Chapter: Medical Physiology: The Autonomic Nervous System and the Adrenal Medulla
Cholinergic and Adrenergic Fibers- Secretion of Acetylcholine or Norepinephrine
Basic Characteristics of Sympathetic and Parasympathetic Function
Cholinergic and Adrenergic Fibers- Secretion of Acetylcholine or Norepinephrine
The sympathetic and parasympathetic nerve fibers secrete mainly one or the other of two synaptic trans-mitter substances, acetylcholine ornorepinephrine. Those fibers that secrete acetylcholine are said to be cholinergic. Those that secrete norepinephrine are saidto be adrenergic, a term derived from adrenalin, which is an alternate name for epinephrine.
All preganglionic neurons are cholinergic in both the sympathetic and the parasympathetic nervous systems. Acetylcholine or acetylcholine-like sub-stances, when applied to the ganglia, will excite both sympathetic and parasympathetic postganglionic neurons. Either all or almost all of the postganglionicneurons of the parasympathetic system are also cholin-ergic. Conversely, most of the postganglionic sym-pathetic neurons are adrenergic. However, thepostganglionic sympathetic nerve fibers to the sweat glands, to the piloerector muscles of the hairs, and to a very few blood vessels are cholinergic.
Thus, the terminal nerve endings of the parasympa-thetic system all or virtually all secrete acetylcholine. Almost all of the sympathetic nerve endings secrete norepinephrine, but a few secrete acetylcholine. Thesehormones in turn act on the different organs to cause respective parasympathetic or sympathetic effects. Therefore, acetylcholine is called a parasympathetictransmitter and norepinephrine is called a sympathetic transmitter.
The molecular structures of acetylcholine and nor-epinephrine are the following:
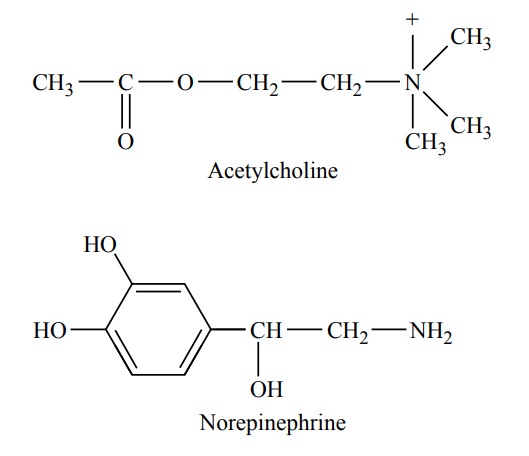
Mechanisms of Transmitter Secretion and Subsequent Removal of the Transmitter at the Postganglionic Endings
Secretion of Acetylcholine and Norepinephrine by Postgan-glionic Nerve Endings. A few of the postganglionicautonomic nerve endings, especially those of the parasympathetic nerves, are similar to but much smaller than those of the skeletal neuromuscular junc-tion. However, many of the parasympathetic nerve fibers and almost all the sympathetic fibers merely touch the effector cells of the organs that they inner-vate as they pass by; or in some instances, they termi-nate in connective tissue located adjacent to the cells that are to be stimulated. Where these filaments touch or pass over or near the cells to be stimulated, they usually have bulbous enlargements called varicosities; it is in these varicosities that the transmitter vesicles of acetylcholine or norepinephrine are synthesized and stored. Also in the varicosities are large numbers of mitochondria that supply adenosine triphosphate, which is required to energize acetylcholine or norepi-nephrine synthesis.
When an action potential spreads over the terminal fibers, the depolarization process increases the perme-ability of the fiber membrane to calcium ions, allowing these ions to diffuse into the nerve terminals or nerve varicosities. The calcium ions in turn cause the termi-nals or varicosities to empty their contents to the exte-rior. Thus, the transmitter substance is secreted.
Synthesis of Acetylcholine, Its Destruction After Secretion, and Its Duration of Action. Acetylcholine is synthesized in theterminal endings and varicosities of the cholinergic nerve fibers where it is stored in vesicles in highly con-centrated form until it is released. The basic chemical reaction of this synthesis is the following:
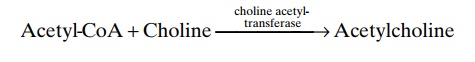
Once acetylcholine is secreted into a tissue by a cholinergic nerve ending, it persists in the tissue for a few seconds while it performs its nerve signal trans-mitter function. Then it is split into an acetate ion and choline, catalyzed by the enzyme acetylcholinesterase that is bound with collagen and glycosaminoglycans in the local connective tissue. This is the same mechanism for acetylcholine signal transmission and subsequent acetylcholine destruction that occurs at the neuro-muscular junctions of skeletal nerve fibers. The choline that is formed is then transported back into the ter-minal nerve ending, where it is used again and again for synthesis of new acetylcholine.
Synthesis of Norepinephrine, Its Removal, and Its Duration of Action. Synthesis of norepinephrine begins in the axo-plasm of the terminal nerve endings of adrenergic nerve fibers but is completed inside the secretory vesi-cles. The basic steps are the following:
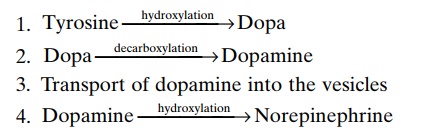
In the adrenal medulla, this reaction goes still one step further to transform about 80 per cent of the nor-epinephrine into epinephrine, as follows:
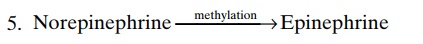
After secretion of norepinephrine by the terminal nerve endings, it is removed from the secretory site in three ways: (1) reuptake into the adrenergic nerve endings themselves by an active transport process— accounting for removal of 50 to 80 per cent of the secreted norepinephrine; (2) diffusion away from the nerve endings into the surrounding body fluids and then into the blood—accounting for removal of most of the remaining norepinephrine; and (3) destruction of small amounts by tissue enzymes (one of these enzymes is monoamine oxidase, which is found in the nerve endings, and another is catechol-O-methyl trans-ferase, which is present diffusely in all tissues).
Ordinarily, the norepinephrine secreted directly into a tissue remains active for only a few seconds, demon-strating that its reuptake and diffusion away from the tissue are rapid. However, the norepinephrine and epinephrine secreted into the blood by the adrenal medullae remain active until they diffuse into some tissue, where they can be destroyed by catechol-O-methyl transferase; this occurs mainly in the liver.
Therefore, when secreted into the blood, both norepi-nephrine and epinephrine remain very active for 10 to 30 seconds; but their activity declines to extinction over 1 to several minutes.
Related Topics