Chapter: Introduction to Human Nutrition: Energy Metabolism
Energy intake - Human Nutrition: Energy Metabolism
Energy intake
Sources of dietary energy
As mentioned , the sources of energy in the food we eat include the major macronutrients: protein, car-bohydrate, and fat, as well as alcohol. Carbohydrate and protein provide 16.8 kJ of energy for each gram; alcohol provides 29.4 kJ/g, whereas fat is the most energy dense, providing 37.8 kJ/g. Note that 4.2 kJ is defined as the amount of heat that is required to raise the temperature of 1 liter of water by 1°C. The energy content of food can be measured by bomb calori-metry, which involves combusting a known weight of food inside a sealed chamber and measuring the amount of heat that is released during this process. Thus, 1 g of pure fat would release 37.8 kJ during its complete combustion, whereas 1 g of pure carbohy-drate would release 16.8 kJ. Thus, if the gram quanti-ties of any type of food are known, the energy content can easily be calculated. For example, if a protein-rich nutrition snack contains 21 g of carbohydrate, 6 g of fat, and 14 g of protein, then the total energy content is (21 × 16.8) + (6 ×37.8) + (14 × 16.8) = 814.8 kJ. The macronutrient composition of food is typically assessed in the percentage contribution of each mac-ronutrient to the total number of calories. If a food has a carbohydrate content of 21 g, which is 352.8 kJ, and the total energy content is 820 kJ the proportion of energy derived from carbohydrate is 43%; the fat content is 6 g, or 226.8 kJ, equivalent to 28% of the energy; and the protein contributes 14 g, 235.2 kJ and 29% of the energy.
Regulation of food intake
Appetite, hunger, and satiety
The quality and quantity of food that is consumed are closely regulated by the body. Food intake is regulated by a number of factors involving complex inter-actions among various hormones, neuroendocrine factors, the central nervous system, and organ systems (e.g., brain and liver), and environmental and external factors.
Appetite is usually defined as a psychological desire to eat and is related to the pleasant sensations that are often associated with specific foods. Scientifically, appetite is used as a general term of overall sensations related to food intake.
Hunger is usually defined as the subjective feeling that determines when food consumption is initiated and can be described as a nagging, irritating feeling that signifies food deprivation to a degree that the next eating episode should take place.
Satiety is considered as the state of inhibition over eating that leads to the termination of a meal, and is related to the time interval until the next eating episode. Thus, hunger and satiety are more intrinsic instincts, whereas appetite is often a learned response.
The internal factors that regulate the overall feeling of hunger and satiety include the central nervous system (primarily the hypothalamus and the vagus nerve), the major digestive organs such as the stomach and liver, and various hormones. In addition, envi-ronmental factors (e.g., meal pattern and composi-tion, food availability, smell and sight of foods, climate), emotional factors (e.g., stress), and some diseased states (e.g., anorexia, trauma, infection) may influence the feelings of both hunger and appetite. The factors that influence appetite include factors external to the individual (e.g., climate, weather), specific appetite cravings, specific learned dislikes or avoidance (e.g., alcohol), intrinsic properties of food (e.g., taste, palatability, texture), cultural practices or preferences, specific effects of some drugs and dis-eases, and metabolic factors such as hormones and neurotransmitters. Some of these factors are described in further detail below.
The classic way to describe the complex appetite-regulating system is the satiety cascade put forth by John Blundell. The satiety cascade describes four dis-tinctly different but overlapping categories of mecha-nisms involved in acute within-meal feeling of satiety (referred to as satiation) and the inbetween-meal satiety (Figure 3.1).
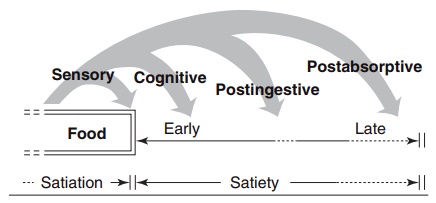
Figure 3.1 The satiety cascade by John Blundell (1987). The four categories of mechanisms are sensory, cognitive, postingestive, and postabsorptive. The sensoric phase includes stimuli mediated via sensory fibers in the cranial nerves and relates to the palatability of the ingested meal including smell, taste, temperature, and texture. The cognitive phase of the satiety cascade represents learned, known, and assumed properties of the ingested food. In the postingestive phase the gastrointestinal tract is involved in a number of satiety signals both via chemo- and mechanoreceptors and appetite-regulating peptides from the gut and pancreas either entering circulation and acting directly in the CNS or signaling via the vagus nerve. Important satiety signals in the postabsorptive phase include circulating nutrients, signals derived from differences in energy turnover, substrate oxida-tion, and neurohormonal factors. Reprinted from Blundell et al. (1987), copyright 1987 with permission of Elsevier.
