Chapter: Medical Physiology: General Principles of Gastrointestinal Function- Motility, Nervous Control, and Blood Circulation
Effect of Gut Activity and Metabolic Factors on Gastrointestinal Blood Flow
Effect of Gut Activity and Metabolic Factors on Gastrointestinal Blood Flow
Under normal conditions, the blood flow in each area of the gastrointestinal tract, as well as in each layer of the gut wall, is directly related to the level of local activity. For instance, during active absorption of nutri-ents, blood flow in the villi and adjacent regions of the submucosa is increased as much as eightfold. Likewise, blood flow in the muscle layers of the intestinal wall increases with increased motor activity in the gut. For instance, after a meal, the motor activity, secretory activity, and absorptive activity all increase; likewise, the blood flow increases greatly but then decreases back to the resting level over another 2 to 4 hours.
Possible Causes of the Increased Blood Flow During Gastroin-testinal Activity. Although the precise cause or causesof the increased blood flow during increased gastroin-testinal activity are still unclear, some facts are known.
First, several vasodilator substances are released from the mucosa of the intestinal tract during the digestive process. Most of these are peptide hormones, including cholecystokinin, vasoactive intestinal peptide, gastrin, and secretin. These same hormones controlspecific motor and secretory activities of the gut.
Second, some of the gastrointestinal glands also release into the gut wall two kinins, kallidin and bradykinin, at the same time that they secrete theirsecretions into the lumen. These kinins are powerful vasodilators that are believed to cause much of the increased mucosal vasodilation that occurs along with secretion.
Third, decreased oxygen concentration in the gut wall can increase intestinal blood flow at least 50 to 100 per cent; therefore, the increased mucosal and gut wall metabolic rate during gut activity probably lowers the oxygen concentration enough to cause much of the vasodilation. The decrease in oxygen can also lead to as much as a fourfold increase of adenosine, a well-known vasodilator that could be responsible for much of the increased flow.
Thus, the increased blood flow during increased gas-trointestinal activity is probably a combination of many of the aforementioned factors plus still others yet undiscovered.
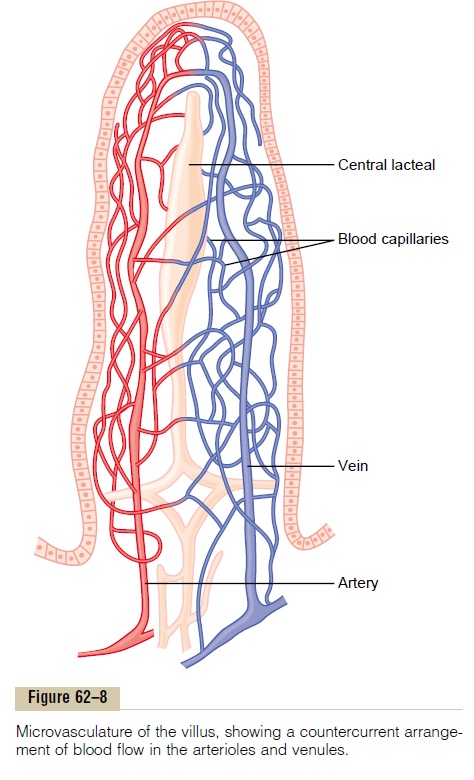
“Countercurrent” Blood Flow in the Villi. Note in Figure 62–8 that the arterial flow into the villus and the venous flow out of the villus are in directions opposite to each other, and that the vessels lie in close apposi-tion to each other. Because of this vascular arrange-ment, much of the blood oxygen diffuses out of the arterioles directly into the adjacent venules without ever being carried in the blood to the tips of the villi. As much as 80 per cent of the oxygen may take this short-circuit route and therefore not be available for local metabolic functions of the villi. The reader will recognize that this type of countercurrent mechanism in the villi is analogous to the countercurrent mecha-nism in the vasa recta of the kidney medulla.
Under normal conditions, this shunting of oxygen from the arterioles to the venules is not harmful to the villi, but in disease conditions in which blood flow to the gut becomes greatly curtailed, such as in circula-tory shock, the oxygen deficit in the tips of the villi can become so great that the villus tip or even the whole villus suffers ischemic death and can disintegrate. Therefore, for this reason and others, in many gas-trointestinal diseases the villi become seriously blunted, leading to greatly diminished intestinal absorptive capacity.
Related Topics