Chapter: Psychiatric Mental Health Nursing : Grief and Loss
Assessment - Grief and Loss: Application of the Nursing Process
Assessment
Effective assessment involves observing all dimensions of human
response: what the person is thinking (cognitive), how the person is feeling
(emotional), what the person’s values and beliefs are (spiritual), how the
person is acting (behavioral), and what is happening in the person’s body
(physiologic). Effective communication skills during assessment can lead the
client toward understanding his or her experience. Thus, assessment facilitates
the client’s grief process.
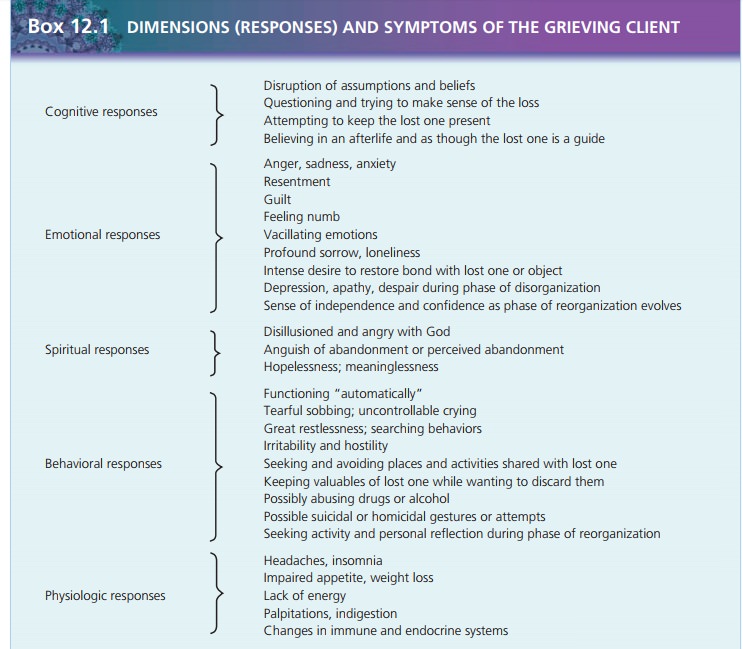
While observing for client responses in the dimensions of grieving,
the nurse explores three critical components in assessment:
·
Adequate perception regarding the loss
·
Adequate support while grieving for the loss
·
Adequate coping behaviors during the process.
Perception of the Loss
Assessment begins with exploration of the client’s percep-tion of
the loss. What does the loss mean to the client? For the woman who has
spontaneously lost her first unborn child and the woman who has elected to
abort a pregnancy, this question could have similar or different answers.
Nevertheless, the question is valuable for beginning to facilitate
the grief process.
Other questions that assess perception and encourage the client’s
movement through the grief process include the following:
·
What does the client think and feel about the loss?
·
How is the loss going to affect the client’s life?
·
What information does the nurse need to clarify or share with the
client?
Assessing the client’s “need to know” in plain and simple language
invites the client to verbalize perceptions that may need clarification. This
is especially true for the person who is anticipating a loss, such as one
facing a life-ending illness or the loss of a body part. The nurse uses
open-ended ques-tions and helps to clarify any misperceptions.

Consider the following. The doctor has just informed Ms. Morrison
that the lump on her breast is cancerous andThree major areas to explore
when assessing a grieving client that she can be scheduled for a mastectomy in 2
days. The nurse visits the client after rounds and finds her quietly watching
television.
Nurse: “How are you?” (offering presence; giv-ing a
broad opening)
Client: “Oh, I’m fine. Really, I am.”
Nurse: “The doctor was just here. Tell me, what is your understanding of what he said?” (using
open-ended questions for description of perception)
Client: “Well, I think he said that I will have to have surgery on my breast.”
Nurse: “How do you feel about that news?” (using
open-ended question for what it means to the client)
Exploring what the person believes about the grieving pro-cess is
another important assessment. Does the client have pre-conceived ideas about
when or how grieving should happen? The nurse can help the client realize that
grieving is very per-sonal and unique: each person grieves in his or her own
way.
Later in the shift, the nurse finds Ms. Morrison hitting her pillow
and crying. She has eaten little food and has refused visitors.
Nurse: “Ms. Morrison, I see that you are upset. Tell me, what is happening right now?” (shar-ing
observation; encouraging description)
Client: “Oh, I’m so disgusted with myself. I’m sorry you had to see me act this way. I shouldbe
able to handle this. Other people have lost their breasts to cancer, and they
are doing OK.”
Nurse: “You’re pretty upset with yourself, thinking you should feel differently.” (using
reflection)
Client: “Yes, exactly. Don’t you think so?”
Nurse: “You’ve had to deal with quite a shock today. Sounds to me like you are expecting quite a bit of yourself.
What do you think?” (using reflection; sharing perceptions; seeking validation)
Client: “I don’t know, maybe. How long is this going to go on? I’m a wreck emotionally.”
Nurse: “You are grieving, and there is no fixed timetable for what you are dealing with. Everyone has a unique time
and way of doing this work.” (informing; validating
experience)
Support
Purposeful assessment of support systems provides the grieving
client with an awareness of those who can meet his or her emotional and
spiritual needs for security and love. The nurse can help the client to
identify his or her support systems and reach out and accept what they can
offer.
Nurse: “Who in your life should or would really want to know what you’ve just heard from the doctor?”
(seeking information about situa-tional support)
Client: “Oh, I’m really alone. I’m not married and don’t have any relatives in town.”Nurse: “There’s no one who would care about this news?” (voicing doubt)
Client: “Oh, maybe a friend I talk with on the phone now and then.”
Coping Behaviors
The client’s behavior is likely to give the nurse the easiest and
most concrete information about coping skills. The nurse must be careful to
observe the client’s behavior throughout the grief process and never assume
that a cli-ent is at a particular phase. The nurse must use effective
communication skills to assess how the client’s behavior reflects coping as
well as emotions and thoughts.
The following day, the nurse has heard in report that Ms. Morrison
had a restless night. She enters Ms. Morrison’s room and sees her crying with a
full tray of food untouched.
Nurse: “I wonder if you are upset about your upcoming surgery.” (making an observation, assuming client was crying as an
expected behavior of loss and grief)
Client: “I’m not having surgery. You have me mistaken for someone else.” (using denial
to cope)
The nurse also must consider several other questions when assessing
the client’s coping. How has the person dealt with loss previously? How is the
person currently impaired? How does the current experience compare with
previous experiences? What does the client perceive as a problem? Is it related
to unrealistic ideas about what he or she shouldfeel or do?. The interaction of
the dimensions of human response is fluid and dynamic. What a person thinks
about during grieving affects his or her feelings, and those feelings influence
his or her behavior. The critical factors of percep-tion, support, and coping are
interrelated as well and pro-vide a framework for assessing and assisting the
client.
Related Topics