Chapter: Obstetrics and Gynecology: Ectopic Pregnancy and Abortion
Tubal Ectopic Pregnancy: Differential Diagnosis and Procedures
DIFFERENTIAL DIAGNOSIS
Symptoms of ectopic pregnancy can
mimic multiple entities. Early pregnancy complications (threatened, incomplete,
or missed abortion), placental polyp, or hemorrhagic corpus luteal cyst are
difficult to diagnose. Moreover, early bleed-ing occurs in about 20% of women
with normal pregnan-cies. A number of nonpregnancy-related disorders, such as
appendicitis and renal calculi, can mimic ectopic pregnancy.
The rapid
and accurate diagnosis of ectopic pregnancy is imperative to reduce the risk of
serious complications or death. Up to half of the women who have
died as a result of ec-topic pregnancy had a lag in treatment because of
delayed or inaccurate diagnoses. Any sexually active woman in the reproductive
age group who presents with pain, irregular bleeding, and/or amenorrhea should
have ectopic preg-nancy as a part of the initial differential diagnosis.
DIAGNOSTIC PROCEDURES
TVS and serial serum β-hCG measurements are the most
valuable diagnostic aids to confirm the clinical suspicion of an ectopic
pregnancy.
The initial assessment in the
otherwise hemodynam-ically stable patient must include a pregnancy test. A neg-ative
pregnancy test excludes the possibility of ectopic pregnancy. Urinary pregnancy
tests, which detect hCG levels to 20 IU/L, are now commonly available. These
tests detect hCG as early as 14 days after conception and are positive in more
than 90% of cases of ectopic pregnancy. Serum assays can detect the presence of
hCG as early as 5 days after conception, that is, before the missed men-strual
cycle; however, because they require additional time and expertise to perform,
they are often not used in a po-tentially emergent clinical setting.
If a positive pregnancy test is
found when ectopic preg-nancy is suspected, the remainder of the workup should
focus on evaluating the viability and location of the preg-nancy. In normal
pregnancies, serum β-hCG levels
rise in a log-linear fashion until 60 or 80 days after the last menses, at
which time values plateau at about 100,000 IU/L. Dur-ing this period a 66% or
greater increase in serum β-hCG
levels should be observed every 48 hours. Approximately 15% of normal
intrauterine pregnancies are associated with less than a 66% increase in hCG,
and 17% of ectopic pregnancies have normal doubling times. Deviation from this
pattern should raise suspicion for a pregnancy that is not proceeding normally,
including ectopic pregnancy. Although
inappropriately rising serum β-hCG levels suggest (but do not diagnose) an
abnormal pregnancy, they do not iden-tify its location.
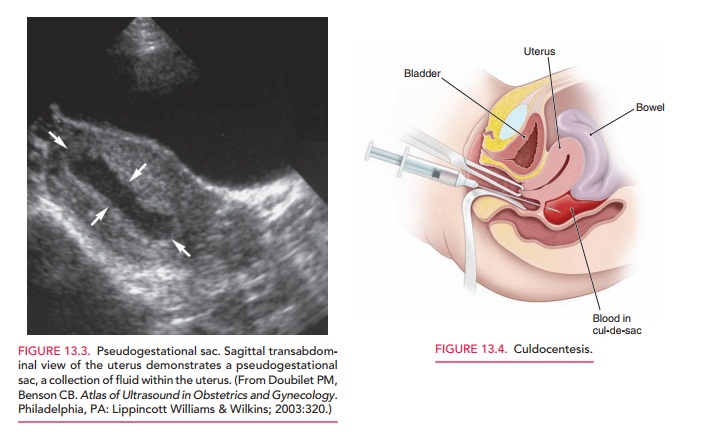
A key adjunct to serial quantitative levels of hCG is pelvic ultrasonography (Fig. 13.2). High-resolution ul-trasonography has revolutionized the clinical manage-ment of women with a suspected ectopic pregnancy. Using TVS, a gestational sac is usually visible between 41⁄2 and 5 weeks from the last menstrual period, the yolk sac appears between 5 and 6 weeks, and a fetal pole with cardiac activity is first detected at 51⁄2 to 6 weeks.
