Chapter: Medical Surgical Nursing: Community-Based Nursing Practice
The Growing Need for Community-Based Health Care
The Growing Need for Community-Based Health Care
As described, the shift
in the settings for health care delivery is a result of changes in federal
legislation, tighter insur-ance regulations, decreasing hospital revenues, and
the develop-ment of alternative health care delivery systems. As a result of
federal legislation passed in 1983 and 1997, hospitals and other health care
providers are now reimbursed at a fixed rate for pa-tients with the same
diagnosis as defined by diagnosis-related groups. Under this system, hospitals
and other health care providers can cut costs and earn income by carefully
monitoring the types of services they provide and discharging patients as soon
as possible. Consequently, patients are being discharged from acute care
facilities to their homes or to residential or long-term facilities at much
earlier stages of recovery than in the past. Com-plex technical equipment, such
as dialysis machinery, intravenous lines, and ventilators, is often part of
home health care (Brown, 2000).
Alternative health care
delivery systems, such as health main-tenance organizations, preferred provider
organizations, and managed health care systems, have also contributed to the
drive to control costs and the availability of health care services. These
regulations have dramatically reduced the length of hospital stay and have led
to patients being treated more frequently in ambu-latory care settings and at
home.
As more health care
delivery shifts into the community, more nurses are working in a variety of
public health and community-based settings. These settings include public
health departments, ambulatory health clinics, long-term care facilities,
prenatal and well-baby clinics, hospice agencies, industrial settings (as
occu-pational nurses), homeless shelters and clinics, nursing centers, home
health agencies, urgent care centers, same day surgical cen-ters, short-stay
facilities, and patients’ homes.
Nurses in these settings
often deliver care without direct on-site supervision or the support of other
health care personnel. They must be self-directed, flexible, adaptable, and
tolerant of various lifestyles and living conditions. Expertise in independent
decision making, critical thinking, assessment, and health educa-tion, and
competence in basic nursing care are essential to func-tion effectively in the
community-based setting (Brown, 2000; Pierson, 1999).
Community-based nursing
is a philosophy of care of individ-uals and families. The care is provided in a
community as the individual or family move among various kinds of service
pro-viders outside of hospitals (Hunt, 2000). Although the phrase
“community-based nursing” is often interchanged with “commu-nity health
nursing,” a distinction should be made. The phrase “community health nursing”
has generally been equated to “pub-lic health nursing.” Public health nursing
is a specialty focused on total populations, although care may be given to
individuals. Community-based nursing is broader and may incorporate com-munity
health–public health nursing; it is focused on individuals and families rather
than total populations. Community-based nursing also includes home health
nursing, school health nurs
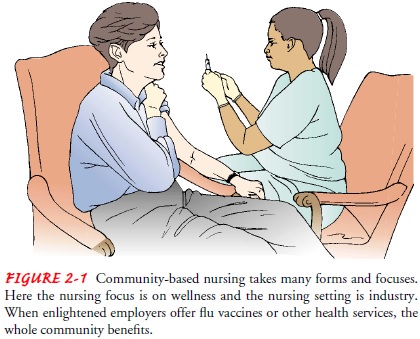
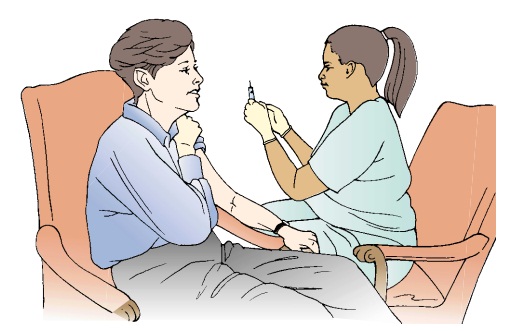
ing, and a host of other
nursing services provided to individuals and groups in the community (Fig.
2-1).
COMMUNITY-BASED CARE
Community-based nursing
practice focuses on promoting and maintaining the health of individuals and
groups, preventing and minimizing the progression of disease, and improving
quality of life (Hunt, 2000). Although nursing interventions used by public
health nurses may involve individuals, families, or small groups, the central
focus remains promotion of health and prevention of dis-ease in the entire
community. The actions of community health nurses may include provision of
direct care to patients and families as well as political advocacy to secure
resources for aggregate pop-ulations (eg, the aged population). The community
health nurse may function as an epidemiologist, a case manager for a group of
patients, a coordinator of services provided to an aggregate of pa-tients, an
occupational health nurse, a school nurse, a visiting nurse, or a parish nurse.
