Chapter: Medical Physiology: General Principles of Gastrointestinal Function- Motility, Nervous Control, and Blood Circulation
Neural Control of Gastrointestinal Function- Enteric Nervous System
Neural Control of Gastrointestinal Function- Enteric Nervous System
The gastrointestinal tract has a nervous system all its own called the enteric nervous system.
It lies entirely in the wall of the gut, beginning in the esophagus and extending all the way to the anus. The number of neurons in this enteric system is about 100 million, almost exactly equal to the number in the entire spinal cord. This highly developed enteric nervous system is especially important in controlling gastrointestinal movements and secretion.
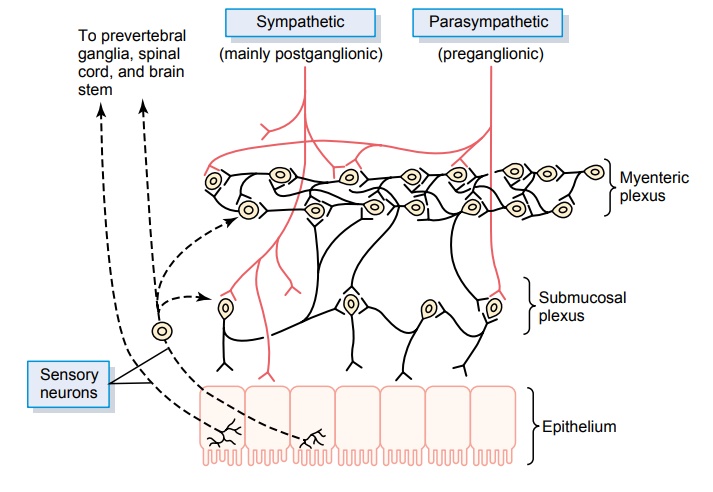
The enteric nervous system is composed mainly of two plexuses, shown in Figure 62–4: (1) an outer plexus lying between the longitudinal and circular muscle layers, called the myenteric plexus or Auerbach’splexus, and (2) an inner plexus, called the submucosal plexus or Meissner’s plexus, that lies in the submucosa.The nervous connections within and between these two plexuses are also shown in Figure 62–4.
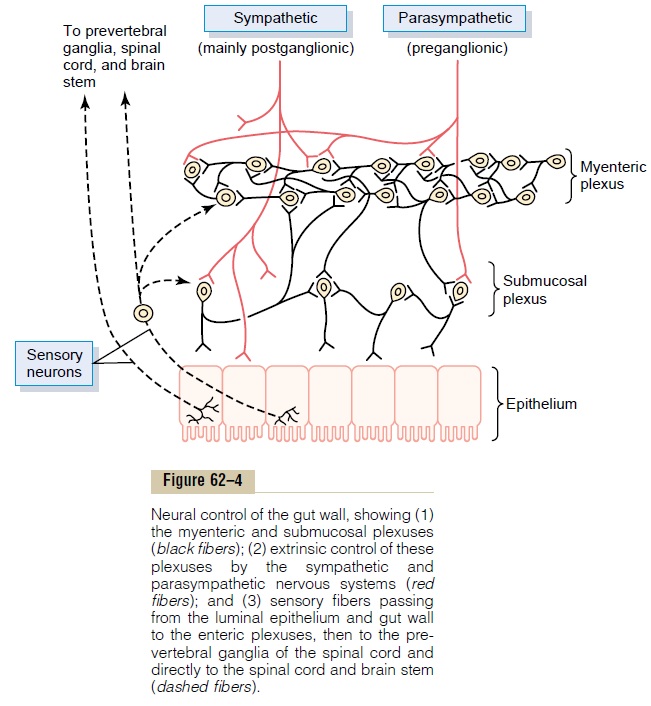
The myenteric plexus controls mainly the gastroin-testinal movements, and the submucosal plexus con-trols mainly gastrointestinal secretion and local blood flow.Note especially in Figure 62–4 the extrinsic sympa-thetic and parasympathetic fibers that connect to both the myenteric and submucosal plexuses. Although the enteric nervous system can function on its own, inde-pendently of these extrinsic nerves, stimulation by the parasympathetic and sympathetic systems can greatly enhance or inhibit gastrointestinal functions, as we discuss later.
Also shown in Figure 62–4 are sensory nerve endings that originate in the gastrointestinal epithe-lium or gut wall and send afferent fibers to both plexuses of the enteric system, as well as (1) to the pre-vertebral ganglia of the sympathetic nervous system, (2) to the spinal cord, and (3) in the vagus nerves all the way to the brain stem. These sensory nerves can elicit local reflexes within the gut wall itself and still other reflexes that are relayed to the gut from either the prevertebral ganglia or the basal regions of the brain.
