Chapter: Medical Microbiology: An Introduction to Infectious Diseases: Host-Parasite Relationships
Attributes of Microbial Pathogenicity
ATTRIBUTES OF MICROBIAL PATHOGENICITY
Whether a microbe is a primary or opportunistic pathogen, it must be able to enter a host; find a unique niche; avoid, circumvent or subvert normal host defenses; and multiply. To be successful, a primary pathogen also must be transmitted to a new susceptible host or es-tablish themselves in the host for an extended period of time and eventually be transmitted.
Entry
Like all other living organisms, humans must maintain contact with the environment to see, breathe, ingest food, reproduce, and eliminate wastes. Consequently, each of the portals in the body that communicates with the outside world becomes a potential site of microbial entry. Human and other animal hosts have various protective mechanisms to pre-vent microbial entry (Table 10 – 1). A simple, although relatively efficient, mechanical bar-rier to microbial invasion is provided by intact epithelium, the most effective of which is the stratified squamous epithelium of the skin with its superficial cornified anucleate lay-ers. Organisms can gain access to the underlying tissues only by breaks or by way of hair follicles, sebaceous glands, and sweat glands that traverse the stratified layers. The surface of the skin continuously desquamates and thus tends to shed contaminating organisms. The skin also inhibits the growth of most extraneous microorganisms because of low moisture, low pH, and the presence of substances with antibacterial activity.
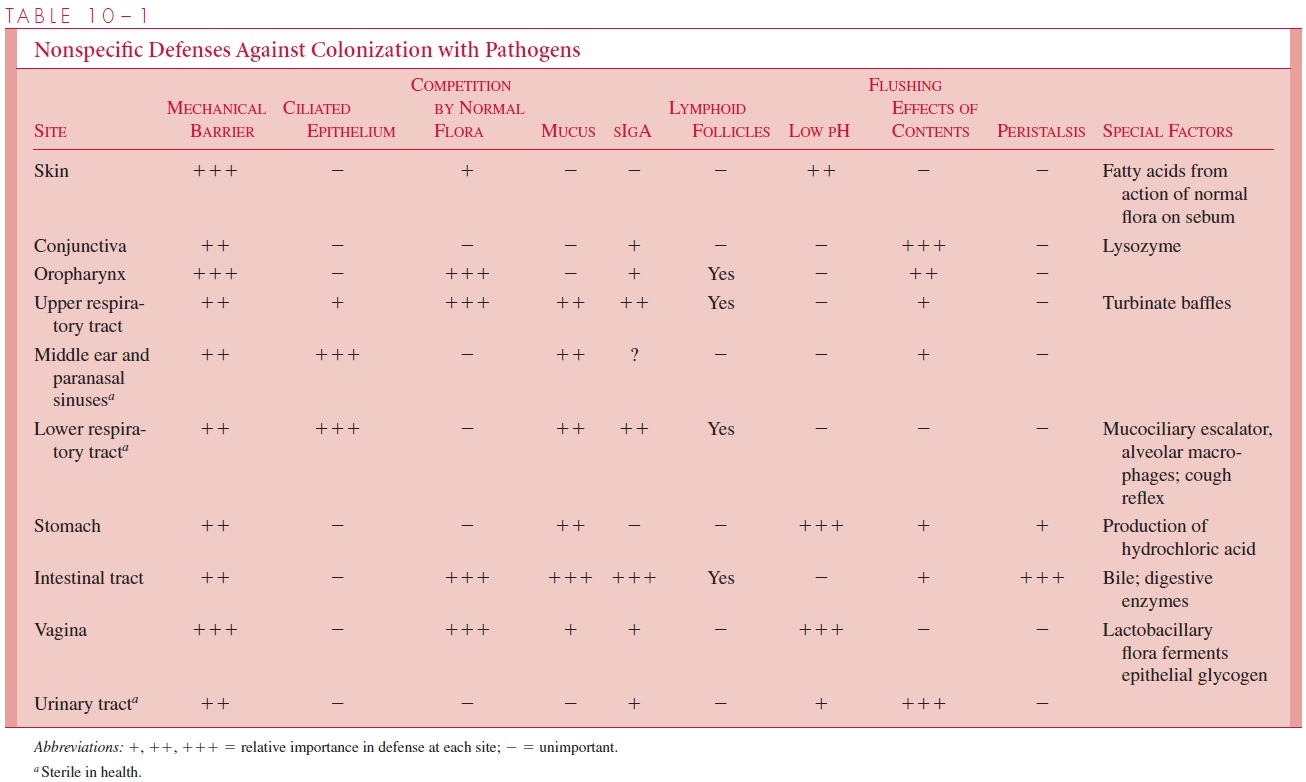
A viscous mucus covering protects the epithelium lining the respiratory tract, the gas-trointestinal tract, and urogenital system secreted by goblet cells. Microorganisms be-come trapped in the mucus layer and may be swept away before they reach the epithelial cell surface. Secretory IgA (sIgA) secreted into the mucus and other secreted antimicro-bials such as lysozyme and lactoferrin aid this cleansing process. Ciliated epithelial cells constantly move the mucus away from the lower respiratory tract. In the respiratory tract, particles larger than 5ÎĽm are trapped in this fashion. The epithelium of the intestinal tract below the esophagus is a less efficient mechanical barrier than the skin, but there are other effective defense mechanisms. The high level of hydrochloric acid and gastric enzymes in the normal stomach kill many ingested bacteria. Others are susceptible to pancreatic digestive enzymes or to the detergent effect of bile salts. Similarly, the multi-layered transitional epithelium of the urinary tract uses the flushing effect of urine and its relatively low pH as additional defense mechanisms to limit microbial entry and growth.
