Chapter: Medical Physiology: Adrenocortical Hormones
Cortisol is Important in Resisting Stress and Inflammation
Cortisol is Important in Resisting Stress and Inflammation
Almost any type of stress, whether physical or neurogenic, causes an immediate and marked increase in ACTH secretion by the anterior pituitary gland, followed within minutes by greatly increased adreno-cortical secretion of cortisol. This is demonstrated dramatically by the experiment shown in Figure 77–5, in which corticosteroid formation and secretion increased sixfold in a rat within 4 to 20 minutes after fracture of two leg bones.
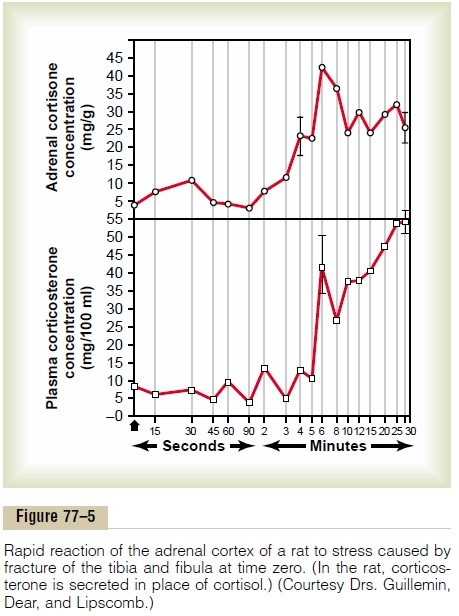
Some of the different types of stress that increase cortisol release are the following:
1. Trauma of almost any type
2. Infection
3. Intense heat or cold
4. Injection of norepinephrine and other sympathomimetic drugs
5. Surgery
6. Injection of necrotizing substances beneath the skin
7. Restraining an animal so that it cannot move
8. Almost any debilitating disease
Even though we know that cortisol secretion often increases greatly in stressful situations, we are not sure why this is of significant benefit to the animal. One possibility is that the glucocorticoids cause rapid mobi-lization of amino acids and fats from their cellular stores, making them immediately available both for energy and for synthesis of other compounds, includ-ing glucose, needed by the different tissues of the body. Indeed, it has been shown in a few instances that damaged tissues that are momentarily depleted of pro-teins can use the newly available amino acids to form new proteins that are essential to the lives of the cells.
Also, the amino acids are perhaps used to synthesize other essential intracellular substances such as purines, pyrimidines, and creatine phosphate, which are neces-sary for maintenance of cellular life and reproduction of new cells.
But all this is mainly supposition. It is supported only by the fact that cortisol usually does not mobilize the basic functional proteins of the cells, such as the muscle contractile proteins and the proteins of neurons, until almost all other proteins have been released. This preferential effect of cortisol in mobilizing labile proteins could make amino acids available to needy cells to synthesize substances essen-tial to life.
Anti-inflammatory Effects of High Levels of Cortisol
When tissues are damaged by trauma, by infection with bacteria, or in other ways, they almost always become “inflamed.” In some conditions, such as in rheumatoid arthritis, the inflammation is more dam-aging than the trauma or disease itself. The adminis-tration of large amounts of cortisol can usually block this inflammation or even reverse many of its effects once it has begun. Before attempting to explain the way in which cortisol functions to block inflammation, let us review the basic steps in the inflammation process.
There are five main stages of inflammation: (1) release from the damaged tissue cells of chemical substances that activate the inflammation process-chemicals such as histamine, bradykinin, proteolytic enzymes, prostaglandins, and leukotrienes; (2) an increase in blood flow in the inflamed area caused by some of the released products from the tissues, an effect called erythema; (3) leakage of large quantities of almost pure plasma out of the capillaries into the damaged areas because of increased capillary perme-ability, followed by clotting of the tissue fluid, thus causing a nonpitting type of edema; (4) infiltration of the area by leukocytes; and (5) after days or weeks, ingrowth of fibrous tissue that often helps in the healing process.
When large amounts of cortisol are secreted or injected into a person, the cortisol has two basic anti-inflammatory effects: (1) it can block the early stagesof the inflammation process before inflammation even begins, or (2) if inflammation has already begun, it causes rapid resolution of the inflammation and increased rapidity of healing. These effects are explained further as follows.
Cortisol Prevents the Development of Inflammation by Stabiliz-ing Lysosomes and by Other Effects. Cortisol has the fol-lowing effects in preventing inflammation:
1. Cortisol stabilizes the lysosomal membranes. Thisis one of its most important anti-inflammatory effects, because it is much more difficult than normal for the membranes of the intracellular lysosomes to rupture. Therefore, most of the proteolytic enzymes that are released by damaged cells to cause inflammation, which are mainly stored in the lysosomes, are released in greatly decreased quantity.
2. Cortisol decreases the permeability of the capillaries, probably as a secondary effect of thereduced release of proteolytic enzymes. This prevents loss of plasma into the tissues.
3. Cortisol decreases both migration of white blood cells into the inflamed area and phagocytosis of the damaged cells. These effects probably result fromthe fact that cortisol diminishes the formation of prostaglandins and leukotrienes that otherwise would increase vasodilation, capillary permeability, and mobility of white blood cells.
4. Cortisol suppresses the immune system, causing lymphocyte reproduction to decrease markedly.The T lymphocytes are especially suppressed. In turn, reduced amounts of T cells and antibodies in the inflamed area lessen the tissue reactions that would otherwise promote the inflammation process.
5. Cortisol attenuates fever mainly because it reducesthe release of interleukin-1 from the white blood cells, which is one of the principal excitants to thehypothalamic temperature control system. The decreased temperature in turn reduces the degree of vasodilation.
Thus, cortisol has an almost global effect in reduc-ing all aspects of the inflammatory process. How much of this results from the simple effect of cortisol in stabilizing lysosomal and cell membranes versus its effect to reduce the formation of prostaglandins and leukotrienes from arachidonic acid in damaged cell membranes and other effects of cortisol is unclear.
Cortisol Causes Resolution of Inflammation. Even afterinflammation has become well established, the admin-istration of cortisol can often reduce inflammation within hours to a few days. The immediate effect is to block most of the factors that are promoting the inflammation. But in addition, the rate of healing is enhanced. This probably results from the same, mainly undefined, factors that allow the body to resist many other types of physical stress when large quantities of cortisol are secreted. Perhaps this results from the mobilization of amino acids and use of these to repair the damaged tissues; perhaps it results from the increased glucogenesis that makes extra glucose avail-able in critical metabolic systems; perhaps it results from increased amounts of fatty acids available for cel-lular energy; or perhaps it depends on some effect of cortisol for inactivating or removing inflammatory products.
Regardless of the precise mechanisms by which the anti-inflammatory effect occurs, this effect of cortisol plays a major role in combating certain types of dis-eases, such as rheumatoid arthritis, rheumatic fever, and acute glomerulonephritis. All these diseases are characterized by severe local inflammation, and the harmful effects on the body are caused mainly by the inflammation itself and not by other aspects of the disease.
When cortisol or other glucocorticoids are adminis-tered to patients with these diseases, almost invariably the inflammation begins to subside within 24 hours.
And even though the cortisol does not correct the basic disease condition, merely preventing the damag-ing effects of the inflammatory response, this alone can often be a lifesaving measure.
Related Topics