Chapter: Clinical Dermatology: Eczema and dermatitis
Eczema and dermatitis: Investigations
Investigations
Each
pattern of eczema needs a different line of inquiry.
Exogenous eczema
Here
the main decision is whether or not to under-take patch testing to confirm allergic contact dermatitis and to
identify the allergens responsible for it. In patch testing, standardized
non-irritating con-centrations of common allergens are applied to the normal
skin of the back. If the patient is allergic to the allergen, eczema will
develop at the site of contact after 48–96 h. Patch testing with irritants is
of no value in any type of eczema, but testing with suitably diluted allergens
is essential in suspected allergic con-tact eczema. The technique is not easy.
Its problems include separating irritant from allergic patch test reactions,
and picking the right allergens to test. If legal issues depend on the results,
testing should be carried out by a dermatologist who will have the stan-dard
equipment and a suitable selection of properly standardized allergens (see Fig.
3.7). Patch testing can be used to confirm a suspected allergy or, by the use
of a battery of common sensitizers, to discover unsus-pected allergies, which
then have to be assessed in the light of the history and the clinical picture.
A visit to the home or workplace may help with this.
Photopatch
testing is more specialized and facilities are only available in a few centres.
A chemical is applied to the skin for 24 h and then the site is irradiated with
a suberythema dose of ultraviolet irradiation; the patches are inspected for an
eczematous reaction 48 h later.
Other types of eczema
The only indication for patch
testing here is when an added contact allergic element is suspected. This is
most common in gravitational eczema; neomycin, framycetin, lanolin or
preservative allergy can per-petuate the condition and even trigger
dissemination. Ironically rubber gloves, so often used to protect eczematous
hands, can themselves sensitize..
Patients with atopic dermatitis
often have multiple type I reactions to foods, danders, pollens, dusts and
moulds. Some find the measurement of serum total immunoglobulin E (IgE), and of
IgE antibodies specific to certain antigens, not only useful in diagnosing the
atopic state, but also helpful when advising on the role of dietary and
environmental allergens in causing or perpetuating atopic dermatitis,
particularly in chil-dren. Total and specific IgE antibodies are measured by a
radioallergosorbent test (RAST). Prick and RAST testing give similar results
but many now prefer the more expensive RAST test as it carries no risk of anaphyl-axis,
is easier to perform and is less time consuming.
If the eczema is worsening despite
treatment, or if there is much crusting, heavy bacterial colonization may be
present. Opinions vary about the value of cultures for
bacteria and candida, but antibiotic treatment may be helpful. Scrapings for
microscopical examination and culture
for fungus will rule out tinea if there is clinical doubtaas in some cases of
discoid eczema.
Finally,
malabsorption should be considered in otherwise unexplained widespread
pigmented atypical patterns of endogenous eczema.
Acute weeping eczema
This
does best with rest and liquid applications. Non-steroidal preparations are
helpful and the techniques used will vary with the facilities available and the
site of the lesions. In general practice a simple and con-venient way of
dealing with weeping eczema of the hands or feet is to use thrice daily 10-min
soaks in a cool 0.65% aluminium acetate solution asaline or even tap water will
do almost as wellaeach soaking being followed by a smear of a corticosteroid
cream or lotion and the application of a non-stick dressing or cotton gloves.
One reason for dropping the dilute potassium permanganate solution that was
once so popular is because it stains the skin and nails brown.
Wider
areas on the trunk respond well to cortico-steroid creams and lotions. However,
traditional rem-edies such as exposure and frequent applications of calamine
lotion, and the use of half-strength magenta paint for the flexures are also
effective.
An
experienced doctor or nurse can teach patients how to use wet dressings, and
supervise this. The aluminium acetate solution, saline or water, can be applied
on cotton gauze, under a polythene covering, and changed twice daily. Details
of wet wrap tech-niques are given below. Rest at home will help too.
Wet wrap dressings
This
is a labour-intensive, but highly effective tech-nique, of value in the
treatment of troublesome atopic eczema in children. After a bath, a
corticosteroid is applied to the skin and then covered with two layers of
tubular dressingathe inner layer already soaked in warm water, the outer layer
being applied dry. Cotton pyjamas or a T-shirt can be used to cover these, and
the dressings can then be left in place for several hours. The corticosteroid
may be one that is rapidly metabolized after systemic absorption such as a
beclomethasone (beclometasone) diproprionate oint-ment diluted to 0.025%
(available only in the UK). Alternatives include 1 or 2.5% hydrocortisone cream
for children and 0.025 or 0.1 % triamcinolone cream for adults. The bandages
can be washed and reused. The evaporation of fluid from the bandages cools the
skin and provides rapid relief of itching. With improvement, the frequency of
the dressings can be cut down and a moisturiser can be substituted for the
corticosteroid. Parents can be taught the technique by a trained nurse, who
must follow up treatment closely. Parents easily learn how to modify the
tech-nique to suit the needs of their own child. Side-effects seem to be minimal.
Subacute eczema
Steroid
lotions or creams are the mainstay of treat-ment; their strength is determined
by the severity of the attack. Vioform, bacitracin, fusidic acid, mupirocin or
neomycin can be incor-porated into the application if an infective element is
present, but watch out for sensitization to neomycin, especially when treating
gravitational eczema.
Chronic eczema
This
responds best to steroids in an ointment base, but is also often helped by
non-steroid applications such as ichthammol and zinc cream or paste.
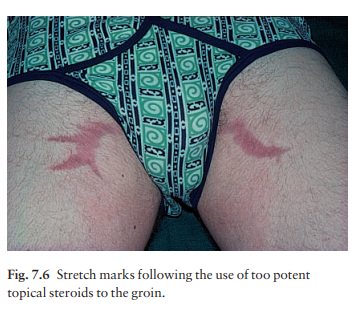
The
strength of the steroid is important (Fig. 7.6). Nothing stronger than 0.5 or
1% hydrocortisone ointment should be used on the face or in infancy. Even in
adults one should be reluctant to prescribe more than 200 g/week of a mildly
potent steroid, 50 g/week of a moderately potent or 30 g/week of a potent one
for long periods. Very potent topical steroids should not be used long-term.
Bacterial
superinfection may need systemic antibi-otics but can often be controlled by
the incorporation of antibiotics, e.g. fusidic acid, mupirocin, neomycin or
chlortetracycline, or antiseptics, e.g. Vioform, into the steroid formulation.
Many proprietary mixtures of this type are available in the UK. Chronic
localized hyperkeratotic eczema of the palms or soles can be helped by
salicylic acid (1–6% in emulsifying oint-ment) or stabilized urea preparations.
Systemic treatment
Short
courses of systemic steroids may occasionally be justified in extremely acute
and severe eczema, par-ticularly when the cause is known and already
elim-inated (e.g. allergic contact dermatitis from a plant such as poison ivy).
However, prolonged systemic steroid treatment should be avoided in chronic cases,
particularly in atopic eczema. Hydroxyzine, doxepin, trimeprazine and other
antihistamines may help at night.
Systemic antibiotics may be needed in widespread bacterial superinfection.
How-ever, Staphylococcus
aureus routinely colonizes all weeping eczemas, and most dry ones
as well. Simply isolating it does not automatically prompt a prescrip-tion for
an antibiotic, although if the density of organ-isms is high, usually manifest
as extensive crusting, then systemic antibiotics can help.
Related Topics