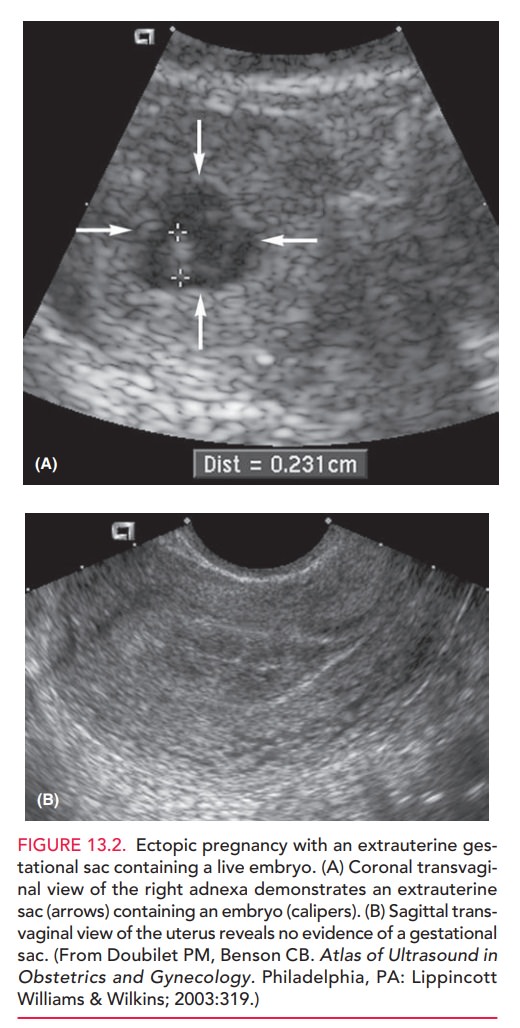
With transabdominal sonography these structures are visualized slightly
later. Each institution must define a β-hCG dis-criminatory
value, that is, the lower limit of hCG atwhich an examiner can reliably
visualize pregnancy on ultrasound. The more sensitive transvaginal
ultrasonogra-phy should show the pregnancy by the time the hCG level is 1000 to
2000 IU/L. Transabdominal ultrasonography should be able to identify an intrauterine
gestation by the time the hCG level reaches 5000 to 6000 IU/L. Accurate
diagnosis by sonography is three times more likely if the initial β-hCG level is above this value.
The absence of uterine pregnancy with β-hCG levels above the discrimi-natory value
signifies an abnormal pregnancy—ectopic, incomplete abortion, or resolving
completed abortion. Care must be taken to differentiate between a uterine
ges-tation and a pseudogestational sac.
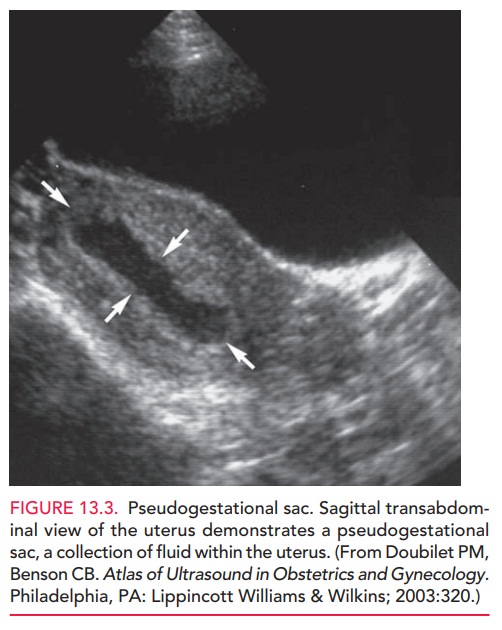
This one-layer sac is the result of an intracavitary fluid collection caused by
sloughing of the decidua typically situated in the midline of the uterine
cavity, whereas a normal gestational sac is eccentrically located (Fig. 13.3).
