Chapter: Medical Microbiology: An Introduction to Infectious Diseases: Nosocomial Infections and Infection Control
History: Semmelweis and Childbed Fever
HISTORY: SEMMELWEIS AND CHILDBED FEVER
The shining example of the fundamental importance of epidemiology in detection and control of nosocomial infections is the work of Ignaz Semmelweis, which preceded the microbiologic discoveries of Pasteur and Koch by a decade. Semmelweis was assistant obstetrician at the Vienna General Hospital, where more than 7000 infants were delivered each year. Childbed fever (puerperal endometritis), which we now know is caused pri-marily by group A streptococci, was a major problem accounting for 600 to 800 maternal deaths per year. By careful review of hospital statistics between 1846 and 1849, Semmel-weis clearly showed that the death rate in one of the two divisions of the hospital was 10 times that in the other. Division I, which had the high mortality, was the teaching unit in which all deliveries were by obstetricians and students. In division II, all deliveries were by midwives. No similar epidemic existed elsewhere in the city of Vienna, and mor-tality was very low in mothers delivering at home.
Semmelweis postulated that the key difference between divisions I and II was partici-pation of the physicians and students in autopsies. One or more cadavers were dissected daily, some from cases of childbed fever and other infections. Handwashing was perfunc-tory, and Semmelweis believed this allowed the transmission of “invisible cadaver parti-cles” by direct contact between the mother and the physician’s hands during examinations and delivery. In 1847, as a countermeasure, he required handwashing with a chlorine so-lution until the hands were slippery and the odor of the cadaver was gone. The results were dramatic. The full effect of the chlorine handwashing can be seen by comparing mortality in the two divisions for 1846 and 1848 (Table 72 – 1). The mortality in division I was reduced to that of division II, and both were below 2%.
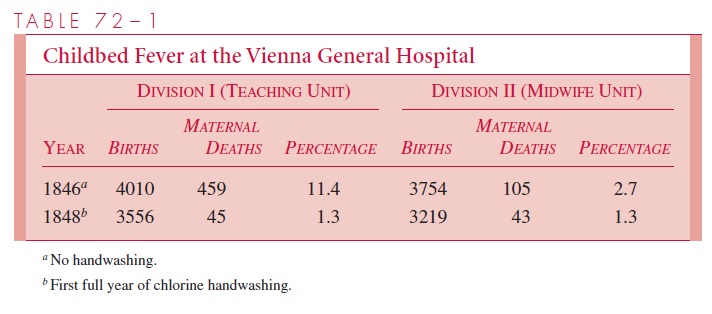
Unfortunately, because of his personality and failure to publish his work until 1860, Semmelweis’ contribution was not generally appreciated in his lifetime. As his frustration mounted over lack of acceptance of his ideas, he became abusive and irrational, eventu-ally alienating even his early supporters. Some believe that he also suffered from Alzheimer’s disease. He died in an insane asylum in 1865, unaware that his concept of spread via direct contact would later be recognized as the most important mechanism of nosocomial infection and that handwashing would remain the most important means of infection control in hospitals.
Related Topics