Chapter: Essentials of Anatomy and Physiology: The Heart
Heart Chambers-Vessels and Valves
CHAMBERS - VESSELS AND VALVES
The walls of the four chambers of the heart are made of cardiac muscle called the myocardium. The cham-bers are lined withendocardium, simple squamous epithelium that also covers the valves of the heart and continues into the vessels as their lining (endothe-lium). The important physical characteristic of the endocardium is not its thinness, but rather its smooth-ness. This very smooth tissue prevents abnormal blood clotting, because clotting would be initiated by contact of blood with a rough surface.
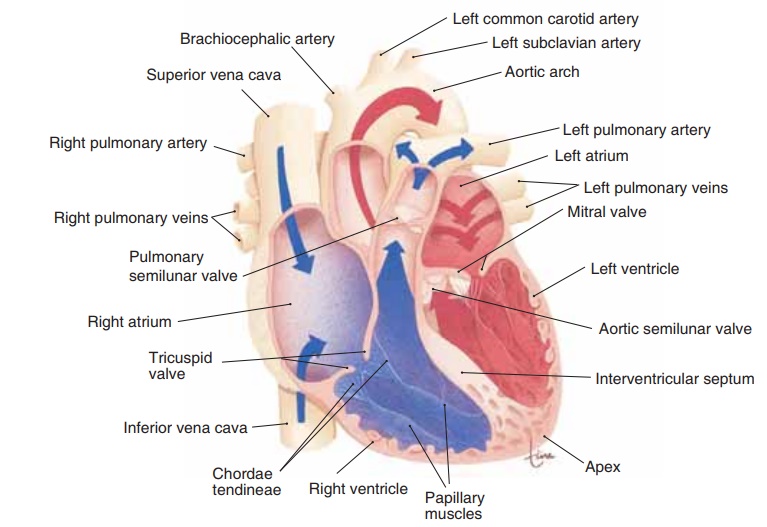
The upper chambers of the heart are the right and left atria (singular: atrium), which have relatively thin walls and are separated by a common wall of myocar-dium called the interatrial septum. The lower cham-bers are the right and left ventricles, which have thicker walls and are separated by the interventricu-lar septum (Fig. 12–2). As you will see, the atria receive blood, either from the body or the lungs, and the ventricles pump blood to either the lungs or the body.
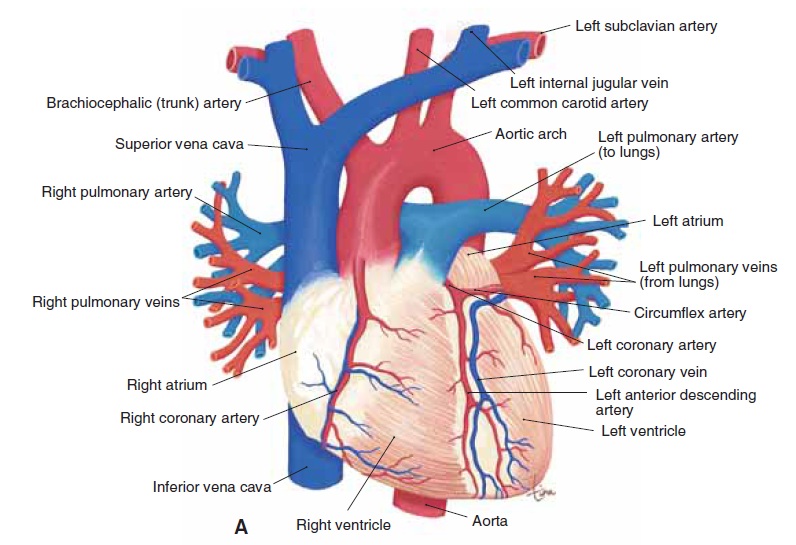
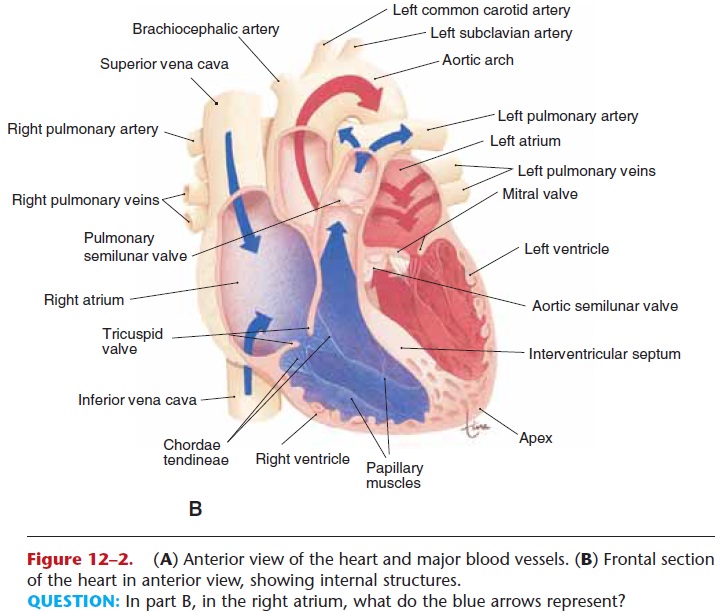
Figure 12–2. (A) Anterior view of the heart and major blood vessels. (B) Frontal section of the heart in anterior view, showing internal structures.
QUESTION: In part B, in the right atrium, what do the blue arrows represent?
RIGHT ATRIUM
The two large caval veins return blood from the body to the right atrium (see Fig. 12–2). The superior vena cava carries blood from the upper body, and the infe-rior vena cava carries blood from the lower body. From the right atrium, blood will flow through theright atrioventricular (AV) valve, or tricuspid valve, into the right ventricle.
The tricuspid valve is made of three flaps (or cusps) of endocardium reinforced with connective tissue. The general purpose of all valves in the circulatory system is to prevent backflow of blood. The specific purpose of the tricuspid valve is to prevent backflow of blood from the right ventricle to the right atrium when the right ventricle contracts. As the ventricle contracts, blood is forced behind the three valve flaps, forcing them upward and together to close the valve.
LEFT ATRIUM
