain, as exhibited
in Case 7-3 (Figure 7-12), is a group of uncommon congenital disorders in which
there is a vari-able degree of loss of pain sensation and is an unusual cause
of neuropathic joints. Patients with asymbolia almost always acquire
deformities of the extremities after repeated trauma. This diagnosis should be
considered in the young patient with multiple healing fractures with
soft-tissue swelling and joint disorganization in whom nonaccidental trauma has
been excluded.
Related Topics