Chapter: Clinical Cases in Anesthesia : Local Anesthetics
What is the treatment for local anesthetic allergic reactions?
What is the treatment for local anesthetic allergic reactions?
Mast cell degranulation liberates histamine,
leukotrienes, prostaglandins, platelet-activating factor, and kinins that
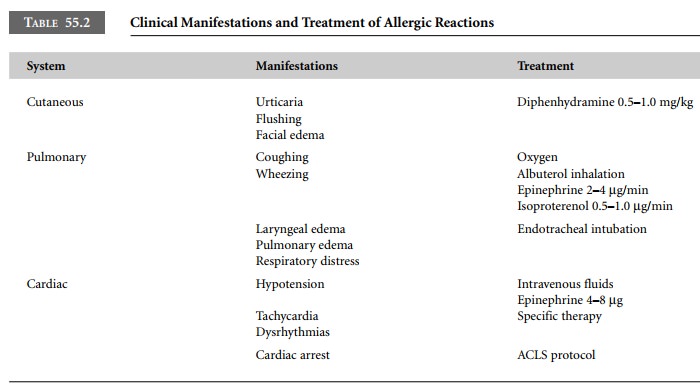
produce adverse systemic effects. Table 55.2 summarizes the clinical
manifestations of allergic reactions and notes specific therapy for potentially
lethal reactions. Management of allergic reactions requires immediate
identification of the offending agent and cessation of its administration.
Cutaneous manifestations such as itching, burning, urticaria, or flushing can
be treated with diphenhydramine, 0.5–1.0 mg/kg intravenously. Respiratory
signs, including coughing and wheezing, are indications for supplemental oxygen
and bronchodilators. The inhaled β-2-selective agents, such as albuterol, are the
preferred bronchodilators. Severe cases may require epinephrine or
isoproterenol. Laryngeal edema, pulmonary edema, and other signs of respiratory
distress require endotracheal intubation and positive pressure ventilation.
Mild hypotension is treated with intravenous fluids. Profound hypotension
requires therapy with fluids and epinephrine. Epinephrine 0.5–1.0 mg is
administered for cardiovascular collapse. Hydrocortisone or methylprednisolone
helps prevent future reactions but probably does little for the acute
situation. When endotracheal intubation is performed for airway edema,
extubation should be preceded by a deflation test. To perform this test,
deflate the endotracheal tube’s cuff, administer positive-pressure ventilation,
and listen for gas escaping between the tube and the airway. The absence of gas
escaping from the outside the endotracheal tube suggests persistent airway
edema.
Related Topics