The left atrium receives blood from the lungs, by way of four pulmonary veins. This blood will then flow into the left ventricle through the left atrioventricular (AV) valve, also called the mitral valve or bicuspid (two flaps) valve. The mitral valve prevents backflow of blood from the left ventricle to the left atrium when the left ventricle contracts.
Another function of the atria is the production of a hormone involved in blood pressure maintenance. When the walls of the atria are stretched by increased blood volume or blood pressure, the cells produce atrial natriuretic peptide (ANP), also called atrial natriuretic hormone (ANH). (The ventricles of the heart produce a similar hormone called B-type natri-uretic peptide, or BNP, but we will use ANP as the representative cardiac hormone.) ANP decreases the reabsorption of sodium ions by the kidneys, so that more sodium ions are excreted in urine, which in turn increases the elimination of water. The loss of water lowers blood volume and blood pressure. You may have noticed that ANP is an antagonist to the hor-mone aldosterone, which raises blood pressure.
RIGHT VENTRICLE
When the right ventricle contracts, the tricuspid valve closes and the blood is pumped to the lungs through the pulmonary artery (or trunk). At the junction of this large artery and the right ventricle is the pulmonary semilunar valve (or more simply, pulmonary valve). Its three flaps are forced open when the right ventri-cle contracts and pumps blood into the pulmonary artery. When the right ventricle relaxes, blood tends to come back, but this fills the valve flaps and closes the pulmonary valve to prevent backflow of blood into the right ventricle.
Projecting into the lower part of the right ventricle are columns of myocardium called papillary muscles (see Fig. 12–2). Strands of fibrous connective tissue, the chordae tendineae, extend from the papillary muscles to the flaps of the tricuspid valve. When the right ventricle contracts, the papillary muscles also contract and pull on the chordae tendineae to prevent inversion of the tricuspid valve. If you have ever had your umbrella blown inside out by a strong wind, you can see what would happen if the flaps of the tricuspid valve were not anchored by the chordae tendineae and papillary muscles.