(In parish nursing, the members of the religious community—the parish—are the
recipients of care.) The com-monality of these various roles is that the nurse
maintains a focus on community needs as well as on the needs of the individual
pa-tient. Community-based care is generally focused on the individ-ual or
family; although efforts may be undertaken to improve the health of the whole
community, the individual or family unit is the main focus. The primary
concepts of community-based nursing care are self-care and preventive care
within the context of culture and community. Two other important concepts are
continuity of care and collaboration (Hunt, 2000). Some community-based nursing
fields have become specialties in their own right, such as school health
nursing and home health nursing.
Primary, secondary, and
tertiary levels of preventive care are used by nurses in community-based
practice. The focus of pri-mary prevention is on health promotion and
prevention of illness or disease, including interventions such as teaching
regarding healthy lifestyles (Hunt, 2000). Secondary prevention centers on
health maintenance and is aimed at early detection and prompt intervention to
prevent or minimize loss of function and inde-pendence; it includes
interventions such as health screening and health risk appraisal. Tertiary
prevention focuses on minimizing deterioration and improving quality of life.
Tertiary care may in-clude rehabilitation to assist patients in achieving their
maximum potential by working through their physical or psychological challenges
(Hunt, 2000).
HOME HEALTH CARE
Home health care is
becoming one of the largest practice areas for nurses. Because of the high acuity
level of patients, nurses with acute care and high-technology experience are in
demand in this field. Tertiary preventive nursing care, which focuses on
rehabil-itation and restoring maximum health function, is a major goal for home
care nurses, although primary and secondary preven-tion are also included in
care. Health care visits may be intermit-tent or periodic, and telephonic case
management may be used to promote communication with home care consumers.
Home care nursing is a
unique aspect of community-based nursing. Home care visits are made by nurses
who work for home care agencies, public health agencies, and visiting nurse
associa-tions; by nurses who are employed by hospitals; and by parish nurses
who voluntarily work with the members of their religious communities to promote
health. Such visits may also be part of the responsibilities of school nurses,
clinic nurses, or occupational health nurses. The type of nursing services
provided to patients in their homes varies from agency to agency. Nurses
working for home care or hospice agencies make home visits to provide skilled
nursing care, follow-up care, and teaching to promote health and prevent
complications. Clinic nurses may conduct home visits as part of patient
follow-up. Public health, parish, and school nurses may make visits to provide
anticipatory guidance to high-risk families and follow-up care to patients with
communicable dis-eases. Many home care patients are acutely ill, and many have
chronic health problems and disabilities, requiring nurses to pro-vide more
education and monitoring to the patient and family to facilitate compliance.
Holistic care is
provided in the home through the collabora-tion of a multidisciplinary team
that includes professional nurses; home health aides; social workers; physical,
speech, and occupa-tional therapists; and the physician (Touchard &
Berthelot, 1999). The team provides health and social services with over-sight
of the total health care plan by a case manager, clinical nurse specialist, or
nurse practitioner. Parish nurses may work to pro-vide home care training to
members of their congregations.
Health care services are
provided by official, publicly funded agencies; nonprofit agencies; private
businesses; proprietary chains; and hospital-based agencies. Some agencies
specialize in high-technology services. Most agencies are reimbursed from a
variety of sources, including Medicare and Medicaid programs, private
insurance, and direct payments by patients. Each funding source has its own
requirements for services rendered, number of visits allowed, and amount of
reimbursement the agency will re-ceive. Many home health care expenditures are
financed by Medicare and are affected by provisions of the Balanced Budget Act
of 1997.
The elderly are the most
frequent users of home care services. To be eligible for service, the patient
must be acutely ill, home-bound, and in need of skilled nursing services.
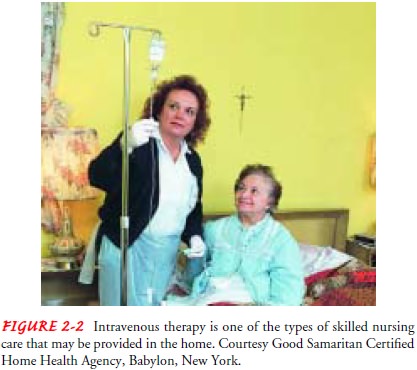
Nursing care in-cludes skilled assessment of the patient’s physical,
psychological, social, and environmental status. Nursing interventions may
in-clude intravenous therapy and injections (Fig. 2-2), parenteral nutrition,
venipuncture, catheter insertion, pressure ulcer treat-ment, wound care, ostomy
care, and patient and family teaching. The nurse instructs the patient and
family in skills and self-care strategies and in health maintenance and
promotion activities (eg, nutritional counseling, exercise programs, stress
management).
Medicare allows nurses
to manage and evaluate patient care for seriously ill patients who have
complex, labile conditions and are at high risk for rehospitalization. The
nurse serves as a casemanager and monitors the delivery of care provided to
patients in their homes.
Related Topics