Chapter: Obstetrics and Gynecology: Sterilization
Sterilization of Men
STERILIZATION OF MEN
About one-third of all surgical
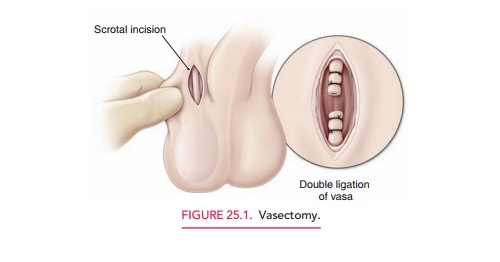
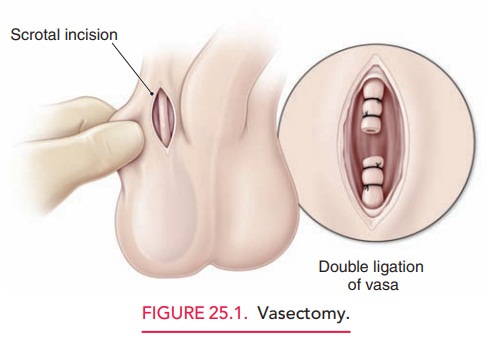
sterilization procedures are performed on men. The technique for vasectomy varies and includes excision
and ligation, electrocautery, and me-chanical or chemical occlusion of the vas
deferens. Because vasectomy is performed outside the abdominal cavity, the
procedure is safer, more easily performed in most cases, less expensive, and
generally more effective than procedures done on women. Vasectomy is also more
easily reversed than most female sterilization procedures (Fig. 25.1). The main
benefit of tubal ligation over vasectomy is immediate sterility.
Minor
postoperative complications occur in 5% to 10% of cases, and include bleeding,
hematomas, acute and chronic pain, and local skin infections. Some
authors report a greater inci-dence of depression and change in body image
after vasec-tomy than after female sterilization. This risk may be minimized
with preoperative counseling and education. Concern has been raised about the
formation of sperm antibodies in approximately 50% of patients, but no ad-verse
long-term effects of vasectomy have been identified. Likewise, concerns about
an increased risk of prostate can-cer following vasectomy are not supported in
literature; in-deed, in countries with the highest rates of vasectomy, there is
no increase in the incidence of prostate cancer.
Pregnancy
after vasectomy occurs in about 1% of cases. Manyof
these pregnancies result from intercourse too soon after the procedure, rather
than from recanalization. Vasectomy is not immediately effective. Multiple
ejaculations are re-quired before the proximal collecting system is emptied of
sperm. Couples should use another method of contracep-tion until male sterility
is reasonably assured or postoper-ative azoospermia is confirmed by semen
analysis (50% at 8 weeks, 100% at 10 weeks postprocedure).
Related Topics