Chapter: Forensic Medicine: Head injuries
Types of head injuries
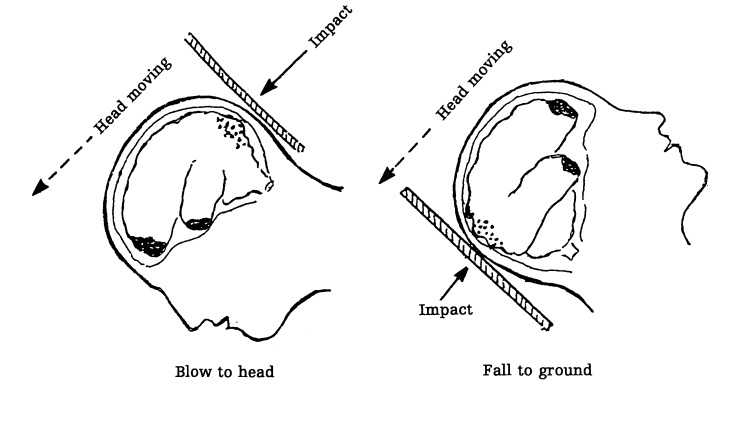
Types of head injuries
Skin injuries
All the different types of blunt and sharp
injuries already discussed in study unit 5 can involve the scalp. A blow to the
head with a blunt object can split the skin because the scalp is trapped
between the blunt object and the underlying skull. These wounds can easily be
confused with an incised wound. However, careful examination will reveal tissue
bridges and a fine margin of abrasion.
The appearance of entrance gunshot wounds is
discussed elsewhere.
If someone wears a protective cap or even just
has a thick head of hair, the skin, but not necessarily the underlying brain,
may be protected against injury. Absence of skin injuries or fractures does
therefore not exclude brain injury.
Fractures
Skull fractures can be classified as follows:
·
Simple fractures: the overlying scalp is intact
·
Open or compound fractures: the fracture and underlying tissue
communicate through a skin defect with the external environment. These
fractures can easily become infected.
·
Comminuted fracture: the bone is broken into many separate pieces.
Skull fractures have certain unique features:
·
Linear fractures are usually not associated with movement of the
adjacent bone plates.
·
Depressed fractures differ from the above. They are often more
localised, and result from impact against a smaller object. Knobkieries often
cause a depressed fracture.
·
Contre-coup fractures are found diagonally opposite the point of impact.
If someone falls on the back of his head, fractures may occur on the frontal
aspect of the skull, especially of the thin and delicate bone overlying the
orbital cavities (orbital plates).
·
A ring fracture is present around the hole at the base of the skull (the
foramen magnum). These fractures occur when someone lands forcefully on his
feet and the weight of the head propels the skull downward on the spine.
·
Hinge fractures are severe and may display extensive fractures involving
the base of the skull. After removal of the cranial vault, the anterior and
posterior aspects of the skull base can be moved relative to one another.
It must be remembered that the skull of an
infant toddler may deform substantially without fracturing. Brain injuries
could therefore occur without any fractures. However, the sutures between the
bony plates may be damaged (diastasis).
Brain contusions and lacerations
Wherever the brain is brought forcefully into
contact with the overlying bone or even the free edges of the dural folds (eg
the inferior aspect of the falxcerebri, the dural fold dividing the brain in
two halves), the tissue can become contused. If the force is sufficient, the
brain surface may even tear (lacerate). As these lacerations are always
surrounded by contusions, we often refer to them as contusions/lacerations.
As can be expected, these injuries will be
located at the points of contact with the overlying bone. Contusions are
therefore seen at the crest of the convolutions (gyri), and not in the depth of
the grooves (sulci). Those parts of the brain in contact with rough and uneven
bony elements are particularly prone to injury. This especially applies to the
base of frontal lobe. If the contact between the brain and bone is severe, the
brain lobe hitting the bone may burst. This usually involves the frontal and
temporal lobes.
In the past much emphasis has been placed on the
concepts coup and contre-coup (fig 7.14). The former is said to occur at the
point of impact and the latter diagonally across from it. It was also said that
the contre-coup injury tends to be more severe. This is not always true.
