Chapter: Clinical Anesthesiology: Anesthetic Management: Neurophysiology & Anesthesia
Cerebral Metabolism
Cerebral Physiology
CEREBRAL METABOLISM
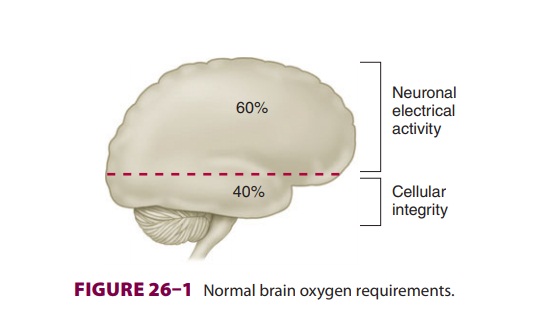
The brain normally consumes 20% of total
body oxygen. Most cerebral oxygen consumption (60%) is used to generate
adenosine triphosphate (ATP) to support neuronal electrical activity ( Figure26–1).
The cerebral metabolic rate (CMR) is usually expressed in terms of oxygen
consumption (CMRo2) and averages 3–3.8 mL/100 g/min (50
mL/min) in adults. CMRo2 is greatest in the gray matter of the
cerebral cortex and generally parallels cortical elec-trical activity. Because
of the relatively high oxygen consumption and the absence of significant oxygen
reserves, interruption of cerebral perfusion usually results in unconsciousness
within 10 sec, as oxygen tension rapidly drops below 30 mm Hg. If blood flow is
not reestablished within 3–8 min under most conditions, ATP stores are
depleted, and irreversible cellular injury begins to occur. The hippocampus and
cerebellum seem to be most sensitive to hypoxic injury.
Neuronal cells normally utilize glucose as their primary energy
source. Brain glucose con-sumption is approximately 5 mg/100 g/min, of which
more than 90% is metabolized aerobically. CMRo2 therefore normally parallels glucose con-sumption. This
relationship is not maintained dur-ing starvation, when ketone bodies
(acetoacetate and β-hydroxybutyrate) also become major energy substrates.
Although the brain can also take up and metabolize lactate, cerebral function
is nor-mally dependent on a continuous supply of glu-cose. Acute sustained
hypoglycemia is injurious to
the brain. Paradoxically, hyperglycemia can exac-erbate global
and focal hypoxic brain injury by accelerating cerebral acidosis and cellular
injury. Tight control of perioperative blood glucose con-centration has been
advocated in part because of adverse effects of hyperglycemia during ischemic
episodes; however, overzealous blood glucose con-trol can likewise produce
injury through iatrogenic hypoglycemia.
Related Topics