LEFT VENTRICLE
The walls of the left ventricle are thicker than those of the right ventricle, which enables the left ventricle to contract more forcefully. The left ventricle pumps blood to the body through the aorta, the largest artery of the body. At the junction of the aorta and the left ventricle is the aortic semilunar valve (or aortic valve) (see Fig. 12–2). This valve is opened by the force of contraction of the left ventricle, which also closes the mitral valve. The aortic valve closes when the left ventricle relaxes, to prevent backflow of blood from the aorta to the left ventricle. When the mitral (left AV) valve closes, it prevents backflow of blood to the left atrium; the flaps of the mitral valve are also anchored by chordae tendineae and papillary muscles.
All of the valves are shown in Fig. 12–3, which also depicts the fibrous skeleton of the heart. This is fibrous connective tissue that anchors the outer edges
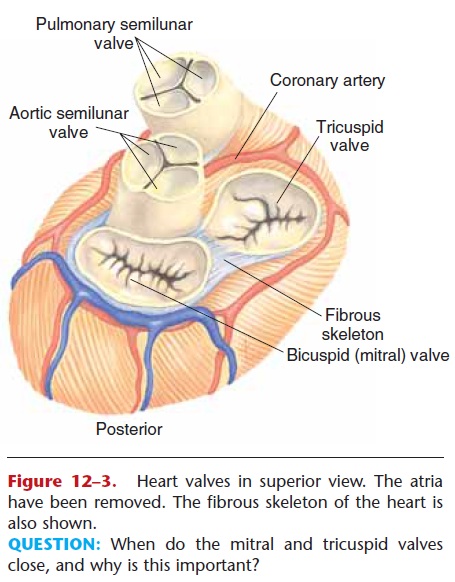
Figure 12–3. Heart valves in superior view. The atria have been removed. The fibrous skeleton of the heart is also shown.
QUESTION: When do the mitral and tricuspid valves close, and why is this important?
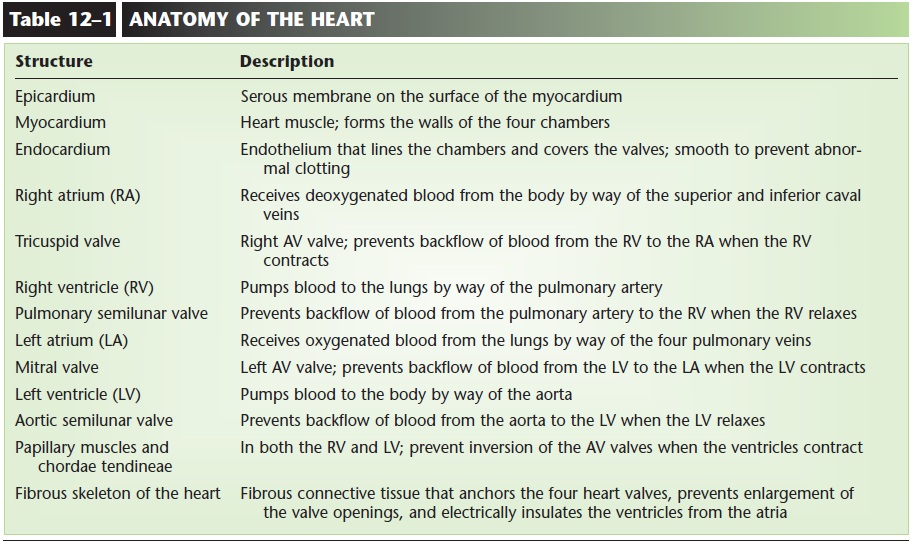
As you can see from this description of the cham-bers and their vessels, the heart is really a double, or two-sided, pump. The right side of the heart receives deoxygenated blood from the body and pumps it to the lungs to pick up oxygen and release carbon diox-ide. The left side of the heart receives oxygenated blood from the lungs and pumps it to the body. Both pumps work simultaneously; that is, both atria con-tract together, followed by the contraction of both ventricles. Aspects of the anatomy of the heart are summarized in Table 12–1.
Related Topics