Differences Between the Myenteric and Submucosal Plexuses
The myenteric plexus consists mostly of a linear chain of many interconnecting neurons that extends the entire length of the gastrointestinal tract. A section of this chain is shown in Figure 62–4.
Because the myenteric plexus extends all the way along the intestinal wall and because it lies between the longitudinal and circular layers of intestinal smooth muscle, it is concerned mainly with controlling muscle activity along the length of the gut. When this plexus is stimulated, its principal effects are (1) increased tonic contraction, or “tone,” of the gut wall, increased intensity of the rhythmical contractions, slightly increased rate of the rhythm of contraction, and (4) increased velocity of conduction of excitatory waves along the gut wall, causing more rapid move-ment of the gut peristaltic waves.
The myenteric plexus should not be considered entirely excitatory because some of its neurons are inhibitory; their fiber endings secrete an inhibitorytransmitter, possibly vasoactive intestinal polypeptide or some other inhibitory peptide. The resulting inhibitory signals are especially useful for inhibiting some of the intestinal sphincter muscles that impede movement of food along successive segments of the gastrointestinal tract, such as the pyloric sphincter, which controls emptying of the stomach into the duo-denum, and the sphincter of the ileocecal valve, which controls emptying from the small intestine into the cecum.
The submucosal plexus, in contrast to the myenteric plexus, is mainly concerned with controlling function within the inner wall of each minute segment of the intestine. For instance, many sensory signals originate from the gastrointestinal epithelium and are then integrated in the submucosal plexus to help control local intestinal secretion, local absorption, and local contraction of the submucosal muscle that causesvarious degrees of infolding of the gastrointestinal mucosa.
Types of Neurotransmitters Secreted by Enteric Neurons
In an attempt to understand better the multiple func-tions of the gastrointestinal enteric nervous system, research workers the world over have identified a dozen or more different neurotransmitter substances that are released by the nerve endings of different types of enteric neurons. Two of them with which we are already familiar are (1) acetylcholine and (2) nor-epinephrine. Others are (3) adenosine triphosphate, (4) serotonin, (5)dopamine, (6) cholecystokinin, (7) substance P, (8) vasoactive intestinal polypeptide, (9) somatostatin, (10) leu-enkephalin, (11) met-enkephalin, and (12) bombesin. The specific functionsof many of these are not known well enough to justify discussion here, other than to point out the following.
Acetylcholine most often excites gastrointestinalactivity. Norepinephrine almost always inhibits gas-trointestinal activity. This is also true ofepinephrine, which reaches the gastrointestinal tract mainly by way of the blood after it is secreted by the adrenal medul-lae into the circulation. The other aforementioned transmitter substances are a mixture of excitatory and inhibitory agents.
Autonomic Control of the Gastrointestinal Tract Parasympathetic Innervation. The parasympathetic sup-ply to the gut is divided into cranial and sacral divisions.
Except for a few parasympathetic fibers to the mouth and pharyngeal regions of the alimentary tract, the cranial parasympathetic nerve fibers are almost entirely in the vagus nerves. These fibers provide extensive innervation to the esophagus, stomach, and pancreas and somewhat less to the intestines down through the first half of the large intestine.
The sacral parasympathetics originate in the second, third, and fourth sacral segments of the spinal cord and pass through the pelvic nerves to the distal half of the large intestine and all the way to the anus. The sig-moidal, rectal, and anal regions are considerably better supplied with parasympathetic fibers than are the other intestinal areas. These fibers function especially to execute the defecation reflexes.
The postganglionic neurons of the gastrointestinal parasympathetic system are located mainly in the myenteric and submucosal plexuses. Stimulation of these parasympathetic nerves causes general increase in activity of the entire enteric nervous system. This in turn enhances activity of most gastrointestinal functions.
Sympathetic Innervation. The sympathetic fibers to thegastrointestinal tract originate in the spinal cord between segments T-5 and L-2. Most of the pregan-glionic fibers that innervate the gut, after leaving the cord, enter the sympathetic chains that lie lateral to the spinal column, and many of these fibers then pass on through the chains to outlying ganglia such as to the celiac ganglion and various mesenteric ganglia. Most ofthe postganglionic sympathetic neuron bodies are in these ganglia, and postganglionic fibers then spread through postganglionic sympathetic nerves to all parts of the gut.. The sympathetics innervate essentially all of the gastrointestinal tract, rather than being more extensive nearest the oral cavity and anus as is true of the parasympathetics. The sympathetic nerve endings secrete mainly norepinephrine but also small amounts of epinephrine.
In general, stimulation of the sympathetic nervous system inhibits activity of the gastrointestinal tract, causing many effects opposite to those of the parasympathetic system. It exerts its effects in two ways: (1) to a slight extent by direct effect of secreted norepinephrine to inhibit intestinal tract smooth muscle (except the mucosal muscle, which it excites) and (2) to a major extent by an inhibitory effect of norepinephrine on the neurons of the entire enteric nervous system.