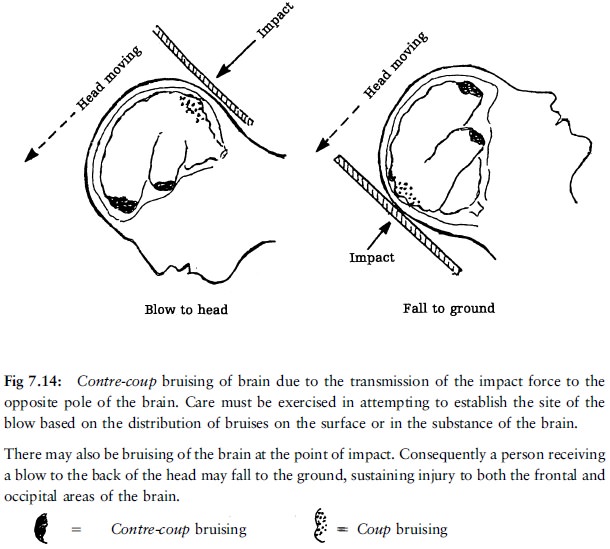
If someone is hit on the back of the head
(occiput), movement of the under-surface of the frontal lobe over the rough
bony surface of the anterior cranial fossa will cause a contre-coup injury of
the base of the frontal lobe. However, the occipital lobe moving over the
relatively smooth surface of the tentorium cerebelli will suffer less injury.
In this case the contre-coup injury will be more severe than the coup injury.
If the blow is over the frontal aspect, the frontal lobe will still suffer more injury, for the same reasons. In this case the coup injury will be more severe than the contre-coup injury.
Diffuse axonal injury
Diffuse axonal injury (DAI) is a condition which
occurs at the moment of impact. Due to acceleration and deceleration forces in
the brain tissue (often accompanied by rotational and angulation forces), a
diffuse disruption of axons (nerve fibres) occurs due to shearing and traction.
Clinical presentation
DAI presents immediately at the moment of
impact. Clinically it can present with a spectrum of different grades, varying
from mild, which presents clinically as concussion, to severe. In the latter
case the patient is immediately unconscious with no lucid interval. In these
cases the coma usually lasts more than 6 hours.
Pathological changes
Macroscopically (with the naked eye) or with
certain radiological procedures (a CT scan or magnetic resonance (MR))
petechial haemorrhages are present in the corpus callosum (the fibres joining
the two halves of the brain) and in the dorso-lateral aspects of the pons (a
part of the brain stem). A tear of the septum pellucidum and fornixes may also
be present. This results in haemorrhage in the two lateral ventricals of the
brain (intraventricular haemorrhage). The petechial haemorrhages are the result
of rupture of the small blood vessels running alongside the axons (nerve
fibres) in the brain. As these vessels are also damaged by the shearing forces
experienced during DAI, it is an indirect indicator of axonal injury, as the
latter is not visible with the naked eye. In the corpus callosum and
dorso-lateral aspects of the pons, the nerve fibres are more susceptible to
damage as they are longer and are therefore more prone to damage by shearing
forces.
Microscopically a diffuse disruption of the
axons can be seen. Depending on the survival period certain changes will be
evident, of which the first sign will be retraction balls due to axonal
swelling. Damage to axons (and neurons, ie brain cells) is irreversible, and
with time these damaged neurons disappear.
Associations
The method of injury (whether the brain
decelerates or accelerates inside the cranial cavity) can cause certain
associations with other, but separate, brain injuries. Gliding contusions occur
almost in the midline of the brain (parasagittal region) where the surface of
the brain is fixed by means of the arachnoid villi to the overlying dura mater.
When movement of the brain occurs relative to these points of fixation, small
haemorrhages occur at the interface between the white and grey matter as the
latter is fixed by means of the arachnoid villi, and cannot move with the white
matter.
There are sometimes also haematomas (localised
haemorrhages) in die deep intra-cerebral matter, in the region of the basal
ganglia. They are also known as intermediary coup lesions.
It is important to note that DAI has no or
minimal association with other injuries which are normally the result of more
localised impact, such as fractures of the skull, contusions or lacerations of
the brain matter, and intracranial haemorrhages (other than those mentioned
above). In addition DAI is seldom associated with an increase in the
intracranial pressure.
To summarise: DAI is a common injury due to
acceleration and deceleration of the brain, often concomitant with rotational
and angulation forces. If severe enough, it can cause a vegetative state, where
a patient is unconscious, but able to maintain his or her own vital functions
(respiration and cardiovascular status)
Traumatic intracranial haemorrhage
1 General
·
This is often the result of non-missile injury, such as a blow to the
head.
·
These haemorrhages are the most common cause of deterioration in a
patient after a lucid (``awake'') period.
