Chapter: Essential Anesthesia From Science to Practice : Clinical management : Regional anesthesia
Peripheral nerve blocks
Peripheral nerve blocks
With
neuraxial anesthesia, it is difficult to block only the area of interest.
Almost by definition, surgical anesthesia at the desired level includes
everything “south” as well. Peripheral nerve blocks provide an alternative,
interrupting nerve impulses at specific points in their course, rather than the
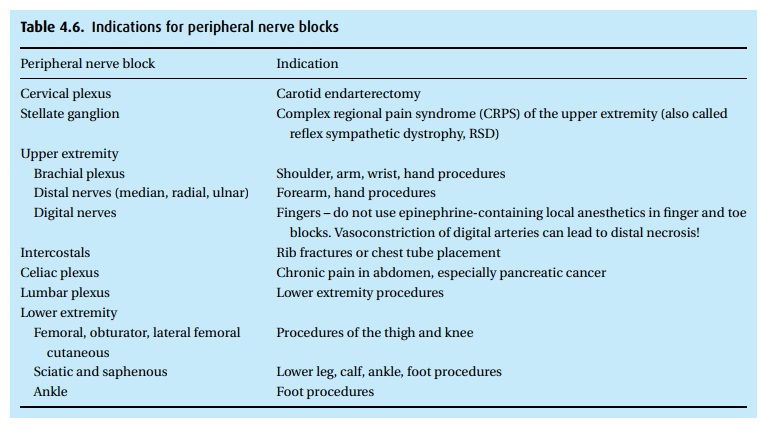
entire spinal cord. Table 4.6 lists some of
the blocks we perform.
While
local anesthetics can diffuse a small distance, depositing the drug in close
proximity to the desired nerve increases the likelihood of a successful block.
Therefore, knowledge of anatomy is paramount. Sometimes, anatomic landmarks
suffice;
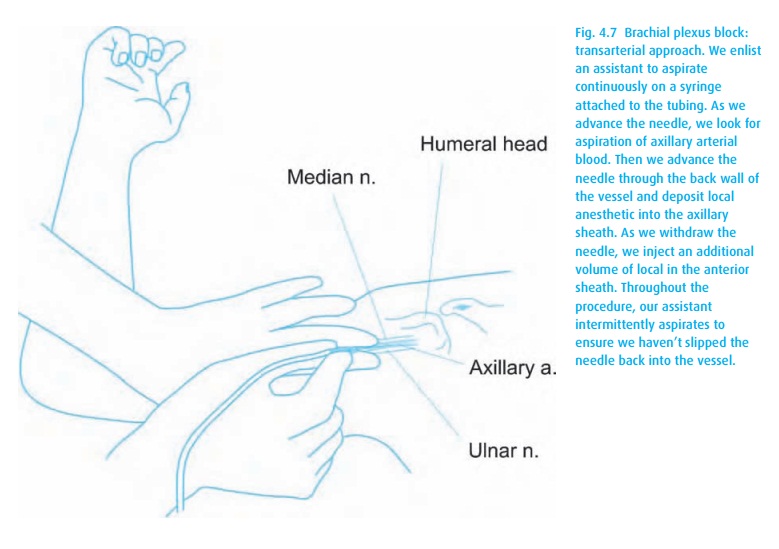
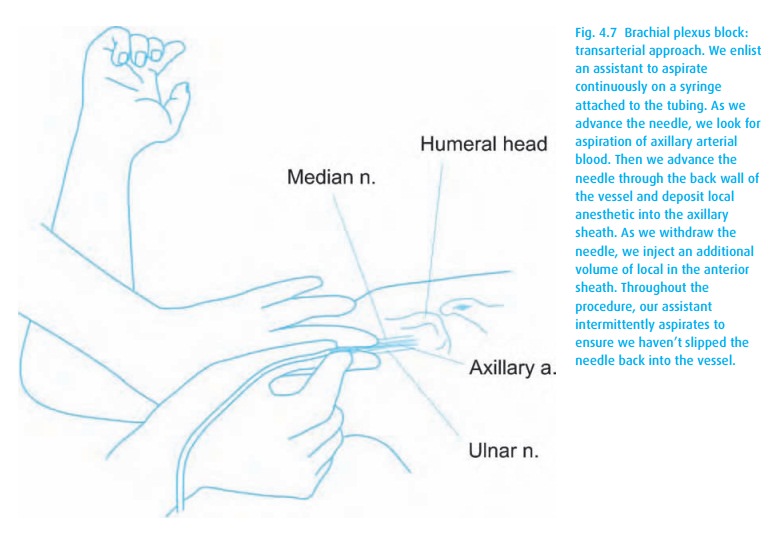
for example, we can deposit local anesthetic in the axillary sheath by
traversing its artery (Fig. 4.7). For most
other blocks, in order to ensure the needle tip lies within millimeters of the
intended nerve (and not in the
nerve), we use one of two common techniques:
·
Paresthesia technique, in which placement of a needle in close
proximity to a nerve causes a “pins and needles” sensation in the nerve’s
peripheral distribu-tion. Depending on the area of the intended block, specific
paresthesias can be sought with manipulation of the needle. This technique can
be uncom-fortable for the patient, yet requires the patient to be sufficiently
awake to respond. We need to watch the patient while gauging the pressure we
apply to the plunger of the syringe. The patient will let us know if he feels
an “electric shock” or pain – signs we associate with the intraneural placement
of the needle, at which point we do not proceed to inject drug under high
pressure, which would compress the nerve in its sheath, causing nerve ischemia
and injury.
·
Nerve stimulator technique, in which we apply a small electrical
current to an insulated needle, causing motor stimulation when near a nerve. We
adjust the needle position to achieve the maximal motor response in the desired
distribution. This technique enables us to exploit anatomical cues to direct
needle movement. For example, stimulation of the phrenic nerve (the patient
will hiccup) when performing an interscalene block tells us the brachial plexus
lies just a centimeter lower in the neck.
Indications
Peripheral
nerve blocks may be performed for operative procedures, as well as for
post-operative pain management. Through blockade of nerve impulses, pre-emptive
analgesia may be obtained. Furthermore, catheter techniques enable
post-operative pain management with continuous infusions of local anesthetic
and/or opioids. Such infusions can improve perfusion to the operative
extremity, reduce pain with movement, speed recovery, and improve quality of
life even weeks after the operation.
Related Topics