Chapter: Medical Physiology: Nervous Regulation of the Circulation, and Rapid Control of Arterial Pressure
Central Nervous System Ischemic Response
Central Nervous System Ischemic Response—Control of Arterial Pressure by the Brain’s Vasomotor Center in Response to Diminished Brain Blood Flow
Most nervous control of blood pressure is achieved by reflexes that originate in the baroreceptors, the chemoreceptors, and the low-pressure receptors, all of which are located in the peripheral circulation outside the brain. However, when blood flow to the vasomotor center in the lower brain stem becomes decreased severely enough to cause nutritional deficiency—that is, to cause cerebral ischemia—the vasoconstrictor and cardioaccelerator neurons in the vasomotor center respond directly to the ischemia and become strongly excited. When this occurs, the systemic arterial pressure often rises to a level as high as the heart can possibly pump. This effect is believed to be caused by failure of the slowly flowing blood to carry carbon dioxide away from the brain stem vasomotor center: at low levels of blood flow to the vasomotor center, the local con-centration of carbon dioxide increases greatly and has an extremely potent effect in stimulating the sym-pathetic vasomotor nervous control areas in the brain’s medulla.
It is possible that other factors, such as buildup of lactic acid and other acidic substances in the vasomotor center, also contribute to the marked stimulation and elevation in arterial pressure. This arterial pressure ele-vation in response to cerebral ischemia is known as the central nervous system ischemic response, or simply CNS ischemic response.
The magnitude of the ischemic effect on vasomotor activity is tremendous: it can elevate the mean arterial pressure for as long as 10 minutes sometimes to as high as 250 mm Hg. The degree of sympathetic vasoconstric-tion caused by intense cerebral ischemia is often so great that some of the peripheral vessels become totally or almost totally occluded.
The kidneys, for instance, often entirely cease their production of urine because of renal arteriolar constriction in response to the sympathetic discharge. Therefore, the CNS ischemic response is oneof the most powerful of all the activators of the sympa-thetic vasoconstrictor system.
Importance of the CNS Ischemic Response as a Regulator of Arte- rial Pressure. Despite the powerful nature of the CNSischemic response, it does not become significant until the arterial pressure falls far below normal, down to 60 mm Hg and below, reaching its greatest degree of stimulation at a pressure of 15 to 20 mm Hg. Therefore, it is not one of the normal mechanisms for regulating arterial pressure. Instead, it operates principally as an emergency pressure control system that acts rapidly and very powerfully to prevent further decrease in arterial pressure whenever blood flow to the brain decreases dan-gerously close to the lethal level. It is sometimes calledthe “last ditch stand” pressure control mechanism.
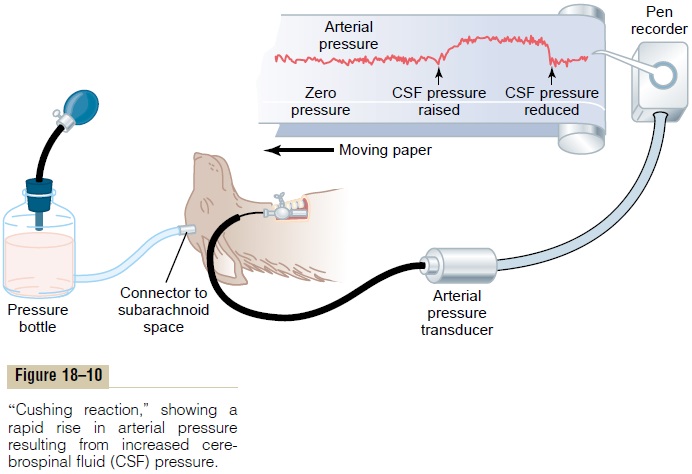
Cushing Reaction. The so-calledCushing reactionis aspecial type of CNS ischemic response that results from increased pressure of the cerebrospinal fluid around the brain in the cranial vault. For instance, when the cerebrospinal fluid pressure rises to equal the arterial pressure, it compresses the whole brain as well as the arteries in the brain and cuts off the blood supply to the brain.This initiates a CNS ischemic response that causes the arterial pressure to rise. When the arterial pressure has risen to a level higher than the cerebrospinal fluid pressure, blood will flow once again into the vessels of the brain to relieve the brain ischemia. Ordinarily, the blood pressure comes to a new equilibrium level slightly higher than the cerebrospinal fluid pressure, thus allow-ing blood to begin again to flow through the brain. A typical Cushing reaction is shown in Figure 18–10, caused in this instance by pumping fluid under pressure into the cranial vault around the brain. The Cushing reaction helps protect the vital centers of the brain from loss of nutrition if ever the cerebrospinal fluid pressure rises high enough to compress the cerebral arteries.
Related Topics