·
More than 35 ml is a sufficient volume to act as a space-occupying
lesion.
·
These haemorrhages are often associated with fracture(s).
·
There is often more than one type of haemorrhage.
·
Although of primary origin, it often presents as a complication, in
other words as a secondary phenomenon.
2 Classification
·
extradural haemorrhage
·
subdural haemorrhage
·
subarachnoidal haemorrhage
·
intracerebral haemorrhage
·
intraventricular haemorrhage
This classification is limited to traumatic
haemorrhages, and does not include spontaneous causes of haemorrhages, such as
hypertensive haemorrhages or haemorrhages due to rupture of a berry aneurysm
(defect in the blood-vessel wall).
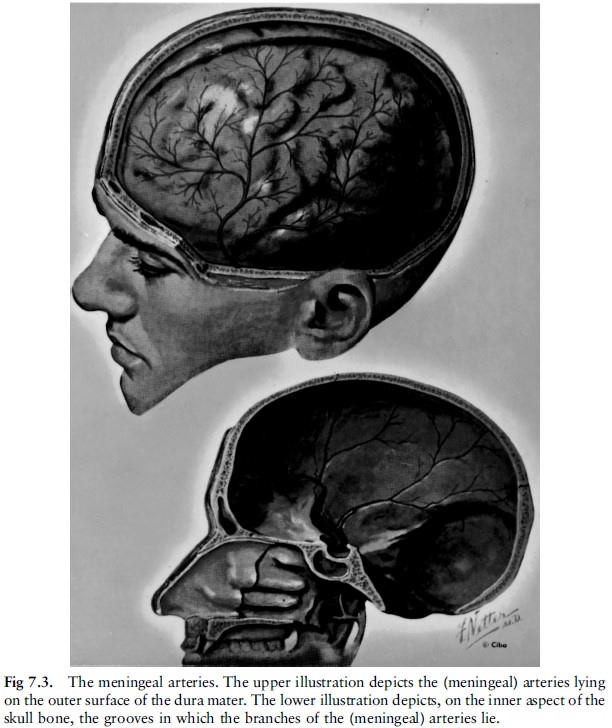
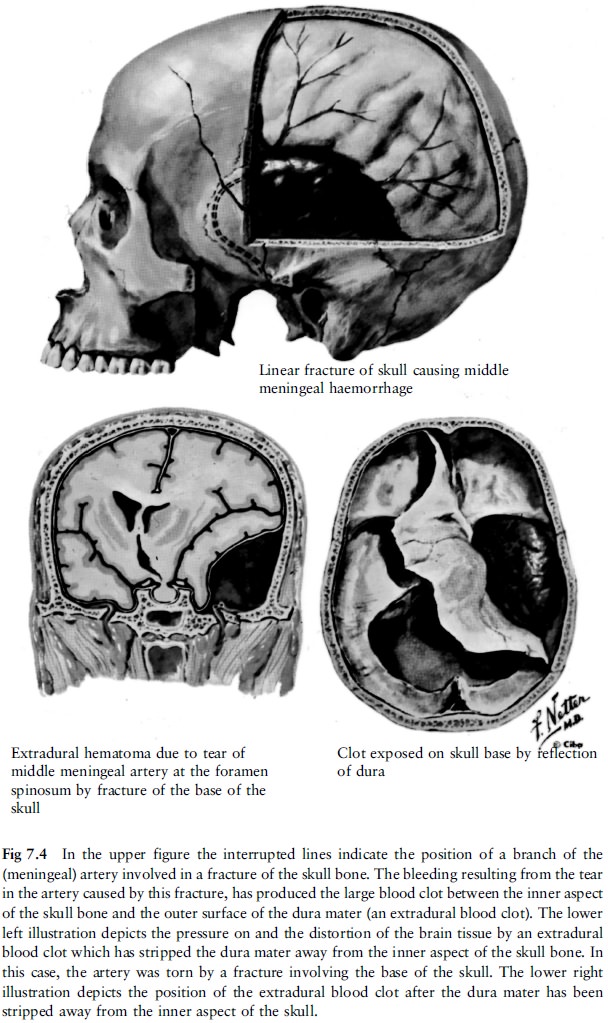
a. Extra(epi)dural haemorrhage (fig 7.3 and fig 7.4)
Extradural haemorrhages are also known as
epidural haemorrhages. These haemorrhages occur between the dura and the
overlying skull. The dura is a relatively thick membrane which lines the inner
surface of the skull. A number of arteries are present in the dura. They are
often partially embedded in the overlying skull bone. One of these arteries is
the middle meningeal artery which runs on the side of the head in the
temporo-parietal region. This artery can be damaged with subsequent haemorhage
if a fracture occurs in that region. Smaller fracture-associated extradural
haemorrhages may also occur elsewhere.
