Chapter: Medical Microbiology: An Introduction to Infectious Diseases: Nosocomial Infections and Infection Control
Nosocomial Infection Control and Prevention
INFECTION CONTROL
Infection control is the sum of all the means used to prevent nosocomial infections. Historically, such methods have been developed as an integral part of the study of infec-tious diseases, often serving as key elements in the proof of infectious etiology. Semmel-weis’ handwashing is the first example. Later in the 19th century, Joseph Lister achieved a dramatic reduction in surgical wound infections by infusion of a phenolic antiseptic into wounds. This local destruction of organisms was known as antisepsis,and it some-times included liberal applications of disinfectants, including sprays to the environment. As it became recognized that contamination of wounds was not inevitable, the emphasis gradually shifted to preventing contact between microorganisms and susceptible sites, a concept called asepsis. Asepsis, which combines containment with the methods of steril-ization and disinfection discussed, is the central concept of infection control. The measures taken to achieve asepsis vary, depending on whether the circum-stances and environment are most similar to the operating room, hospital ward, or outpa-tient clinic.
Asepsis
Operating Room
The surgical suite and operating room represent the most controlled and rigid application of aseptic principles. The procedure begins with the use of an antiseptic scrub of the skin over the operative site and the hands and forearms of all who will have contact with the patient. The use of sterile drapes, gowns, and instruments serves to prevent spread through direct contact, and caps and face masks reduce airborne spread from personnel to the wound. As all students learn the first time they scrub, even the manner of dressing andmoving in the operating room are rigidly specified, and those involved assume a strict aseptic attitude as well as their masks and gowns. In some hospitals, the air entering the operating room is filter sterilized, but this practice is expensive and its value unproved. The level of bacteria in the air is generally more related to the number of persons and amount of movement in the operating room than to incoming air. The net effect of these procedures is to draw a sterile curtain around the operative site, thus minimizing contact with microorganisms. Surgical asepsis is also used in other areas where invasive special procedures such as cardiac catheterization are performed.
Hospital Ward
Although theoretically desirable, strict aseptic procedures as used in the operating room are impractical in the ward setting. Asepsis is practiced by the use of sterile needles, medications,dressings, and other items that could serve as transmission vehicles if contaminated.A “no touch” technique for examining wounds and changing dressings eliminates direct contact with any nonsterile item. Invasive procedures such as catheter insertion and lumbar punctures are performed under aseptic precautions similar to those used in theoperatingroom. In all circumstances, handwashing between patient contacts is the single most important aseptic precaution.
Outpatient Clinic
The general, aseptic practices used on the hospital ward are also appropriate to the outpa-tient situation as preventive measures. The potential for cross-infection in the clinic or waiting room is obvious but has been little studied regarding preventive measures. Pa-tients who may be infected should be segregated whenever possible using techniques sim-ilar to those of hospital ward isolation. The examining room may be used in a manner analogous to the private rooms on a hospital ward. Although this approach is difficult be-cause of patient turnover, it should be attempted for infections that would require strict or respiratory isolation in the hospital.
Isolation Procedures
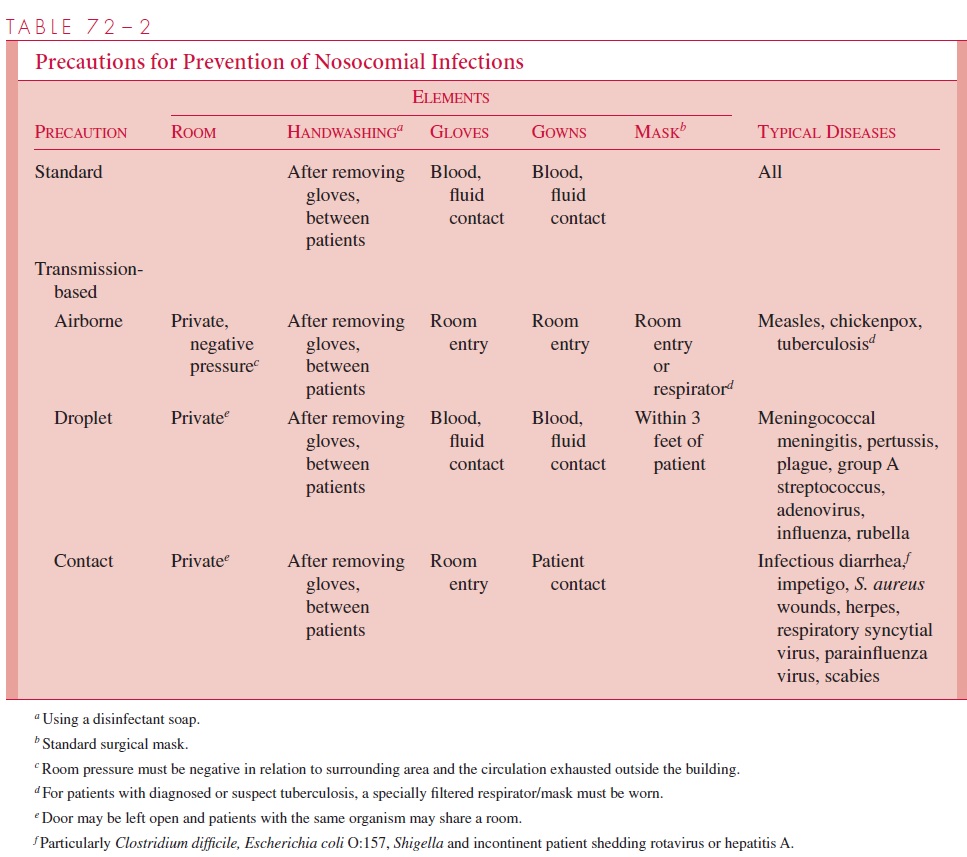