Urinary tract infections are much more common in women than men because the short urethra in females allows easier passage of organisms to the bladder; such infections in women are often associated with sexual intercourse.
Pathogenic organisms have evolved mechanisms to capitalize on each of these human sites of environmental contact as points of entry. Removal of the epithelial barrier and normal host cell functions makes human into the victims of opportunists. One natural method of bypassing the skin is direct inoculation by insect bites; several organisms use this route, including the plague bacillus Yersinia pestis and the malarial parasite. These microorganisms, which must spend part of their lives in remarkably different environ-ments than their mammalian hosts, have adapted mechanisms for survival. Another means in the modern world of bypassing the skin is through the deliberate inoculation used by drug addicts who suffer from a particular constellation of infectious disease agents as a result.
We still know very little about the microbial factors essential to ensure infectious trans-mission from host to host. Obviously, microbes adapted to life in humans have evolved to take advantage of existing avenues of contact between their hosts. Dissemination by aerosol is common, but success is more than just random chance; the parasite must design itself for the rigors of atmospheric drying and other environmental factors. The virus of the common cold must exist on inanimate objects (fomites) waiting for a hand to touch and carry them to the conjunctiva or nasopharynx. The burden on an enteric pathogen that fol-lows the fecal – oral route is substantial: feces, mouth to stomach to small bowel to large bowel and back to the cold cruel world in stool. Thus, bacteria causing enteric infection are exposed to extremes of temperature, pH, bile salts, digestive enzymes, and a myriad of competing microorganisms. Sexually transmitted pathogens ordinarily are delivered by di-rect inoculation onto mucosal surfaces. This microbial strategy avoids life in the external environment but is not without its own set of special requirements to overcome changing pH, mucus obstruction, anatomic barriers, local antibodies, and phagocytic cells.
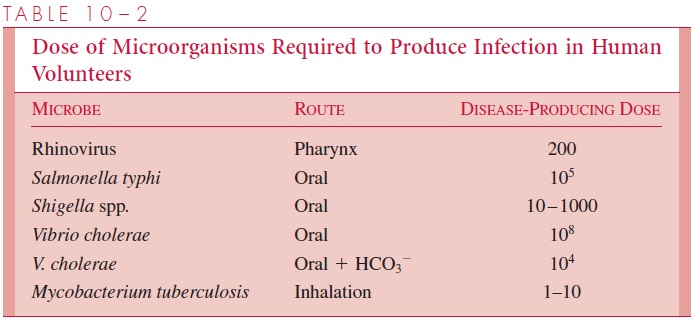
All of the factors in the initial encounter of the host with the parasite can be assessed to some degree by measuring the infectious dose of the organism. How many organisms must be given a host to ensure infection in some proportion of the individuals? The mea-sure of the infectious dose-50 (ID50) for several pathogens is shown in Table 10 – 2. It is a simple measurement of a very complex interaction. Moreover, it is somewhat misleading, as the endpoint is disease in human volunteers or death (a rigorous endpoint) in animal experiments.
Related Topics