Chapter: Clinical Anesthesiology: Anesthetic Management: Anesthesia for Otorhinolaryngologic Surgery
Anesthesia for Nasal & Sinus Surgery
NASAL & SINUS SURGERY
Common nasal and sinus surgeries include polyp-ectomy, endoscopic sinus
surgery, maxillary sinus-otomy (Caldwell–Luc procedure), rhinoplasty, and
septoplasty.
Preoperative Considerations
Patients undergoing nasal or sinus surgery may have a considerable
degree of preoperative nasal obstruc-tion caused by polyps, a deviated septum,
or muco-sal congestion from infection. This may make face mask ventilation
difficult, particularly if combined with other causes of difficult ventilation
(eg, obesity, maxillofacial deformities).
Nasal polyps are often associated with
allergic disorders, such as asthma. Patients who also have a history of
allergic reactions to aspirin should not be given any nonsteroidal
antiinflammatory drugs (including ketorolac) for postoperative analgesia. Nasal
polyps are a common feature of cystic fibrosis.
Because of the rich vascular supply of the nasal mucosa, the
preoperative interview should concen-trate on questions concerning medication
use (eg, aspirin, clopidogrel) and any history of bleeding problems.
Intraoperative Management
Many nasal procedures can be satisfactorily
per-formed under local anesthesia with sedation. The anterior ethmoidal nerve
and sphenopalatine nerves (Figure 19–3) provide sensory innervation to the
nasal septum and lateral walls. Both can be blocked by packing the nose with
gauze or cotton-tipped applicators soaked with local anesthetic. The topical
anesthetic should be allowed to remain in place at least 10 min before
instrumentation is attempted. Supplementation with submucosal injec-tions of
local anesthetic is often required. Use of an epinephrine-containing solution
or cocaine (usually a 4% or 10% solution) will shrink the nasal mucosa and
potentially decrease intraoperative blood loss. Intranasal cocaine (maximum
dose, 3 mg/kg) is rap-idly absorbed (reaching peak levels in 30 min) and may be
associated with cardiovascular side effects .
General anesthesia is often preferred for
nasal surgery because of the discomfort and incom-plete block that may
accompany topical anesthesia. Special considerations during and shortly
following induction include using an oral airway during face mask ventilation
to mitigate the effects of nasal obstruction; intubating with a reinforced or
pre-formed Mallinckrodt oral RAE® (Ring–Adair–Elwyn)
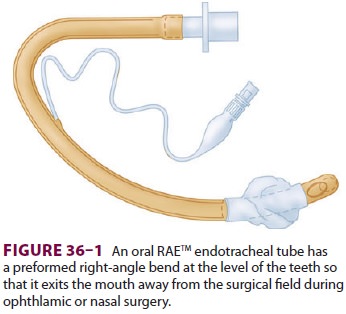
endotracheal tube (Figure 36–1); and tucking
the patient’s padded arms, with protection of the fingers, to the side. Because
of the proximity of the surgical field, it is important to tape the patient’s
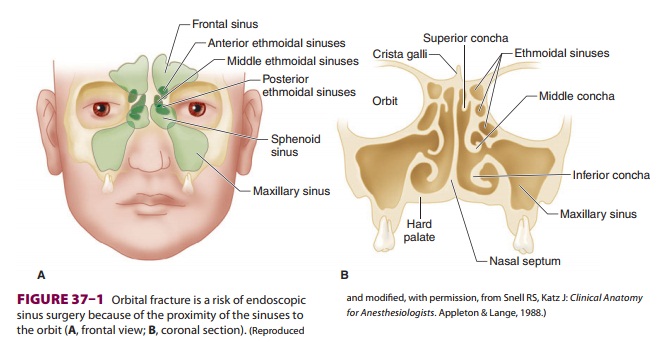
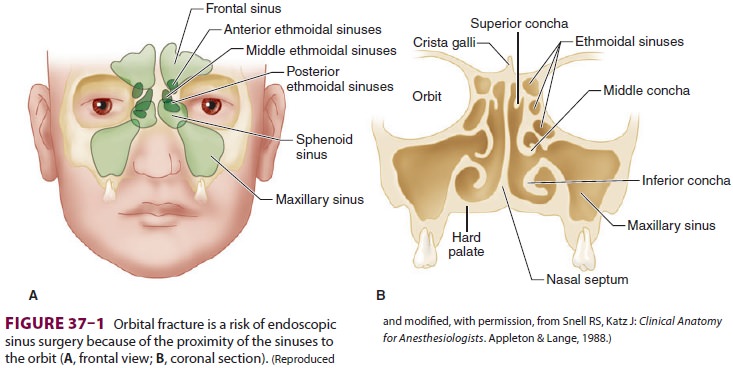
eyes closed to avoid a corneal abrasion. One exception to this occurs during
dissection in endoscopic sinus sur-gery, when the surgeon may wish to
periodically check for eye movement because of the close prox-imity of the
sinuses and orbit (Figure 37–1);
none-theless, the eyes should remain protected until the surgeon is ready to
observe them. NMBs are often utilized because of the potential neurological or
ophthalmic complications that might arise if the patient moves during sinus
instrumentation.Techniques to minimize intraoperative blood loss include
supplementation with cocaineor an epinephrine-containing local
anesthetic, maintaining a slightly head-up position, and pro-viding a mild
degree of controlled hypotension. A posterior pharyngeal pack is often placed
to limit the risk of aspiration of blood. Despite these pre-cautions, the
anesthesiologist must be prepared for major blood loss, particularly during the
resection of vascular tumors (eg, juvenile nasopharyngeal angiofibroma).
Coughing or straining during emergence from anesthesia and extubation
should be avoided, as these events will increase venous pressure and increase
postoperative bleeding. Unfortunately, rela-tively deep extubation strategies
that are commonly and appropriately utilized to accomplish this goal also may
increase the risk of aspiration.
Related Topics