Factors influencing food intake
Digestive factors
Several factors in the digestive system exert a short-term influence over food intake. The presence of food and drink in the stomach and intestine and the resul-tant pressure that they exert may regulate food intake. This effect is known as gastrointestinal distension. In addition, the stomach produces a hormone called cholecystokinin (CCK) in response to food intake, which may, in turn, regulate food intake. Furthermore, when subjects have fat or carbohydrate infused directly into the small intestine, they report feelings of satiety. This suggests that factors in the intestine regulate food intake. Indeed, receptors in the intes-tine have been identified that recognize the presence of specific macronutrients; these receptors are linked to the brain and therefore can communicate directly with the central nervous system, resulting in regula-tion of energy balance. In addition, other gastrointes-tinal hormones, such as glucagon-like peptide-1 and -2 (GLPs), CCK, and glucose-dependent insulinotro-pic polypeptide (GIP) are likely to play a role in the mediation of gut events and brain perception of hunger and satiety.
Central nervous system factors
The main contributory factor regulating food intake in the central nervous system is the hypothalamus.
The hypothalamus is linked to specific parts of the brain that are known to modify feeding behavior, specifically the paraventricular nuclei and the nigro-striatal tract. These areas of the brain respond to various neurotransmitters as well as sympathetic nervous system activity. In general, food intake will decrease as sympathetic nervous system activity increases, and vice versa.
Circulating factors
After consumption of a meal, food is broken down into its basic components (i.e., carbohydrate is broken down to glucose, protein to amino acids, and fats or triglycerides to glycerol and fatty acids) and the cir-culating levels of some of these breakdown products increase in the blood. Consequently, glucose, amino acids, glycerol, and fatty acids are further metabo-lized, primarily in the liver, or used for immediate energy (e.g., in muscle or brain). There is evidence to suggest that this resultant metabolism, especially in the liver, may in turn regulate food intake. After meal consumption, the circulating levels of nutrients fall (within minutes for glucose, several hours for triglyc-erides) and the feelings of hunger return. The link from nutrient metabolism to central control of food intake occurs through signals from the liver to the brain via the vagus nerve. Thus, circulating factors provide a link between the digestive system and the central nervous system, which provides another system for regulating food intake.
Signals from the periphery
Leptin is a hormone that is produced by fat cells and communicates with the central nervous system through leptin receptors in the hypothalamus. Reduced production of leptin, or lack of sensitivity of the hypo-thalamus to leptin, may regulate food intake and play a key role in the etiology of rare forms of obesity in humans. Leptin and the other peripheral hormones with a central effect on appetite are divided into two broad categories: (1) the so-called adiposity signals, which are tonically active providing information on body fat stores to the CNS and (2) the satiety signals which are released in response to food intake and are thought to be involved in short-term regulation of energy intake. Currently known adiposity signals are insulin, leptin, and adiponectin, which are considered as long-acting signals reducing energy intake. Among the satiety signals are the hunger hormone ghrelin, which is secreted in the stomach, and the short-acting gut- and pancreas-derived satiety signals CCK, peptide YY (PYY), GLP-1, oxyntomodulin (OXM), and pan-creatic polypeptide (PP). Many of the peripheral satiety signals have receptors in the arcuate nucleus (ARC) of the hypothalamus, which plays an impor-tant role in appetite regulation. The ARC contains neuropeptide Y (NPY)- and agouti-related peptide (AgRP)-expressing neurons acting to stimulate food intake along with the adjacent pro-opiomelanocortin (POMC) and cocaine- and amphetamine-regulated transcript (CART)-expressing neurons which inhibit feeding. Besides the ARC, the nucleus of the solitary tract (NTS) and the area postrema (AP) receive appe-tite-regulating inputs from vagal afferents and circu-lating factors and are connected to the hypothalamic nuclei controlling food intake.
External factors
Various nonphysiological or external factors are also known to modify food intake, and these effects may be mediated through the intrinsic factors described above. Psychological factors such as depression may lead to either increased or decreased food intake, or changes in the consumption of specific types of foods. Environmental factors are also important, the most obvious being food availability. Even when food is available, some of the specific properties of foods make them more or less appealing, thereby modifying food intake. Important physical characteristics of food include taste, texture, color, temperature, and presentation. Other cultural influences in the envi-ronment, such as time of day, social factors, peer influence, and cultural preferences, can also play a role in influencing food intake.
Related Topics