Chapter: Pathology: Joint Pathology
Osteoarthritis
OSTEOARTHRITIS
Osteoarthritis (OA) (degenerative joint disease) is joint
degeneration with loss of articular cartilage, with no to minimal inflammation. It is the
most common form of arthritis. Risk increases with age; OA affects at least 1
joint in 80% of people age >70.
Clinically, there is an
insidious onset of joint stiffness; deep, aching joint pain, which worsens with
repetitive motion; decreased range of motion; crepitus; and joint effu-sions
and swelling. Osteophytes may cause nerve compression. X-ray studies show
narrowing of the joint space due to loss of cartilage; osteosclerosis and bone
cysts; and osteophytes (osteophytic lipping).
The pathogenesis involves
both biomechanical factors (aging or wear and tear of articular cartilage) and
biochemical factors (chondrocyte injury and abnormal colla-gen activity).
Predisposing factors include obesity, previous joint injury, ochronosis,
diabetes, and hemarthrosis.
OA affects weight-bearing
joints (knees, hips, and spine), often with asymmetrical involvement.
•
There is degeneration and loss of articular cartilage with
eburnation (exposed bone becomes polished) and subchondral bone sclerosis.
•
The changes may include subchondral bone cysts, loose bodies (joint
mice), which are free-floating fragments of cartilage and bone, and osteophytes
(bone spurs), which are reactive bony outgrowths.
•
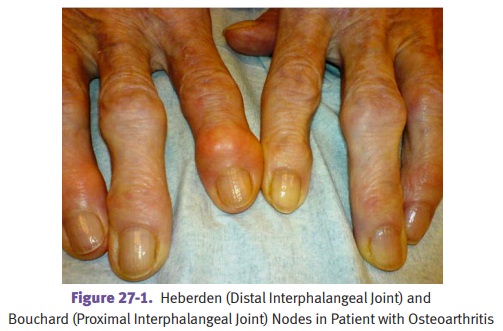
Heberden nodes are osteophytes at the distal
interphalangeal (DIP) joints, while Bouchard nodes are osteophytes at the
proximal interphalangeal (PIP) joints.
Related Topics