Microbiology - Drugs Resistance Mechanisms | 12th Microbiology : Chapter 3 : Control of Microorganisms by Chemical Methods
Chapter: 12th Microbiology : Chapter 3 : Control of Microorganisms by Chemical Methods
Drugs Resistance Mechanisms
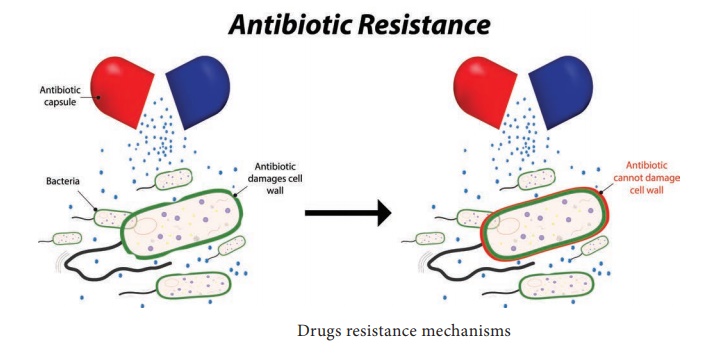
Drugs Resistance Mechanisms
Some
microbes respond predictably to certain drugs making selection of treatment
easy. Other microbes may vary in their responses, and laboratory tests are
usually required to ensure that the selected therapy is appropriate.
Chemotherapeutic effectiveness depends upon the sensitivity of the pathogen to
the agent. Antibiotic resistance, however, may develop in microbes within the
population. In fact, the history of chemotherapy has been closely paralleled by
the history of drug resistance.
None of
the therapeutic drugs (antibiotic) inhibits all microbial pathogens and some
microbial pathogens possess natural ability to resist to certain antibiotics.
Bacteria become drug resistant using several different resistance mechanisms. A
particular type of resistance mechanism is not confined to a single class of
drugs. Two bacteria may employ different resistance mechanisms to counter the
same antibiotic. However, bacteria acquire drugs resistance using resistance
mechanisms such as reduced permeability to antibiotic, efflux (pumping)
antibiotic out of the cell, drug inactivation through chemical modification,
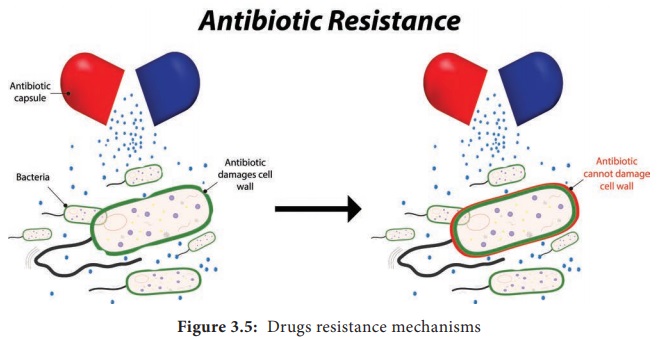
target modification and development of a resistant biochemical pathway (Figure
3.5).
Infobits
Methicillin-resistant staphylococcus aureus (MRSA) is a bacteria
that is resistant to many antiobiotics. Staph and MRSA can cause a variety of
problems ranging from are skin infections and sepsis to pneumonia to blood stream
infections.
Related Topics