Serum progesterone concentration has also been used as a screening test for ectopic pregnancy. There is minimal variation in serum progesterone concentration between 5 and 10 weeks’ gestation, thus a single value is sufficient. A serum progesterone level of <5 ng/mL has been used to identify a nonviable pregnancy with near-perfect specificity and with a sensitivity of 60%. Conversely, a serum proges-terone of >20 ng/mL has a sensitivity of 95%, with a speci-ficity of approximately 40% to identify a healthy pregnancy.
Serum
progesterone values cannot differentiate between an ectopic and intrauterine
pregnancy.
Curettage
of the uterine cavity can also help ruleout ectopic
pregnancy but should only be undertaken after the possibility of interrupting
an intact pregnancy has been considered. Although intrauterine and ectopic
pregnancy can exist simultaneously in rare cases (hetero-topic pregnancy),
identification of chorionic villi in tissue samples identifies an intrauterine
location of the preg-nancy and essentially rules out ectopic pregnancy. The
presumptive diagnosis of ectopic pregnancy is reportedly inaccurate in nearly
40% of cases without histologic exclu-sion of a spontaneous pregnancy loss. The
Arias-Stellareaction, a
hypersecretory endometrium of pregnancyseen on histologic examination, occurs
with both ectopic and intrauterine pregnancies and, therefore, is not useful in
identifying an ectopic pregnancy.
Culdocentesis can identify hemoperitoneum (bloodin the peritoneal cavity), which may indicate a ruptured ectopic pregnancy, although it is also consistent with other causes, such as a ruptured corpus luteum cyst. An 18-gauge needle is inserted posterior to the cervix, between the utero-sacral ligaments, and into the cul-de-sac of the peritoneal cavity (Fig. 13.4). Aspiration of clear peritoneal fluid (neg-ative culdocentesis) indicates no hemorrhage into the abdominal cavity but does not rule out an unruptured ectopic pregnancy.
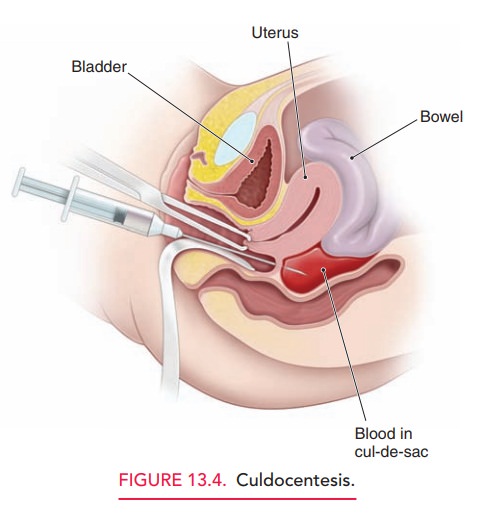
Aspiration of blood that clots can indicate either penetration of a
vessel or such rapid blood loss into the peritoneal cavity that the blood clot
has not had time to undergo fibrinolysis. Nonclotting blood is evidence of
hemoperitoneum (positive culdocentesis), in which the blood clot has undergone
fibrinolysis. If nothing is aspirated (equivocal or nondiagnostic
culdocentesis), no information is obtained. Purulent fluid suggests a num-ber
of infection-related causes, such as salpingitis or appendicitis. Because no
finding on culdocentesis can definitively confirm the presence or absence of
ectopic pregnancy, its use in clinical practice has declined. When used, the
primary utility of culdocentesis is that a positive culdocentesis identifies
blood in the peritoneal cavity and confirms the need for further evaluation to
identify the source of the bleeding.
The most accurate technique of
identifying an ectopic pregnancy is by direct
visualization, which is done most commonly via laparoscopy. Even laparoscopy, however, has a 2% to 5% misdiagnosis
rate. For example, an ex-tremely early tubal gestation may not be identified
because it may not distend the fallopian tube sufficiently to be rec-ognized as
an abnormality (false-negative). Conversely, a false-positive diagnosis may
result from a hematosalpinx (blood
in the fallopian tube) being misinterpreted as an unruptured ectopic pregnancy
or tubal abortion.
Related Topics