Chapter: Essentials of Anatomy and Physiology: An Introduction to Microbiology and Human Disease
Normal Flora
NORMAL FLORA
Each of us has a natural population of microorganisms living on and within us. This is our normal flora. These microbes may be further categorized as resi-dents or transients. Resident flora are those species that live on or in nearly everyone almost all the time. These residents live in specific sites, and we provide a very favorable environment for them. Some, such as Staphylococcus epidermidis, live on the skin. Others, such as E. coli, live in the colon and small intestine. When in their natural sites, resident flora do not cause harm to healthy tissue, and some are even beneficial to us. However, residents may become pathogenic if they are introduced into abnormal sites. If E. coli, for exam-ple, gains access to the urinary bladder, it causes an infection called cystitis. In this situation, E. coli is con-sidered an opportunist, which is a normally harmless species that has become a pathogen in special circum-stances.
Transient flora are those species that are found periodically on or in the body; they are not as well adapted to us as are the resident flora. Streptococcus pneumoniae, for example, is a transient in the upper res-piratory tract, where it usually does not cause harm in healthy people. However, transients may become path-ogenic when the host’s resistance is lowered. In an eld-erly person with influenza, S. pneumoniae may invade the lower respiratory tract and cause a serious or even fatal pneumonia.
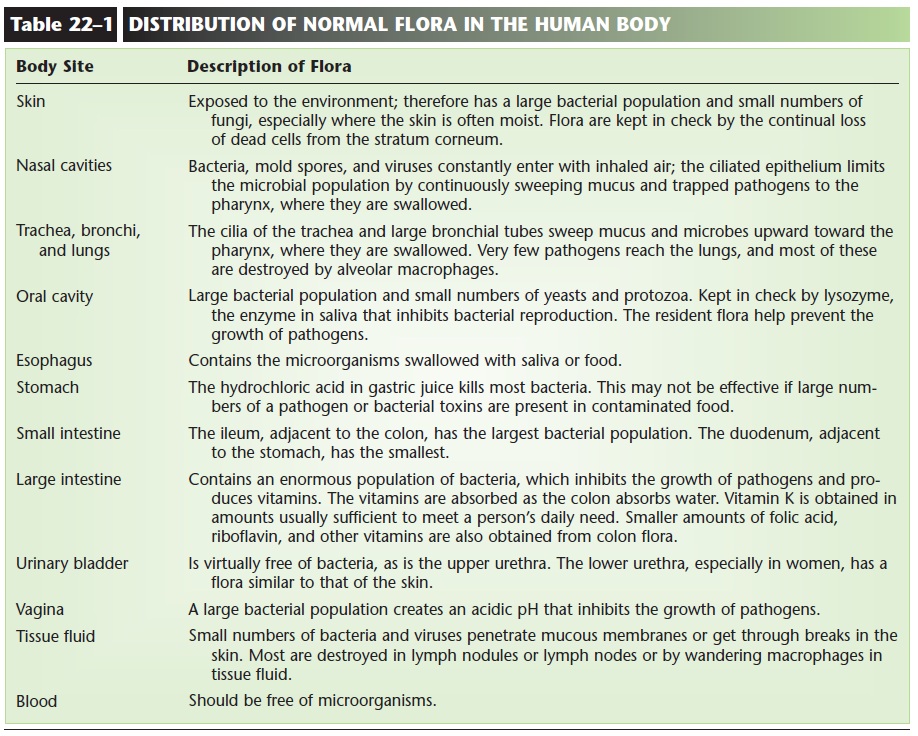
The distribution of our normal flora is summarized in Table 22–1. You can see that an important function of normal flora is to inhibit the growth of pathogens in the oral cavity, intestines, and in women, the vagina. The resident bacteria are believed to do this by pro-ducing antibacterial chemicals but also by simply being there and providing competition that makes it difficult for pathogens to establish themselves. An example may be helpful here. Let us use botulism. Typical food-borne botulism is acquired by ingesting the bacterial toxin that has been produced in food. Infants, however, may acquire botulism by ingesting the spores (dormant forms) of the botulism bacteria on foods such as honey or raw vegetables. The infant’s colon flora is not yet abundant, and the botulism spores may be able to germinate into active cells that produce toxin in the baby’s own intestine. For older children or adults, botulism spores are harmless if ingested, because the normal colon flora prevents the growth of these bacteria.
Recent research suggests that some specific bacte-ria in our colon flora are even more important than we thought. One species,Bacteroides fragilis, produces a polysaccharide, Psac, that may be necessary for the normal development of certain aspects of the human immune system: production of normal T cells by the thymus gland and the proper functioning of the spleen. We have much more to learn about our rela-tionship with our resident flora.
Resident flora may be diminished by the use of antibiotics to treat bacterial infections. An antibiotic does not distinguish between the pathogen and the resident bacteria. In such circumstances, without the usual competition, yeasts or pathogenic bacteria may be able to overgrow and create new infections. This is most likely to occur on mucous membranes such as those of the oral cavity and vagina.
Related Topics