Chapter: Modern Pharmacology with Clinical Applications: Vitamins
Physiological Function and Dietary Sources - Vitamins
PHYSIOLOGICAL
FUNCTION AND DIETARY SOURCES
Vitamins are usually
classified as either fat soluble (vi-tamins A, D, E, and K) or water soluble
(vitamins B and C). The fat-soluble vitamins are generally metabolized slowly
and are stored in the liver. In contrast, the water-soluble vitamins are
rapidly metabolized and are read-ily excreted in the urine.
Fat-Soluble Vitamins
Vitamin A
Vitamin A, or retinol, is
essential for the proper main-tenance of the functional and structural
integrity of ep-ithelial cells, and it plays a major role in epithelial
differentiation. Bone development and growth in children have also been linked
to adequate vitamin A intake. Vitamin A, when reduced to the aldehyde 11-cis-retinal, combines with opsin to
produce the visual pigment rhodopsin. This pigment is present in the rods of
the retina and is partly responsible for the process of dark adaptation.
Principal dietary sources of
vitamin A are milk fat (cheese and butter) and eggs. Since it is stored in the
liver, inclusion of liver in the diet also provides vitamin A. A plant pigment,
carotene, is a precursor for vitamin A and is present in highly pigmented
vegetables, such as carrots, rutabaga, and red cabbage.
An early sign of
hypovitaminosis A is night blind-ness. This condition is related to the role of
vitamin A as the prosthetic group of the visual pigment rhodopsin. The night
blindness may progress to xerophthalmia
(dryness and ulceration of the cornea) and blindness. Other symptoms of vitamin
A deficiency include cessa-tion of growth and skin changes due to
hyperkeratosis.
Since vitamin A is a
fat-soluble vitamin, any disease that results in fat malabsorption and impaired
liver stor-age brings with it the risk of vitamin A deficiency; these
conditions include biliary tract disease, pancreatic dis-ease, sprue, and
hepatic cirrhosis. One group at great risk are children from low-income
families, who are likely to lack fresh vegetables (carotene) and dairy products
(vitamin A) in the diet.
Acute hypervitaminosis A results in drowsiness, headache, vomiting, papilledema, and a bulging fon-tanel in
infants. The symptoms of chronic toxicity in-clude scaly skin, hair loss,
brittle nails, and he-patosplenomegaly. Anorexia, irritability, and swelling of
the bones have been seen in children. Retardation of growth also may occur.
Liver toxicity has been associ-ated with excessive vitamin A intake. Vitamin A
is ter-atogenic in large amounts, and supplements should not be given during a
normal pregnancy. The IOM has re-ported the UL of vitamin A to be 3,000 ÎĽg/day.
Vitamin D
Vitamin D is the collective
term for a group of com-pounds formed by the action of ultraviolet irradiation
on sterols. Cholecalciferol (vitamin D3) and calciferol (vita-min D2)
are formed by irradiation of the provitamins 7-dehydrocholesterol and
ergosterol, respectively. The conversion to vitamin D3 occurs in the
skin. The liver is the principal storage site for vitamin D, and it is here
that the vitamin is hydroxylated to form 25-hydroxyvitamin D. Additional
hydroxylation to form 1,25-dihydroxyvita-min D occurs in the kidney in response
to the need for calcium and phosphate.
The principal disorder
associated with inadequate vitamin D intake is rickets. The low blood calcium
and phosphate levels that occur during vitamin D deficiency stimulate
parathyroid hormone secretion to restore cal-cium levels . In children, this
deficiency leads to the formation of soft bones that become de-formed easily;
in adults, osteomalacia results from the removal of calcium from the bone.
Vitamin D deficiency may occur in patients with metabolic disorders, such as
hypoparathyroidism and renal osteodystrophy. The re-quirement for vitamin D is
slightly higher in members of darker-pigmented races, since melanin interferes
with the irradiation that produces vitamin D3 in the skin. People
with limited exposure to the sun may need to supplement vitamin D intake.
The hypercalcemia resulting
from hypervitaminosis D is responsible for toxic symptoms such
as muscle weakness, bone pain,
anorexia, ectopic calcification, hy-pertension, and cardiac arrhythmias.
Toxicity in infants can result in mental and physical retardation, renal
fail-ure, and death.
Vitamin E
Vitamin E is a potent
antioxidant that is capable of pro-tecting polyunsaturated fatty acids from
oxidative breakdown. This vitamin also functions to enhance vita-min A use.
