Chapter: Psychiatric Mental Health Nursing : Grief and Loss
Complicated Grieving
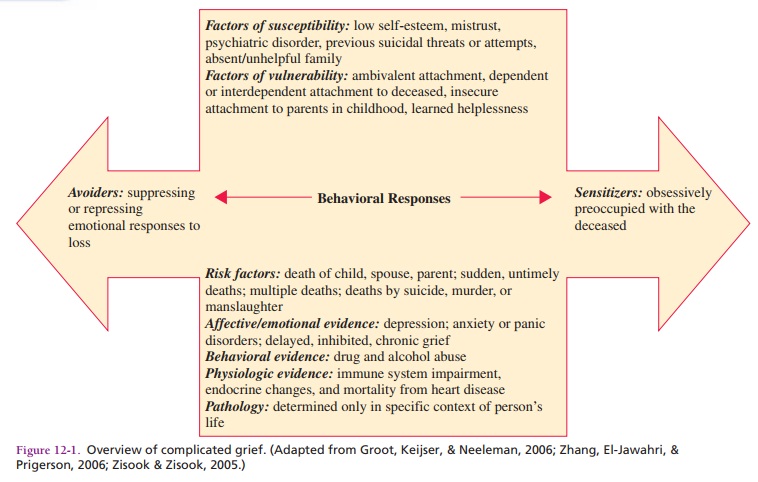
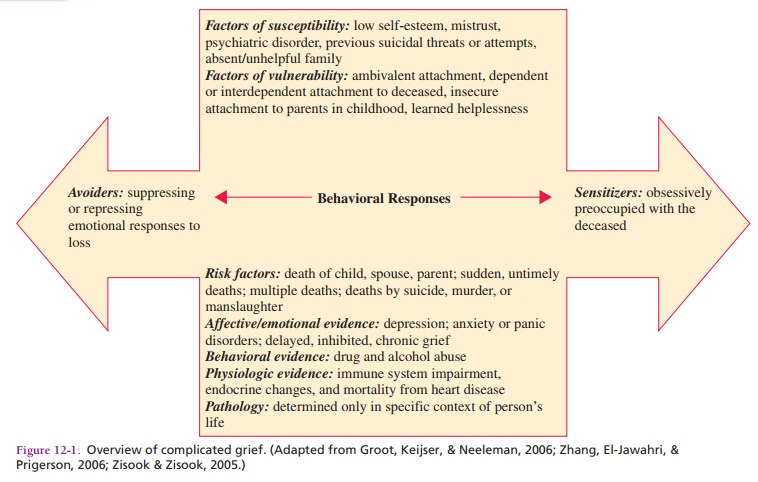
COMPLICATED GRIEVING
Some believe complicated
grieving to be a response out-side the norm, occurring when a person is
void of emo-tion, grieves for prolonged periods, or has expressions of grief
that seem disproportionate to the event. People may suppress emotional
responses to the loss or become obses-sively preoccupied with the deceased
person or lost object. Others actually may suffer from clinical depression when
they cannot make progress in the grief process (Zhang, El-Jawahri, &
Prigerson, 2006). Figure 12.1 depicts an overview of complicated grieving.
Previously existing psychiatric disorders also may com-plicate the
grief process, so nurses must be particularly alert to clients with psychiatric
disorders who also are grieving. Grief can precipitate major depression in a
per-son with a history of the disorder. These clients also can experience grief
and a sense of loss when they encounter changes in treatment settings, routine,
environment, or even staff.
Although nurses must recognize that complications may arise in the
grief process, the process remains unique and dynamic for each person. Immense
variety exists in terms of the cultural determinants in communicating the
experience and the individual differences in emotional reactions, depth of
pain, and time needed to acknowledge and grasp the personal meaning or
assimilate the loss.
Characteristics of Susceptibility
For some, the effects of grief are particularly devastating because
their personalities, emotional states, or situations make them susceptible to
complications during the pro-cess. People who are vulnerable to complicated
grieving include those with the following characteristics:
Low self-esteem
Low truth in others
A previous psychiatric disorder
Previous suicide threats or attempts Absent or unhelpful family
members
An ambivalent, dependent, or insecure attachment to the deceased
person.
·
In an ambivalent attachment,
at least one partner is un-clear about how the couple loves or does not love
each other. For example, when a woman is uncertain about and feels pressure
from others to have an abortion, she is experiencing ambivalence about her
unborn child.
·
In a dependent attachment,
one partner relies on the other to provide for his or her needs without
necessar-ily meeting the partner’s needs.
·
An insecure attachment
usually forms during childhood, especially if a child has learned fear and
helplessness (i.e., through intimidation, abuse, or control by parents).
A person’s perception is another factor contributing to
vulnerability: Perception, or how a person thinks or feels about a situation,
is not always reality. After the death of a loved one, a person may believe
that he or she really can-not continue and is at a great disadvantage. He or
she may become increasingly sad and depressed, not eat or sleep, and perhaps
entertain suicidal thoughts.
Risk Factors Leading to Vulnerability
Zhang, El-Jawahri, and Prigerson (2006) and Zisook and Zisook
(2005) identified experiences that increase the risk![]()
![]() for complicated grieving for the vulnerable
parties previ-ously mentioned. These experiences are related to trauma or individual
perceptions of vulnerability and include the following:
for complicated grieving for the vulnerable
parties previ-ously mentioned. These experiences are related to trauma or individual
perceptions of vulnerability and include the following:
·
Death of a spouse or child
·
Death of a parent (particularly in early childhood or adolescence)
·
Sudden, unexpected, and untimely death
·
Multiple deaths
·
Death by suicide or murder
Based on the experiences previously identified, those most
intimately affected by the terrorist attacks on September 11, 2001 could be
considered at increased risk for complicated grieving.
Complicated Grieving as a Unique and Varied Experience
The person with complicated grieving also can experience
physiologic and emotional reactions. Physical reactions can include an impaired
immune system, increased adre-nocortical activity, increased levels of serum
prolactin and growth hormone, psychosomatic disorders, and increased mortality
from heart disease. Characteristic emotional responses include depression,
anxiety or panic disorders, delayed or inhibited grief, and chronic grief
(Zisook & Zisook, 2005).
Because the grieving process is unique to each person, the nurse
must assess the degree of impairment within the context of the client’s life
and experiences—for example, by examining current coping responses compared
with previ-ous experiences and assessing whether or not the client is engaging
in maladaptive behaviors such as drug and alcohol abuse as a means to deal with
the painful experience.
Related Topics