Strong stimulation of the sympathetic system can inhibit motor movements of the gut so greatly that this literally can block movement of food through the gas-trointestinal tract.
Afferent Sensory Nerve Fibers from the Gut
Many afferent sensory nerve fibers innervate the gut. Some of them have their cell bodies in the enteric nervous system itself and some in the dorsal root ganglia of the spinal cord. These sensory nerves can be stimulated by (1) irritation of the gut mucosa, (2) excessive distention of the gut, or (3) presence of spe-cific chemical substances in the gut. Signals trans-mitted through the fibers can then cause excitation or, under other conditions,inhibition of intestinal move-ments or intestinal secretion.
In addition, other sensory signals from the gut go all the way to multiple areas of the spinal cord and even the brain stem. For example, 80 per cent of the nerve fibers in the vagus nerves are afferent rather than efferent. These afferent fibers transmit sensory signals from the gastrointestinal tract into the brain medulla, which in turn initiates vagal reflex signals that return to the gastrointestinal tract to control many of its functions.
Gastrointestinal Reflexes
The anatomical arrangement of the enteric nervous system and its connections with the sympathetic and parasympathetic systems support three types of gas-trointestinal reflexes that are essential to gastroin-testinal control. They are the following:
1.Reflexes that are integrated entirely within the gut wall enteric nervous system. These include reflexesthat control much gastrointestinal secretion, peristalsis, mixing contractions, local inhibitory effects, and so forth.
2.Reflexes from the gut to the prevertebral sympathetic ganglia and then back to the gastrointestinal tract. These reflexes transmitsignals long distances to other areas of the gastrointestinal tract, such as signals from the stomach to cause evacuation of the colon (the gastrocolic reflex), signals from the colon andsmall intestine to inhibit stomach motility and stomach secretion (the enterogastric reflexes), and reflexes from the colon to inhibit emptying of ileal contents into the colon (the colonoileal reflex).
3.Reflexes from the gut to the spinal cord or brain stem and then back to the gastrointestinal tract.
These include especially (1) reflexes from the stomach and duodenum to the brain stem and back to the stomach—by way of the vagus nerves—to control gastric motor and secretory activity; (2) pain reflexes that cause general inhibition of the entire gastrointestinal tract; and (3) defecation reflexes that travel from the colon and rectum to the spinal cord and back again to produce the powerful colonic, rectal, and abdominal contractions required for defecation (the defecation reflexes).
Hormonal Control of Gastrointestinal Motility
We discuss the extreme importance of several hormones for controlling gastrointestinal secretion. Most of these same hormones also affect motility in some parts of the gastrointestinal tract. Although the motility effects are usually less important than the secretory effects of the hormones, some of the more important of them are the following.
Gastrin is secreted by the “G” cells of the antrum of the stomach in response to stimuli associated withingestion of a meal, such as distention of the stomach, the products of proteins, and gastrin releasing peptide, which is released by the nerves of the gastric mucosa during vagal stimulation. The primary actions of gastrin are (1) stimulation of gastric acid secretion and(2) stimulation of growth of the gastric mucosa.
Cholecystokinin is secreted by “I” cells in the mucosa of the duodenum and jejunum mainly inresponse to digestive products of fat, fatty acids, and monoglycerides in the intestinal contents. This hormone strongly contracts the gallbladder, expelling bile into the small intestine where the bile in turn plays important roles in emulsifying fatty substances, allow-ing them to be digested and absorbed. Cholecystokinin also inhibits stomach contraction moderately. There-fore, at the same time that this hormone causes emp-tying of the gallbladder, it also slows the emptying of food from the stomach to give adequate time for diges-tion of the fats in the upper intestinal tract.
Secretin was the first gastrointestinal hormone dis-covered and is secreted by the “S” cells in the mucosa of the duodenum in response to acidic gastric juiceemptying into the duodenum from the pylorus of the stomach. Secretin has a mild effect on motility of the gastrointestinal tract and acts to promote pancreatic secretion of bicarbonate which in turn helps to neu-tralize the acid in the small intestine.
Gastric inhibitory peptide is secreted by the mucosa of the upper small intestine, mainly in response to fattyacids and amino acids but to a lesser extent in response to carbohydrate. It has a mild effect in decreasing motor activity of the stomach and therefore slows emptying of gastric contents into the duodenum when the upper small intestine is already overloaded with food products.
Motilin is secreted by the upper duodenum duringfasting, and the only known function of this hormone is to increase gastrointestinal motility. Motilin is released cyclically and stimulates waves of gastroin-testinal motility called interdigestive myoelectric com-plexes that move through the stomach and smallintestine every 90 minutes in a fasted person. Motilin secretion is inhibited after ingestion by mechanisms that are not fully understood.
Related Topics