Chapter: Nutrition and Diet Therapy: Diet and Cardiovascular Disease
Myocardial Infarction
MYOCARDIAL INFARCTION
Myocardial infarction
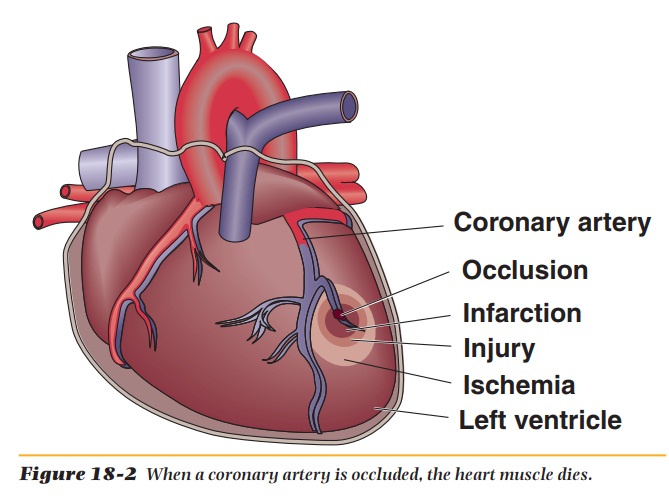
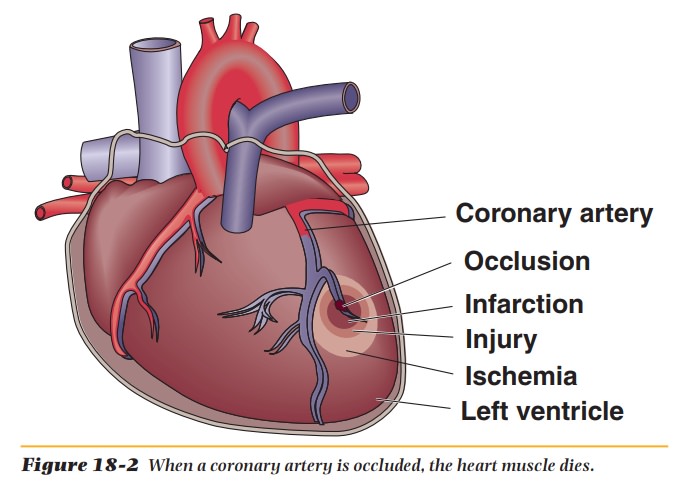
is caused by the blockage of a coronary artery supplying blood to the heart. The
heart tissue denied blood because of this blockage dies (see Figure 18-2).
Atherosclerosis is a primary cause, but hypertension, abnormal blood clotting,
and infection such as that caused by rheumatic fever (which damages heart
valves) are also contributory factors.
After the attack, the
client is in shock. This causes a fluid shift, and the client may feel thirsty.
The client should be given nothing by mouth (NPO), however, until the physician
evaluates the condition. If the client remains nauseated after the period of
shock, IV infusions are given to prevent dehydration.
After several hours,
the client may begin to eat. A liquid diet may be recom-mended for the first 24
hours. Following that, a low-cholesterol–low-sodium diet is usually given, with
the client regulating the amount eaten.
Foods should not be
extremely hot or extremely cold. They should be easy to chew and digest and
contain little roughage so that the work of the heart will be minimal. Both
chewing and the increased activity of the gastrointestinal tract that follow
ingestion of high-fiber foods cause extra work for the heart. The percentage of
energy nutrients will be based on the particular needs of the client, but, in
most cases, the types and amounts of fats will be limited. Sodium is usually
limited to prevent fluid accumulation. Some physicians will order a restriction
on the amount of caffeine for the first few days after an MI. The dual goal is
to allow the heart to rest and its tissue to heal.
Related Topics