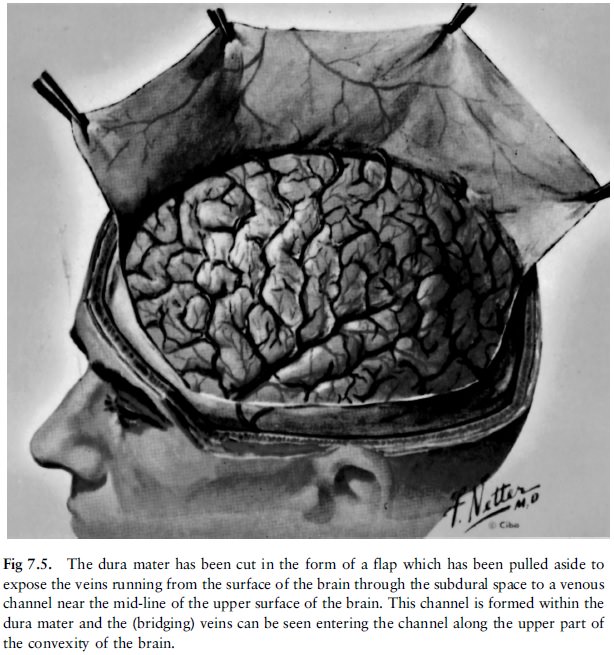
b. Subdural haemorrhage (fig 7.5, fig 7.6 and fig 7.7)
A number of small veins run between the surface
of the brain (arachnoid mater or leptomeninges) and the dura. With sudden
acceleration or deceleration these small veins may rupture, with subsequent
haemorrhage. A relatively small brain compared with the cranial cavity will
predispose to such movement, and therefore injury with subsequent haermorrhage.
This condition is therefore often found in alcoholics with brain atrophy. In
addition, babies have relatively small brains compared with the cranial cavity.
The muscles of a baby's neck are also not well
developed, and if you shake a baby, as is often seen in cases of child abuse,
excessive movement of the brain can occur in the cranial cavity, with subsequent
damage to these vessels.
Subdural haemorrhages can also occur in cases of
burst lobe, where severe trauma to part of the brain will cause haemorrhage in
the brain tissue (in a brain lobe), as well as outside (in the subdural space).
This usually communicates via contusion/laceration. Subdural haemorrhage
typically present after a period of time, as they are venous in origin and
therefore take time to develop (longer compared with an extradural
haemorrhage). These patients are often called ``walk-talk-and-die'' patients,
as the patient will present to the trauma unit with a history of even
relatively trivial trauma, and after examination the doctor will send the
patient home. The next day or thereafter the patient presents in a comatose
state and dies.
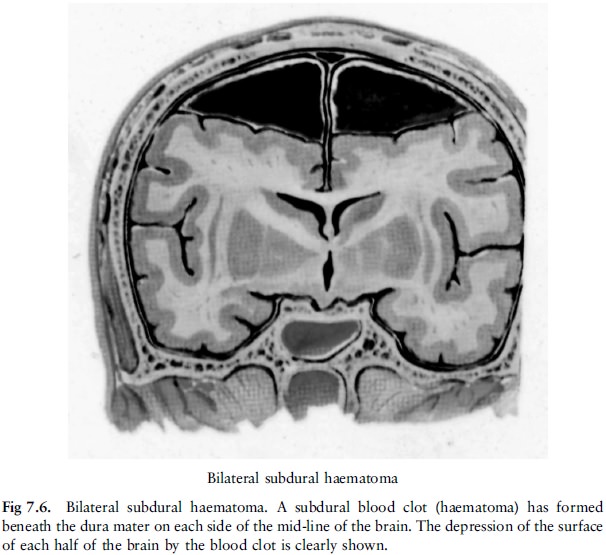
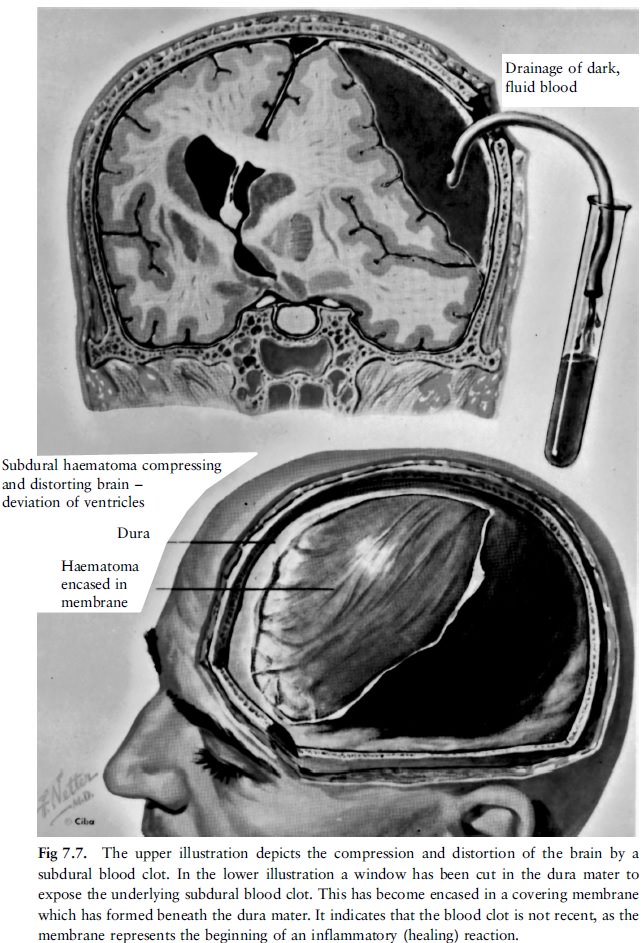
Subdural haemorrhages can be divided into acute,
subacute and chronic haemorrhages. An acute haemorrhage will consist of clotted
blood, while a chronic haemorrhage will consist of liquid blood. In addition
there will often be signs of membrane formation encapsulating these
haemorrhages. Subdural haemorrhages, like any other space-occupying lesion,
