Chapter: Medical Physiology: Transport of Oxygen and Carbon Dioxide in Blood and Tissue Fluids
Diffusion of Oxygen from the Peripheral Capillaries into the Tissue Fluid
Diffusion of Oxygen from the Peripheral Capillaries into the Tissue Fluid
When the arterial blood reaches the peripheral tissues, its PO2 in the capillaries is still 95 mm Hg. Yet, as shown in Figure 40–3, the PO2 in the interstitial fluid that sur-rounds the tissue cells averages only 40 mm Hg. Thus, there is a tremendous initial pressure difference that causes oxygen to diffuse rapidly from the capillary
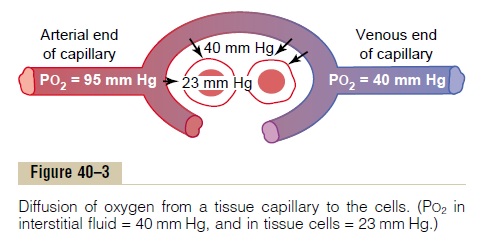
blood into the tissues—so rapidly that the capillary PO2 falls almost to equal the 40 mm Hg pressure in the interstitium. Therefore, the PO2 of the blood leaving the tissue capillaries and entering the systemic veins is also about 40 mm Hg.
Effect of Rate of Blood Flow on Interstitial Fluid PO2. If the blood flow through a particular tissue is increased, greater quantities of oxygen are transported into the tissue, and the tissue PO2 becomes correspondingly higher. This is shown in Figure 40–4. Note that an increase in flow to 400 per cent of normal increases the PO2 from 40 mm Hg (at point A in the figure) to 66 mm Hg (at point B). However, the upper limit to which the PO2 can rise, even with maximal blood flow, is 95 mm Hg, because this is the oxygen pressure in the arterial blood. Conversely, if blood flow through the tissue decreases, the tissue PO2 also decreases, as shown at point C.
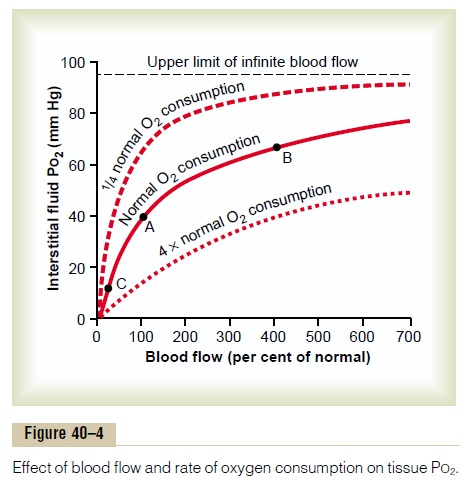
Effect of Rate of Tissue Metabolism on Interstitial Fluid PO2. Ifthe cells use more oxygen for metabolism than nor-mally, this reduces the interstitial fluid PO2. Figure 40–4 also demonstrates this effect, showing reduced intersti-tial fluid PO2 when the cellular oxygen consumption is increased, and increased PO2 when consumption is decreased.
In summary, tissue PO2 is determined by a balance between (1) the rate of oxygen transport to the tissues in the blood and (2) the rate at which the oxygen is used by the tissues.
Related Topics