Patients with infections pose special problems, because they may transmit their infections to other patients either directly or by contact with a staff member. This additional risk is managed by the techniques of isolation, which place barriers between the infected patient and others on the ward. Because not every infected patient presents with suspect signs and/or symptoms, some precaution should be taken with all patients. In the system rec-ommended by the Centers for Disease Control and Prevention, these are called standardprecautions and include the use of gowns and gloves when in contact with patient bloodor secretions. These are particularly directed at protecting health care workers from HIV and hepatitis infection. For those with suspect or proven infection, additional precautions are taken, the nature of which is determined by the known mode of transmission of the organism. These transmission-based precautions are divided into those directed at air-borne, droplet, and contact routes. Theairborne transmission precautions are for infec-tions known to be transmitted by extremely small ( <5μm) particles suspended in the air. This requires that the room air circulation be maintained with negative pressure relative to the surrounding area and be exhausted to the outside. Those entering the room must wear surgical masks, and in the case of tuberculosis, specially designed respirators. Droplet precautions are for infections where the organisms are suspended in larger droplets, which may be airborne, but generally do not travel more than 3 feet from the patient who generates them. These can be contained by the use of gowns, gloves, and masks when working close to the patient. Contact precautions are used for infections that require di-rect contact with organisms on or pass in secretions of the patient. Diarrheal infections are of special concern because of the extent to which they contaminate the environment. Details of the precautions and examples of the typical infectious agents are summarized in Table 72 – 2.
Organization
Modern hospitals are required to have formal infection control programs that include aninfection control committee, epidemiology service, and educational activities. The infection
control committee is composed of representatives of various medical, administrative,nursing, housekeeping, and support services. The committee establishes the institution’sinfection control procedures and regularly reviews information on the status of nosocomialinfections in the hospital. When epidemiologic circumstances warrant it, the committeeis empowered to take drastic action such as closing a hospital unit or suspending aphysician’s privileges.
The epidemiology service is the working arm of the infection control committee. Its functions are performed by one or more epidemiologists who usually have a nursingbackground. This work requires familiarity with clinical microbiology, epidemiology, infectiousdisease, and hospital procedures, as well as immense tact. The main activities aresurveillance and outbreak investigation. Surveillance is the collection of data documentingthe frequency and nature of nosocomial infections in the hospital to detect deviationsfrom the institutional or national norms. Although routine microbiologic sampling of thehospital environment is of no value, programs to sample some of the medical devicesknown to be nosocomial hazards can be useful. On-the-spot investigation of potential outbreaksallows early implementation of preventive measures. This activity is probably thesingle most important function of the epidemiology service. Suspicion of an increased number of infections leads to an investigation to verify the facts, establish basic epidemi-ologic associations, and relate them to preventive measures. The primary concern is cross-infection, in which a virulent organism is being transmitted from patient to patient. Solution of the problem may require additional microbiologic investigations, such as bacteriophage typing of S. aureus.
PREVENTION
The prevention of nosocomial infections is contingent on basic and applied knowledge drawn from all parts of this book. Applied with common sense, these principles can both prevent disease and reduce the costs of medical care.
Related Topics