Chapter: Essential Clinical Immunology: Chronic Lymphocytic Leukemia
Characterizing the Heterogeneity of B-CLL by Molecular and Clinical Subtypes
CHARACTERIZING THE HETEROGENEITY
OF B-CLL BY MOLECULAR AND CLINICAL SUBTYPES
Based on
their mutation status, B-CLL patients can be divided into two groups: those
whose B-CLL cells use unmutated IgVH
genes (U-CLL) and those whose B-CLL cells
use mutated Ig VH genes
(M-CLL). Ini-tially, it was believed that the two types of B-CLL cells could be
generated by virgin and memory cells, respectively, although, as we shall
discuss, there is now evidence
B-CLL cells are monoclonal B-cell ex-pansions as
documented by the expression of monotypic (i.e., either κ or λ) surface
Ig and the CD19 antigen; this is in line with the presence of monoclonal
rearrange-ments of VDJ genes in the leukemic cells. Most B-CLL cells also
express activation markers and, like normal activated B cells, have low levels
of surface IgM and IgD. The expression of CD5,
usually thought of as a lineage marker, is characteristic of B-CLL cells and
should be considered part of their activation status as it can with normal B
cells when stimulated through several receptors, including the BCR. The
presence of these markers and the degree of activa-tion varies in different
B-CLL cases.
B-CLL
clones can be further subdivided based on their activation marker expres-sion:
in one subgroup, the majority of leu-kemic cells express two activation
markers, that is, CD38 and ZAP-70; and in the other, the majority of the cells
lack these markers. The two molecules appear to be involved in the regulation
of signals delivered by the BCR. The CD38+ ZAP-70+ B-CLL
subset is primarily characterized by the presence of more members of the
leukemic clone-bearing markers of activated B cells. These activation
marker-defined subgroups also differ in their expression of several other
molecules up-regulated by cellular activation.
In
comparing these two subsetting schemes – the first based on IgVH mutation status and the
second on activation markers – CD38+ZAP-70+ B-CLL clones
generally use unmutated IgVH
genes, whereas CD38−ZAP-70− B-CLL clones mainly use
mutated IgVH region genes.
Although the subdivision into CD38+ZAP-70+ U-CLL and CD38−ZAP-70−
M-CLL is true for the majority of patients, it is not universal since about 25
percent of cases are discordant for the expression of the three markers.
It is
interesting to note the correlation between the molecular characterizations of
the patients’ clones with the patients’ clinical course. Of major clinical and
inves-tigative importance are the observations that IgVH gene mutation status and ZAP-70 and CD38 expression
have clinical relevance, since cases in whom the major-ity of the cells express
CD38, ZAP-70, and exhibit unmutated IgVH
genes have a more aggressive clinical course (Figure 7.4). Correspondingly,
those patients whose clones are in the main CD38−ZAP-70−
and express mutated IgVH
genes generally fare better and have a good prognosis. In those individual
cases that are discordant for the expression of these markers, there is
nevertheless generally a direct correlation between the number of unfavorable
mark-ers and clinical outcome.
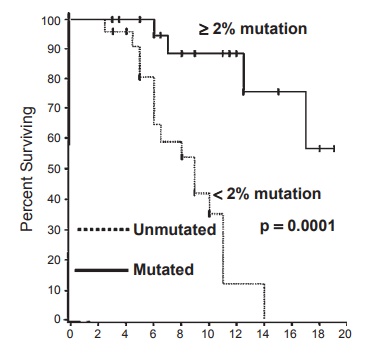
Figure 7.4 IGHV mutation status is a robust prognostic marker in B-cell-type chronic lymphocytic leukemia (B-CLL). CLL cases can be divided into two categories based on the presence of somatic mutations in the expressed IGHV gene. Those patients whose CLL cells have an IgVH gene that differs by greater than 2 percent from its germ line counterpart have a much longer survival time than those patients whose cells use an IgVH gene that differs by less than 2 percent. This distinction has major prognostic value. Reprinted by permission from Damle RN, Wasil T, Fais F, et al. IgV gene mutation status and CD38 expression as novel prognostic indicators in chronic lymphocytic leukemia. Blood. 1999;94:1840–1847.
Related Topics