Chapter: Obstetrics and Gynecology: Ovarian and Adnexal Disease
Functional Ovarian Cysts
FUNCTIONAL OVARIAN CYSTS
Functional ovarian cysts are not neoplasms, but,
rather,anatomic variations that arise as a result of normal ovarian function. They may
present as an asymptomatic adnexalmass or become symptomatic, requiring
evaluation and possibly treatment.
When an ovarian follicle fails to
rupture during follic-ular maturation, ovulation does not occur, and a follicularcyst may develop. This
process, by definition, involves alengthening of the follicular phase of the
cycle, with resul-tant transient secondary amenorrhea. Follicular cysts are
lined by normal granulosa cells, and the fluid contained in them is rich in
estrogen.
A follicular cyst becomes
clinically significant if it is large enough to cause pain or if it persists
beyond one men-strual interval. For poorly understood reasons, the granulosa
cells lining the follicular cyst persist through the time when ovulation should
have occurred and continue to enlarge through the second half of the cycle. A
cyst may enlarge beyond 5 cm and continue to fill with follicular fluid from
the thickened granulosa cell layer. Symptoms associated with a follicular cyst
may include mild to moderate uni-lateral lower abdominal pain and alteration of
the menstrual interval. The latter may be the result of both failed sub-sequent
ovulation and bleeding stimulated by the large amount of estradiol produced in
the follicle. This hormonal environment, along with the lack of ovulation,
overstimu-lates the endometrium and causes irregular bleeding. Pelvic
examination findings may include unilateral tenderness with a palpable, mobile,
cystic adnexal mass.
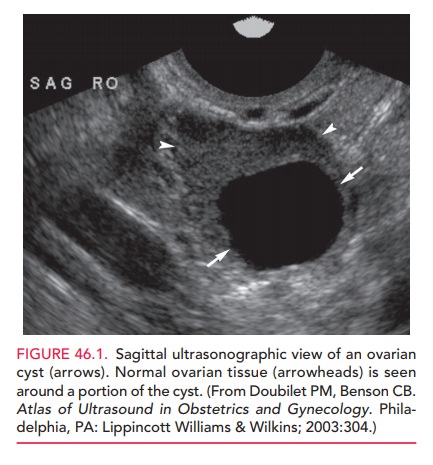
Pelvic ultrasonography is often warranted in reproduc-tive-age patients who have cysts larger than 5 cm in diame-ter. Ultrasound characteristics of benign tumors include unilocular simple cyst without evidence of thick septa-tions, soft tissue elements, or evidence of internal or exter-nal excrescences (Fig. 46.1). For many patients, however, ultrasound confirmation is not required. Instead, the patient may be reassured and followed with a repeat pelvic examination in about 6 weeks, once pregnancy has been ruled out.
Most follicular cysts
spontaneously resolve during this time. Alternatively, an estrogen- and
progesterone-containing oral contraceptive may be given to suppress
gonadotropin stimulation of the cyst. Although this prac-tice has not been
shown to “shrink” the existing follicu-lar cyst, it may suppress the
development of a new cyst and permit resolution of the existing problem. If the
cyst per-sists despite expectant management, another type of cyst or neoplasm
should be suspected and further evaluated by imaging studies and/or surgery.
On occasion, rupture of a
follicular cyst may cause acute pelvic pain. Because release of follicular
fluid into the peritoneum produces only transient symptoms, surgical
intervention is rarely necessary.
Corpus luteum cyst is the other common type of
func-tional ovarian cyst, designated a cyst rather than simply a cor-pus luteum
when its diameter exceeds about 3 cm. It is
relatedto the postovulatory (i.e., progesterone-dominant) phase of the
menstrual cycle. Two variations of corpus luteum cysts are encountered. The
first is a slightly enlarged cor-pus luteum, which may continue to produce
progesterone for longer than the usual 14 days. Menstruation is delayed from a
few days to several weeks, although it usually occurs within 2 weeks of the
missed period. Persistent cor-pus luteum cysts are often associated with dull
lower-quadrant pain. This pain and a missed menstrual period are the most
common complaints associated with persis-tent corpus luteum cysts. Pelvic
examination usually dis-closes an enlarged, tender, cystic, or solid adnexal
mass. Because of the triad of missed menstrual period, unilateral
lower-quadrant pain, and adnexal enlargement, ectopic pregnancy is often
considered in the differential diagno-sis. A negative pregnancy test eliminates
this possibility, whereas a positive pregnancy test mandates further
evalu-ation regarding the location of the pregnancy. Patients with recurrent
persistent corpus luteum cysts may benefit from cyclic oral contraceptive
therapy.
The second less-common type of
corpus luteum cyst is the rapidly enlarging luteal-phase cyst into which there is spontaneous hemorrhage.
Sometimes called the corpushemorrhagicum,
this hemorrhagic corpus luteum cyst mayrupture late in the luteal phase,
resulting in the following clinical picture: a patient not using oral
contraceptives, with regular periods, who presents with acute pain late in the
luteal phase. Some patients present with evidence of hemo-peritoneum as well as
hypovolemia and require surgical resection of the bleeding cyst. In others, the
acute pain and blood loss are self-limited. These patients may be managed with
mild analgesics and reassurance. Patients at risk for repetitive hemorrhagic
corpus luteum cysts include those who are taking anticoagulation medication and
those who have inherent bleeding disorders. This process may be the hallmark to
initiate an investigation for an inherent bleed-ing disorder.
The least common functional cyst
is the theca luteincyst, associated
with pregnancy and usually bilateral. Theyare more common in multiple
gestations, trophoblastic disease, and also with ovulation induction with
clomiphene and human menopausal gonadotropin/human chorionic gonadotropin
(hCG). They may become large and are multicystic, but also regress
spontaneously in most cases without intervention.
Related Topics