Chapter: Modern Pharmacology with Clinical Applications: Introduction to Central Nervous System Pharmacology
Blood-Brain Barrier
BLOOD-BRAIN
BARRIER
Not all substances in the
bloodstream can readily gain entry into the brain. This apparent barrier to
drugs and other chemicals is relative rather than absolute, and in fact there
are several barriers to substances entering the brain from the systemic circulation.
The term blood-brain barrier is
usually applied to the lack of passage of
certain drugs or other exogenously administered chem-icals into the brain.
One important property that
determines entry to the brain from the systemic circulation is molecular
weight. Compounds with molecular weights of about 60,000 and above tend to
remain within the circulatory system. Furthermore, the portion of an
administered drug that is bound to plasma proteins is unavailable for
distribution to the brain (as well as to other tissues and organs), in part
because of the high molecular weight of the plasma protein–drug complex.
There are two physicochemical
factors particularly important in allowing a drug to enter the CNS. First, for
compounds that are mainly un-ionized at plasma pH (pKa 7.4 or
higher), the drug’s solubility in lipids
is an important determinant. A
lipid-soluble agent can more easily
penetrate lipid membranes, such as those found in the CNS. The proportion of
drug that is un-ionized is another important determinant. These two properties
cannot be completely separated, since un-ionized drugs are generally more lipid
soluble than ionized ones.
Location of the Blood-Brain Barrier
The capillaries of the brain
are the most likely location of the blood-brain barrier. Brain capillaries
differ in several important respects from capillaries in other body locations
(Fig. 24.5). For example, the endothelial cells of brain capillaries are so
closely joined to each other that passage of substances cannot readily occur through
the intercellular clefts between adjacent cells; furthermore, brain capillaries
do not contain fenestrae (pores). Fenestrae are prominent in many capillaries,
especially those in renal glomeruli and in the chorioid plexus. The ability of
a drug to leave a capillary by dif-fusion appears to be directly related to the
number of capillary pores. Compared with capillaries at other sites, brain
capillaries also appear to possess very few pinocytotic vesicles, which are
believed to play a role in the transport of large molecules through capillary
walls.
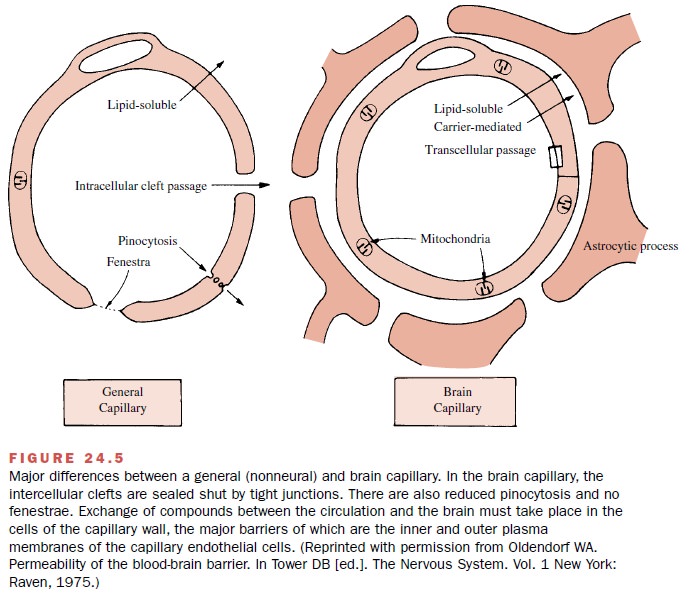
Brain capillaries contain many more mitochondria than do other capillaries, and it is probable that the mi-tochondria supply energy for active transport of water-soluble nutrient substances into the brain. A large number of lipid-insoluble endogenous substances are known to be transported into the brain. These substances include glucose, amino acids, simple car-boxylic acids, and purines.
Significance of the Blood-Brain Barrier
It is likely that the
blood-brain barrier serves primarily to preserve the internal environment of
the brain and prevent sudden increases in concentration of a variety of
water-soluble ionized substances, including many cir-culating
neurotransmitters, such as norepinephrine, epi-nephrine, ACh, serotonin, and
dopamine. The concen-tration in the brain of these bioactive substances appears
to be carefully regulated. On the other hand, the biochemical precursors of
these transmitters can pass relatively easily, although usually by active
trans-port, from the blood to the brain, and this ensures an adequate supply of
locally synthesized transmitters. By and large, the precursors are inactive
biologically or have only minimal biological activity. The amino acid
transmitters GABA, glycine, glutamic acid, and aspartic acid are actively taken
up by the brain capillaries, but ordinarily the transport system for these
amino acids is close to saturation. Therefore, a sudden increase in blood
concentration of these substances would have lit-tle effect on brain levels.
Peptide transmitters will not readily penetrate the brain from the circulation,
and they are synthesized in the brain.
The blood-brain barrier is
not found in all parts of the brain. Certain small areas, including the area postrema
beneath the floor of the fourth ventricle, an area in the preoptic recess,
and portions of the floor of the third ventricle surrounding the stalk of the
pituitary, appear to be devoid of this barrier.
The ability of the
blood-brain barrier to exclude en-try of a number of drugs into the brain has
several ther-apeutic implications. Many drugs, most notably certain
antibiotics, are relatively excluded from the brain. In the treatment of
infectious diseases of the CNS, the physi-cian must, in addition to
establishing the organism’s drug sensitivity, either select an agent that can
get to the site of the infection or use a route (intrathecal) that by-passes
the barrier. In the human fetus and newborn, the barrier is not as well
developed as it is in later life. This fact also must be taken into
consideration when one is prescribing drugs during pregnancy and for neonates .
Related Topics