Although several other physiological actions have been suggested, to date no
unifying concept exists to explain these actions. Vitamin E ( -tocopherol) is
found in a variety of foodstuffs, the richest sources be-ing plant oils,
including wheat germ and rice, and the lipids of green leaves.
Deficiency of vitamin E is
characterized by low serum tocopherol levels and a positive hydrogen perox-ide
hemolysis test. This deficiency is believed to occur in patients with biliary,
pancreatic, or intestinal disease that is characterized by excessive
steatorrhea. Prema-ture infants with a high intake of fatty acids exhibit a
deficiency syndrome characterized by edema, anemia, and low tocopherol levels.
This condition is reversed by giving vitamin E.
Prolonged administration of large dosages of vita-min E may result
in muscle weakness, fatigue, headache, and
nausea. This toxicity can be reversed by discontinu-ing the large-dose
supplementation.
Vitamin K
Vitamin K+ activity
is associated with several quinones, including phylloquinone (vitamin K1),
menadione (vita-min K3), and a variety of menaquinones (vitamin K2).
These quinones promote the synthesis of proteins that are involved in the
coagulation of blood. These proteins include prothrombin, factor VII
(proconvertin), factor IX (plasma thromboplastin), and factor X (Stuart
fac-tor). The vitamin K+ quinones are obtained from three major
sources. Vitamin K+ is present in various plants, especially green
vegetables. The mena-quinones that possess vitamin K2 activity are
synthe-sized by bacteria, particularly gram-positive organisms; the bacteria in
the gut of animals produce useful quan-tities of this vitamin. Vitamin K3
is a chemically synthe-sized quinone that possesses the same activity as
vita-min K1.
Vitamin K+ deficiency
results in increased bleeding time. This hypoprothrombinemia may lead to
hemor-rhage from the gastrointestinal tract, urinary tract, and nasal mucosa.
In normal, healthy adults, deficiency is rare. The two groups at greatest risk
are newborn in-fants and patients receiving anticoagulant therapy;
hy-poprothrombinemia preexists in these two groups. Any disease that causes the
malabsorption of fats may lead to deficiency. Inhibition of the growth of
intestinal bac-teria from extended antibiotic therapy will result in de-creased
vitamin K synthesis and possible deficiency.
Toxicity of vitamin K has not been well defined. Jaundice may occur in a newborn if large dosages of vi-tamin K are
given to the mother before birth. Although kernicterus may result, this can be
prevented by using vitamin K.
Water-Soluble Vitamins
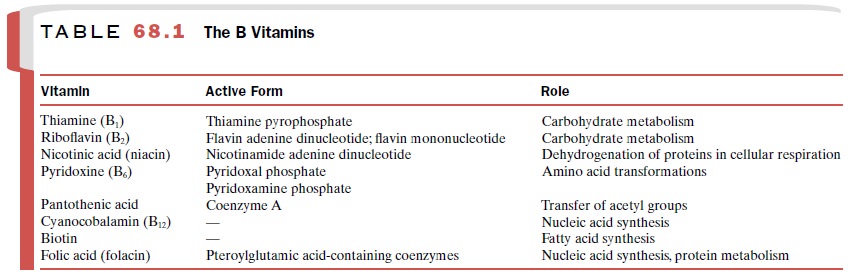
The B Vitamins
The B vitamin group is made
up of substances that tend to occur together in foods and are given the
collective name vitamin B complex. The vitamins of the B group usually have to
be converted to an active form, and most of them play a vital role in
intracellular metabo-lism (Table 68.1). The B vitamins are obtained from both
meat and vegetable products, except for vitamin B12, which occurs
only in animal products. The richest source of the B vitamin group is seeds,
including the germ of wheat or of rice.
The deficiency diseases
associated with the lack of the individual B vitamins are briefly described
next.
Severe thiamine (vitamin B1)
deficiency results in beriberi. The
symptoms can include growth retardation, muscular weakness, apathy, edema, and
heart failure. Neurological symptoms, such as personality changes and mental
deterioration, also may be present in severe cases. Because of the role played
by thiamine in meta-bolic processes in all cells, a mild deficiency may occur
when energy needs are increased. Since thiamine is widely distributed in food,
beriberi is rare except in communities existing on a single staple cereal food.
The disease does occur with some frequency in alcoholics, whose poor diet may
lead to an inadequate daily intake of thiamine.
Riboflavin (vitamin B2) deficiency results in local se-borrheic dermatitis that may be limited to the face and scrotum. Other symptoms of ariboflavinosis include an-gular stomatitis, cheilitis, and glossitis. Specific ocular signs include vascularization of the cornea and keratitis. This deficiency usually occurs in association with defi-ciency of other B complex vitamins.