will cause herniation of brain tissue if of sufficient volume.
c. Subarachnoidal haemorrhage
These haemorrhages occur below the leptomeninges
(arachnoid mater) in the subarachnoidal space, are quite common in head
injuries, and can be diffuse or focal. Subarachnoidal haemorrhages are also
seen when there is rupture of a berry aneurysm. Berry aneurysms occur because
of weakening of the vasculature of the brain. At these points the wall of the
blood vessel forms small balloons (aneurysms) which can rupture, with
subsequent often fatal haemorrhage. It is important to remember that this is
not a trauma-related haemorrhage.
d. Intracerebral haemorrhage
Intracerebral haemorrhages may either be present
in a lobe of the brain (lobar haematoma), or in the basal ganglia region, as
seen in cases of diffuse axonal injury.
e. Intraventricular haemorrhage
Intraventricular haemorrhages occur in the
lateral ventricles of the brain.
They are often the result of rupture of the
septum pellucidum or fornix.
These haemorrhages therefore occur in cases of
diffuse axonal injury.
Herniations
The volume of the cranial cavity is fixed. The
intracranial contents consist of 70% brain tissue, 15% blood and 15%
cerebrospinal fluid. If there is an increase in the volume occupied by the
brain or blood, the cerebrospinal fluid will decrease in volume to accommodate
this. However, when this volume is exceeded, the intracranial pressure will
rise. Increased intracranial pressure is almost always associated with
herniations (figure 7.15).
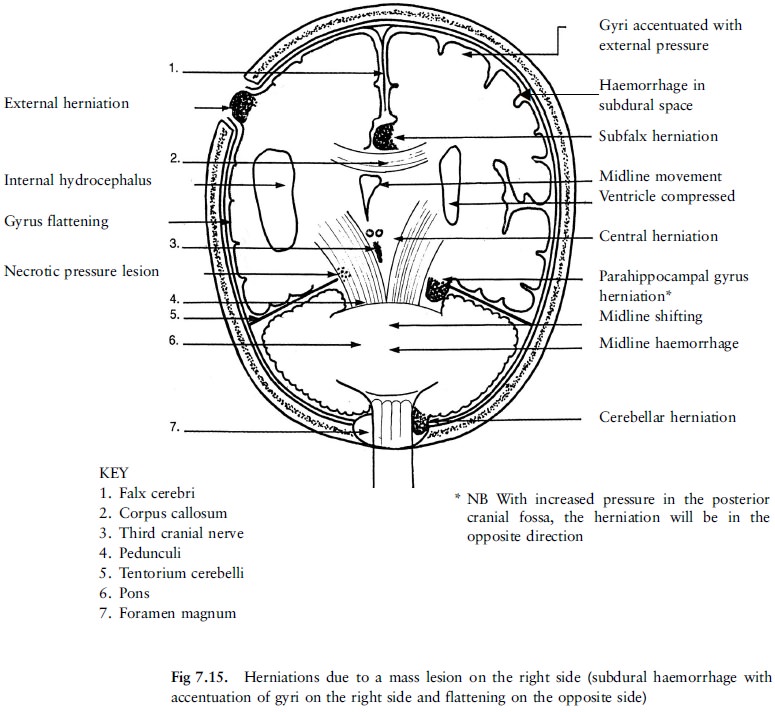
The intracranial cavity is divided by dural
folds into three compartments. The tentorium cerebelli is the membrane fold
separating the cerebrum (brain) and cerebellum (hind brain). The space below it
is also called the infratentorial space and is found in the posterior cranial
fossa. The supratentorial space above the tentorium is divided by the
falxcerebri into two halves/ hemispheres.
Herniations are brain tissue which is forced
from one part of the intracranial cavity to another. As the brain tissue is
pushed over the free edges of the dural folds it can become contused and
damaged. In addition, the general direction of herniation is downwards towards
the foramen magnum, and with increasing pressure in the posterior cranial
fossa, the vital centres controlling respiration and the vasomotor systems will
become depressed, ultimately leading to death.
The following herniations may occur see (fig
7.15). As herniation is a dynamic process, more than one is often present, as
it creates a domino effect.
·
Subfalx herniation. The medial aspect of the one cerebral hemisphere
is forced below (sub) the falxcerebri (falx) to the opposite side. As this is
located above the corpus callosum it is also called a supra-callosal
herniation. (The falxcerebri is the fold between the cerebral hemispheres.
Herniation means the abnormal protrusion of a body structure through a defect
in a membrane, muscle or bone.)
·
Central herniation. The central aspect of the brain is forced
downwards onto the brain stem. This may cause secondary haemorrhages in the
brain stem, with damage to the vital centres, and death.
·
Parahippocampalgyrus herniation. The medial aspect of the temporal lobe (the
parahippocampalgyrus) is forced over the free edge of the opening in the
tentorium cerebelli (incisura) into the posterior cranial fossa. Traction and
compression may cause damage to nerves and blood vessels - the latter with infarction of brain tissue.
·
Tonsillar herniation. This is also known as coning. The cerebellum
(cerebellar tonsils) is forced downwards through the foramen magnum. As this is
a risk in cases of raised intracranial pressure, it is contra-indicated to
perform a lumbar puncture in patients expected to suffer from raised
intracranial pressure, as it lowers the pressure in the spinal colum.
All these are internal herniations. External
herniations occur when brain tissue herniate through a defect in the skull. It
appears as a mushroom of brain tissue protruding from the head.
Brain swelling
Brain swelling is an increase in the size of the
brain or parts thereof. It can be due to an increase in the blood volume, ie
perfusion swelling; the blood (and therefore fluid) is still intravascular (in
the vessels). This condition occurs in two situations: in young children after
brain trauma, and in the brain on the same side as a subdural haemorrhage. It
is the result of collapse of the system which controls blood-flow in the brain.
If the fluid accumulates outside the vessels
(extravascular) it is also called cerebral oedema. There are different types of
oedema.
Tumors and brain abscesses are often surrounded
by new, immature blood vessels. The walls leak, and fluid accumulates in the
surrounding tissue. This surrounding rim of oedema is called vasogenic oedema,
and increases the size of the tumor or abscess significantly.
The other important type of cerebral oedema is
cytotoxic oedema. This is caused by damage to cells, which then swell due to
loss of the normal energy-dependant fluid control of the cells. It is often
seen in an infarction, where loss of oxygen supply causes the energy-dependant
processes to stop. Sodium will then accumulate in the cell, it will attract
water due to the osmotic pressure, with concomitant swelling.
As a matter of interest it must be noted that
both types of oedema are often seen in an infarction. The central aspect shows
cytotoxic oedema, and the more peripheral aspect, where the blood vessel walls
have been damaged by the hypoxia, exhibits vasogenic oedema.
There are also other types of oedema, for
example in cases of hypertension (hydrostatic oedema) or due to rehydration
after a period of diabetic coma or hypertonic dehydration (osmotic oedema).
These, however, fall beyond the scope of this study guide.