Niacin or nicotinic acid deficiency produces
the symptoms of pellagra. The
clinical picture progresses from an initial phase of general malaise to
symptoms in-cluding photosensitivity, sore and swollen tongue, gas-tritis, and
diarrhea. Neurological disturbances, depres-sion, and apathy also may occur.
Both niacin and the amino acid tryptophan can be converted to
diphospho-pyridine nucleotide and triphosphopyridine nucleotide. These
reactions require the presence of thiamine, ri-boflavin, and pyridoxine.
Therefore, treatment of the symptoms of pellagra should include, in addition to
B complex vitamin supplementation, an intake of dietary proteins to provide
adequate amounts of tryptophan.
Pyridoxine (vitamin B6) deficiency symptoms are generally expressed as alterations in
the skin, blood, and central nervous system. Symptoms include sensory
neu-ritis, mental depression, and convulsions. Hypochromic, sideroblastic
anemia also may result. Since pyridoxine is required for the conversion of
tryptophan to diphos-phopyridine and triphosphopyridine nucleotides,
pella-gralike symptoms can occur with vitamin B6 deficiency. This
deficiency is found most often in conjunction with other B complex
deficiencies.
The symptoms of pantothenic acid deficiency have not
been clinically described. Since pantothenic acid is a ubiquitous vitamin,
isolated deficiency is unlikely. However, marginal deficiency may exist in
persons with general malnutrition.
Severe cyanocobalamin (vitamin B12)
deficiency re-sults in pernicious
anemia that is characterized by megaloblastic anemia and neuropathies. The
symptoms of this deficiency can be masked by high intake of fo-late. Vitamin B12
is recycled by an effective enterohep-atic circulation and thus has a very long
half-life. Absorption of vitamin B12 from the gastrointestinal tract
requires the presence of gastric intrinsic factor. This factor binds to the
vitamin, forming a complex that can now be absorbed in the terminal ileum. Lack
of this factor results in pernicious anemia. Following a gastrec-tomy, patients
must be given vitamin B12 parenterally. There is no way to determine
how many people have undiagnosed vitamin B12 deficiency. Since
Vitamin B12 is found in almost all animal products, dietary
deficiencies are rare except in some vegan vegetarians who consume no animal
products and need to get their vitamin B12 from a supplement.
However, marginal nutritional lev-els of Vitamin B12 have been
observed in elderly per-sons, demented patients, AIDS patients, and patients
with malignant diseases.
Biotin deficiency is characterized by anorexia, nau-sea,
vomiting, glossitis, depression, and dry, scaly der-matitis. Biotin deficiency
occurs when avidin, a biotin-binding
glycoprotein, is present. Avidin, which is found in raw egg whites, binds the
biotin, making it nutrition-ally unavailable.
Folic acid deficiency symptoms include megaloblas-tic anemia,
glossitis, diarrhea, and weight loss. The re-quirement for this vitamin
increases during pregnancy and lactation.
The effects of most vitamin B overdoses have not been
documented, although large dosages of pyridoxine have been reported to cause
peripheral neuropathies. Ataxia and numbness of the hands and feet and
impairment of the senses of pain, touch, and temperature may result. Excessive
niacin intake may result in flushing, pruritus, and gastrointestinal
disturbances. These symptoms are due to niacin’s ability to cause the release
of histamine. Large dosages of niacin can result in hepatic toxicity.
Vitamin C
Vitamin C (ascorbic acid) is
essential for the mainte-nance of the ground substance that binds cells
together and for the formation and maintenance of collagen. The exact
biochemical role it plays in these functions is not known, but it may be
related to its ability to act as an oxidation–reduction system.
Vitamin C is found in fresh
fruit and vegetables. It is very water soluble, is readily destroyed by heat,
espe-cially in an alkaline medium, and is rapidly oxidized in air. Fruit and
vegetables that have been stored in air, cut or bruised, washed, or cooked may
have lost much of their vitamin C content.
The deficiency disease
associated with a lack of ascorbic acid is called scurvy. Early symptoms
include malaise and follicular hyperkeratosis. Capillary fragility results in
hemorrhages, particularly of the gums. Abnormal bone and tooth development can
occur in growing children. The body’s requirement for vitamin C increases
during periods of stress, such as pregnancy and lactation.
Megavitamin intake of vitamin C may result in diar-rhea due to intestinal
irritation. Since ascorbic acid is partially metabolized and excreted as
oxalate, renal ox-alate stones may form in some patients.
Related Topics